Thoracic Idiopathic Scoliosis: Establishing the Diagnostic Accuracy and Reference Values of Surface Topography
Article Information
Isis Juliene Rodrigues Leite Navarro*, Jéssica Secrieru, Cláudia Tarragô Candotti
Physical Education, Physiotherapy and Dance School of Federal University of Rio Grande do Sul (UFRGS), Porto Alegre, Brazil
*Corresponding Author: Isis Juliene Rodrigues Leite Navarro, Physical Education, Physiotherapy and Dance School of Universidade Federal do Rio Grande do Sul (UFRGS), ESEFID/LAPEX/BIOMEC, Rua Felizardo, 750, Porto Alegre, RS, CEP 90690-200, Brazil
Received: 15 June 2019; Accepted: 01 July 2019; Published: 15 July 2019
Citation:
Isis Juliene Rodrigues Leite Navarro, Jéssica Secrieru, Cláudia Tarragô Candotti. Thoracic Idiopathic Scoliosis: Establishing the Diagnostic Accuracy and Reference Values of Surface Topography. Journal of Spine Research and Surgery 1 (2019): 037-047.
Share at FacebookAbstract
Study design: This is a cross-sectional prospective study of diagnostic accuracy.
Objective: The aim of this study was to establish the diagnostic accuracy and cut-off points of the surface topography parameters.
Methods: Seventy-seven participants of both genders, aged between 7 and 18 years old, were consecutively included. Each participant was evaluated using two randomly-chosen consecutive procedures, by means of a surface topography scanner and a Scoliometer®. In this study, the angle of trunk rotation (ATR) determined using the Scoliometer® was taken as reference. For statistical purposes, a multiple linear regression analysis was made to establish which surface topography parameters have the highest standardized beta coefficients (β). Based on the β values, two topographic parameters were chosen (apex of the curve and trunk rotation) to compose the Receiver Operating Characteristic (ROC) analysis.
Results: The cut-off points for the topographic parameters were established as ATR <5° for subjects without scoliosis and ≥8° for severe scoliosis. The ROC curve analysis for the apex of the curve was significant (p<0.001) with an area under the curve (AUC) ranging between 76% [cut-off point 4.4 mm] for the subjects without scoliosis and 84% [cut-off point 9.4 mm] for the subjects with severe scoliosis. For the trunk rotation parameter, the AUC was also significant, ranging between 68% [cut-off point 1.5°, p=0.023] for subjects without scoliosis, and 73% [cut-off point 4.8°, p=0.018] for the subjects with severe scoliosis.
Conclusion: Surface topography provides adequate accuracy and can be used to eval
Keywords
Scoliosis, Adolescent, Surface topography, Linear regression analysis
Scoliosis articles Scoliosis Research articles Scoliosis review articles Scoliosis PubMed articles Scoliosis PubMed Central articles Scoliosis 2023 articles Scoliosis 2024 articles Scoliosis Scopus articles Scoliosis impact factor journals Scoliosis Scopus journals Scoliosis PubMed journals Scoliosis medical journals Scoliosis free journals Scoliosis best journals Scoliosis top journals Scoliosis free medical journals Scoliosis famous journals Scoliosis Google Scholar indexed journals Adolescent articles Adolescent Research articles Adolescent review articles Adolescent PubMed articles Adolescent PubMed Central articles Adolescent 2023 articles Adolescent 2024 articles Adolescent Scopus articles Adolescent impact factor journals Adolescent Scopus journals Adolescent PubMed journals Adolescent medical journals Adolescent free journals Adolescent best journals Adolescent top journals Adolescent free medical journals Adolescent famous journals Adolescent Google Scholar indexed journals Surface topography articles Surface topography Research articles Surface topography review articles Surface topography PubMed articles Surface topography PubMed Central articles Surface topography 2023 articles Surface topography 2024 articles Surface topography Scopus articles Surface topography impact factor journals Surface topography Scopus journals Surface topography PubMed journals Surface topography medical journals Surface topography free journals Surface topography best journals Surface topography top journals Surface topography free medical journals Surface topography famous journals Surface topography Google Scholar indexed journals Linear regression analysis articles Linear regression analysis Research articles Linear regression analysis review articles Linear regression analysis PubMed articles Linear regression analysis PubMed Central articles Linear regression analysis 2023 articles Linear regression analysis 2024 articles Linear regression analysis Scopus articles Linear regression analysis impact factor journals Linear regression analysis Scopus journals Linear regression analysis PubMed journals Linear regression analysis medical journals Linear regression analysis free journals Linear regression analysis best journals Linear regression analysis top journals Linear regression analysis free medical journals Linear regression analysis famous journals Linear regression analysis Google Scholar indexed journals non-invasive technology articles non-invasive technology Research articles non-invasive technology review articles non-invasive technology PubMed articles non-invasive technology PubMed Central articles non-invasive technology 2023 articles non-invasive technology 2024 articles non-invasive technology Scopus articles non-invasive technology impact factor journals non-invasive technology Scopus journals non-invasive technology PubMed journals non-invasive technology medical journals non-invasive technology free journals non-invasive technology best journals non-invasive technology top journals non-invasive technology free medical journals non-invasive technology famous journals non-invasive technology Google Scholar indexed journals idiopathic scoliosis articles idiopathic scoliosis Research articles idiopathic scoliosis review articles idiopathic scoliosis PubMed articles idiopathic scoliosis PubMed Central articles idiopathic scoliosis 2023 articles idiopathic scoliosis 2024 articles idiopathic scoliosis Scopus articles idiopathic scoliosis impact factor journals idiopathic scoliosis Scopus journals idiopathic scoliosis PubMed journals