Ureter an Innocent Bystander: Lower Ureteral Stricture Following Angioembolisation of Uterine Artery
Article Information
Tushar Aditya Narain1, Manjeet Kumar2*, Shrawan Singh1, Gopal Sharma1, Shantanu Tyagi1
1Department of Urology, Postgraduate Institute of Medical Education and Research, Chandigarh, India
2Indira Gandhi Medical College and Hospital (IGMC), Shimla, Himachal Pradesh, India
*Corresponding Author: Dr. Manjeet Kumar, Department of Urology, Indira Gandhi Medical College and Hospital (IGMC), Shimla, Himachal Pradesh, India
Received: 24 May 2019; Accepted: 31 May 2019; Published: 10 June 2019
Citation: Tushar Aditya Narain, Manjeet Kumar, Shrawan Singh, Gopal Sharma, Shantanu Tyagi. Ureter an Innocent Bystander: Lower Ureteral Stricture Following Angioembolisation of Uterine Artery. Archives of Nephrology and Urology 2 (2019): 029-032.
Share at FacebookAbstract
Lower ureteric strictures are a common cause for unilateral hydroureteronephrosis, commonly resulting from previous surgeries, weather endoscopic, laproscopic or open. Devascularisation of the ureter resulting in fibrosis forms the underlying pathophysiology of stricture formation. We report a case of ureteral stricture resulting from angioembolization done for a bleeding arteriovenous malformation (AVM) of the uterus.
Keywords
Angioembolisation, Stricture, Ureter
Angioembolisation articles, Stricture articles, Ureter articles
Angioembolisation articles Angioembolisation Research articles Angioembolisation review articles Angioembolisation PubMed articles Angioembolisation PubMed Central articles Angioembolisation 2023 articles Angioembolisation 2024 articles Angioembolisation Scopus articles Angioembolisation impact factor journals Angioembolisation Scopus journals Angioembolisation PubMed journals Angioembolisation medical journals Angioembolisation free journals Angioembolisation best journals Angioembolisation top journals Angioembolisation free medical journals Angioembolisation famous journals Angioembolisation Google Scholar indexed journals Stricture articles Stricture Research articles Stricture review articles Stricture PubMed articles Stricture PubMed Central articles Stricture 2023 articles Stricture 2024 articles Stricture Scopus articles Stricture impact factor journals Stricture Scopus journals Stricture PubMed journals Stricture medical journals Stricture free journals Stricture best journals Stricture top journals Stricture free medical journals Stricture famous journals Stricture Google Scholar indexed journals Ureter articles Ureter Research articles Ureter review articles Ureter PubMed articles Ureter PubMed Central articles Ureter 2023 articles Ureter 2024 articles Ureter Scopus articles Ureter impact factor journals Ureter Scopus journals Ureter PubMed journals Ureter medical journals Ureter free journals Ureter best journals Ureter top journals Ureter free medical journals Ureter famous journals Ureter Google Scholar indexed journals percutaneous nephrostomy articles percutaneous nephrostomy Research articles percutaneous nephrostomy review articles percutaneous nephrostomy PubMed articles percutaneous nephrostomy PubMed Central articles percutaneous nephrostomy 2023 articles percutaneous nephrostomy 2024 articles percutaneous nephrostomy Scopus articles percutaneous nephrostomy impact factor journals percutaneous nephrostomy Scopus journals percutaneous nephrostomy PubMed journals percutaneous nephrostomy medical journals percutaneous nephrostomy free journals percutaneous nephrostomy best journals percutaneous nephrostomy top journals percutaneous nephrostomy free medical journals percutaneous nephrostomy famous journals percutaneous nephrostomy Google Scholar indexed journals computerized tomography articles computerized tomography Research articles computerized tomography review articles computerized tomography PubMed articles computerized tomography PubMed Central articles computerized tomography 2023 articles computerized tomography 2024 articles computerized tomography Scopus articles computerized tomography impact factor journals computerized tomography Scopus journals computerized tomography PubMed journals computerized tomography medical journals computerized tomography free journals computerized tomography best journals computerized tomography top journals computerized tomography free medical journals computerized tomography famous journals computerized tomography Google Scholar indexed journals schistosomiasis articles schistosomiasis Research articles schistosomiasis review articles schistosomiasis PubMed articles schistosomiasis PubMed Central articles schistosomiasis 2023 articles schistosomiasis 2024 articles schistosomiasis Scopus articles schistosomiasis impact factor journals schistosomiasis Scopus journals schistosomiasis PubMed journals schistosomiasis medical journals schistosomiasis free journals schistosomiasis best journals schistosomiasis top journals schistosomiasis free medical journals schistosomiasis famous journals schistosomiasis Google Scholar indexed journals �tuberculosis� articles �tuberculosis� Research articles �tuberculosis� review articles �tuberculosis� PubMed articles �tuberculosis� PubMed Central articles �tuberculosis� 2023 articles �tuberculosis� 2024 articles �tuberculosis� Scopus articles �tuberculosis� impact factor journals �tuberculosis� Scopus journals �tuberculosis� PubMed journals �tuberculosis� medical journals �tuberculosis� free journals �tuberculosis� best journals �tuberculosis� top journals �tuberculosis� free medical journals �tuberculosis� famous journals �tuberculosis� Google Scholar indexed journals Uterine Artery articles Uterine Artery Research articles Uterine Artery review articles Uterine Artery PubMed articles Uterine Artery PubMed Central articles Uterine Artery 2023 articles Uterine Artery 2024 articles Uterine Artery Scopus articles Uterine Artery impact factor journals Uterine Artery Scopus journals Uterine Artery PubMed journals Uterine Artery medical journals Uterine Artery free journals Uterine Artery best journals Uterine Artery top journals Uterine Artery free medical journals Uterine Artery famous journals Uterine Artery Google Scholar indexed journalsArticle Details
1. Introduction
The main cause for ureteral stricture are surgical trauma, impacted ureteral stones, extrinsic compression from a tumor and congenital narrowing. Ureteral stricture is the most frequent complication observed in pelvic surgery. Ureteral strictures are typically due to ischemia, resulting in fibrosis. Wolf and colleagues defined a stricture as ischemic, when it follows open surgery or radiation therapy, whereas a stricture is considered nonischemic if it is caused by spontaneous stone passage or a congenital abnormality [1]. We report a case of ureteral stricture which developed after angioembolisation of bilateral uterine artery done for a bleeding arterio-venous malformation of the uterine cavity.
2. Case Summary
A 24 year old female presented with right flank pain for 3 months. Her medical history revealed sputum positive pulmonary tuberculosis for which she received anti tubercular medication. She also had history of vaginal bleeding, following incomplete abortion, for which suction evacuation was performed. Ultrasonography revealed a mass in the uterus which showed increased vascularity on Doppler examination, suggestive of an arterio-venous malformation. For continuous vaginal bleeding, angiography followed by angioembolisation of AVM was done with PVC beads. She developed right flank pain two months after the angioembolisation. On ultarsonography, patient was found to have right hydroureteronephrosis. On further workup, computerized tomography (CT) scan revealed right hydronephrosis with right hydroureter till lower border of sacroiliac joint. Renal scan suggested decreased right renal function (split function of 18% for the right kidney). Hence, right percutaneous nephrostomy (PCN) was done for urinary diversion, and daily PCN output was 700-900 ml over 24 hours. Patient was investigated for cause of ureteric stricture. Workup for genitourinary tuberculosis, which included urine for acid fast bacilli (AFB), TB-PCR, MTB culture, and cytology for malignancy was negative. It may be noticed here that, the ultrasonography done prior to angiography was normal and ultrasonography done two months after angioembolisation was suggestive of hydronephrosis (Figure 1).
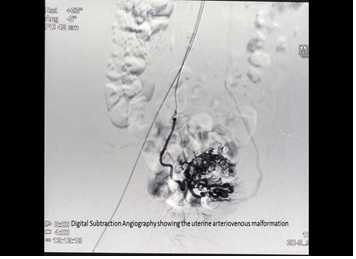
Figure 1: Digital subtraction angiography showing the uterine arteriovenous malformation.
Combined study of nephrostogram and retrograde pyelogram was suggestive of right hydronephrosis with hydroureter with smooth, abrupt tapering at lower border of sacroiliac joint. Urinary bladder and both ureteric orifices were normal on cystoscopy. Urinary bladder capacity was 550 ml. On RGP there was 3 cm complete stricture above right ureteric orifice. No radiological evidence of tuberculosis, could be found. Patient was then planned for an ureteroneocystotomy. Intraoperatively right ureter was found to have a smooth, thin walled, complete stricture of around 4 cm lengths, at the lower border of sacroiliac joint. There were minimal adhesions around ureter and uterus and the adjoining viscera were normal. Right ureteric stricture was resected and ureteroneocystotomy (anti refluxing) with psoas hitch was done. Histopathology of the resected stricture was suggestive of ischemic tissue with no necrosis and/or granuloma. Postoperative nephrostogram and cystogram were performed on 12th postoperative day, which revealed a healed ureterovesical anastomosis with no contrast leak present (Figure 2).
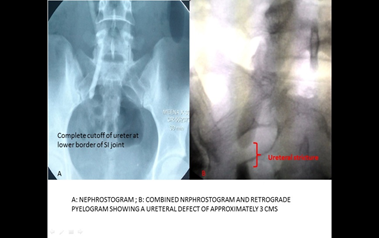
Figure 2: A: Nephrostogram; B: Combined Nephrostogram and retrograde pyelogram showing a ureteral defect of approximately 3 cms.
3. Discussion
Ureteral strictures may be classified as extrinsic or intrinsic, benign or malignant, and iatrogenic or non iatrogenic. Benign intrinsic stricture may be congenital (eg, congenital obstructing megaureter), iatrogenic, or non iatrogenic (e.g., those that follow passage of calculi or chronic inflammatory ureteral involvement [e.g., tuberculosis and schistosomiasis]). Iatrogenic benign strictures may result from previous pelvic surgeries like various gynaecological procedures, for both benign and malignant conditions, radiotherapy for varios malignancies, diagnostic and therapeutic ureteroscopic surgeries and renal transplantation surgeries. Ischemic strictures tend to be associated with fibrosis and scar formation and thus are less likely to respond to endoureterotomy [2-6].
Patients with ureteric strictures present with flank pain, flank fullness, or abdominal fullness or even deterioration of renal function. Diagnosis involves initial evaluation with imaging studies such as ultrasonography or computerized tomography scans which reveal hydroureteronephrosis proximal to the site of stricture. Intravenous pyelography and a retrograde pyelogram would establish the exact location and length of the strictured segment. Indications for intervention in patients with ureteral strictures include pain, infection, or obstruction, which may threaten a patient's renal function. Less common indications may include stone formation proximal to an obstruction or hematuria.
Our patient had a history of angioembolization done for a bleeding arterio venous malformation of the uterus. Angioembolization was done for a branch of the uterine artery, which in turn is a branch of the anterior division of the internal iliac artery. Other branches of the internal iliac artery, arising in close proximity of the uterine artery are the superior vesical, inferior vesical and the middle rectal, all of which contribute to the blood supply of lower part of ureter. Jeopardization of blood supply from any of these branches, during the angioembolization process, may result in ischemia and development of stricture of the lower ureter, as happened in our case.
4. Conclusion
Development of ureteric stricture following surgeries or due to infection like tuberculosis is a common presentation, but that following angioembolization for any reason is unheard off. The clinical presentation of these patients are not straightforward, and a diagnosis cannot be reached unless it is kept in mind that angioembolization for arterio venous malformations of the pelvis can lead to stricture formation in the lower ureter, the basic pathophysiology being ischemia related fibrotic changes and resultant narrowing.
References
- Ramanathan R, Kumar A, Kapoor R, Bhandari M. Relief of urinary tract obstruction in tuberculosis to improve renal function. Analysis of predictive factors. Br J Urol 81 (1998): 199-205.
- Ward AS, Karanjia ND, Russell AJ. Ureteral obstruction following aortobifemoral bypass: management by endoscopic balloon dilation. J Urol 147 (1992): 120-122.
- Tas S, Tugcu V, Mutlu B, Karadag S, et al. Incidence of ureteral stricture after reterorenoscopic pneumatic lithotripsy for distal ureteral calculi. Arch Ital Urol Androl 83 (2011): 141-146.
- Assimos DG, Patterson LC, Taylor CL. Changing incidence and etiology of iatrogenic ureteral injuries. J Urol 152 (1994): 2240-2246.
- Selzman AA, Spirnak JP. Iatrogenic ureteral injuries: a 20-year experience in treating 165 injuries. J Urol 155 (1996): 878-881.
- Wolf JS, Elashry OM, Clayman RV. Long-term results of endoureterotomy for benign ureteral and reteroenteric strictures. J Urol 158 (1997): 759-764.