idiopathic scoliosis medical journals idiopathic scoliosis free journals idiopathic scoliosis best journals idiopathic scoliosis top journals idiopathic scoliosis free medical journals idiopathic scoliosis famous journals idiopathic scoliosis Google Scholar indexed journals scoliotic patients articles scoliotic patients Research articles scoliotic patients review articles scoliotic patients PubMed articles scoliotic patients PubMed Central articles scoliotic patients 2023 articles scoliotic patients 2024 articles scoliotic patients Scopus articles scoliotic patients impact factor journals scoliotic patients Scopus journals scoliotic patients PubMed journals scoliotic patients medical journals scoliotic patients free journals scoliotic patients best journals scoliotic patients top journals scoliotic patients free medical journals scoliotic patients famous journals scoliotic patients Google Scholar indexed journals physicians articles physicians Research articles physicians review articles physicians PubMed articles physicians PubMed Central articles physicians 2023 articles physicians 2024 articles physicians Scopus articles physicians impact factor journals physicians Scopus journals physicians PubMed journals physicians medical journals physicians free journals physicians best journals physicians top journals physicians free medical journals physicians famous journals physicians Google Scholar indexed journals Scoliometer articles Scoliometer Research articles Scoliometer review articles Scoliometer PubMed articles Scoliometer PubMed Central articles Scoliometer 2023 articles Scoliometer 2024 articles Scoliometer Scopus articles Scoliometer impact factor journals Scoliometer Scopus journals Scoliometer PubMed journals Scoliometer medical journals Scoliometer free journals Scoliometer best journals Scoliometer top journals Scoliometer free medical journals Scoliometer famous journals Scoliometer Google Scholar indexed journals
Article Details
1. Introduction
Surface topography is a very useful tool for assessment of the spine and trunk. Based on a non-invasive technology, it allows the measurement of the column curvatures and the asymmetries of body surface [1-3]. Its applicability has been extensively studied since it provides three-dimensional data of the back surface. Moreover, it has the benefit to do not exposure the patients to radiation, like the X-ray examination [1, 3-8]. The idiopathic scoliosis (IS) is a three-dimensional deformity of the spine and the trunk [9], which requires a follow-up by periodic radiographies [2-10]. In this case, it would be an important advance in clinical practice to have the surface topography included by means of a standardizing protocol for diagnostic and follow-up processes of scoliotic patients [3-5]. However, even if surface topography comes to be adopted by health professionals, it shall be emphasized that it is still a complementary tool in the evaluation of the patient, not excluding the importance of radiographies when necessary [6-10].
Currently, what prevents surface topography from being used by the physicians or physiotherapists is the lack of standardization in the protocols. There is no agreement for performing the exam and/or for the interpretation of the data it provides [2, 11]. The topographic examination uses a wide range of parameters to be analyzed by the professionals, making the practicality of the exam are lost in the various data to be interpreted. Besides this, the lack of reference values for the correct and standardized interpretation of the findings raises the subjective character of the evaluation [11, 12]. Another limiting factor is the scarcity of studies that verify the diagnostic accuracy of this tool, which is necessary to predict the precision of this instrument. In this context, the aim of this study was to establish the diagnostic accuracy and cut-off points of the apex of the curve and trunk rotation extracted from surface topography. We hypothesized that surface topography is accurate for evaluation of idiopathic scoliosis determining cut-off points for two topographic parameters.
2. Methods
2.1 Study design
This study was a cross-sectional prospective study for diagnostic test assessment reported to Standards for Reporting Diagnostic Accuracy (STARD) [13].
2.2 Participants
The sample was consecutive of both genders. Eligibility criteria: aged between 7 and 18 years old, with suspicious of idiopathic scoliosis (ATR ≥ 5°), being able to maintain an upright position without help and to have a leg length discrepancy lower than 2 cm. Subjects were excluded if they had undergone surgical intervention of the spine. Sample size was calculated on G*Power 3.1.9.2, using linear multiple regression (fixed model), power of 90%, probabilistic error of 5% and effect size=0.4, resulting in a sample of 75 subjects with 25 subjects per group. Two extra participants were added in case of sample lost. The sample was divided in three groups based on the ATR measured by the Scoliometer®. Group 1: without scoliosis (ATR between 0°-4°); Group 2: mild to moderate scoliosis (ATR between 5°-8°): and Group 3 moderate to severe scoliosis: (ATR above 9°) [14]. Ethical approval was granted by the ethics committee of the university where this study was performed (CAAE 66785817.4.0000.5347). Informed consent was obtained from all individual participants included in the study. The individuals participated if they had agreed to be evaluated and only after their parents have signed the informed consent form prior to the assessments. The participants were identified through social network communication (Facebook, blog, WhatsApp) between June 2017 and April 2018.
2.3 Test methods
Each participant was evaluated using two randomly-chosen consecutive procedures: a surface topography scanner (developed and built in Brazil) and a Scoliometer®. In this study, the angle of trunk rotation (ATR) measured by the Scoliometer® was taken as reference. For both evaluations, the subjects wore adequate clothing, like bathing suits, tank tops and shorts. The evaluator was an experienced physiotherapist (9 years) and specialized in scoliosis assessment.
2.4 Surface topography examination
The subjects were asked to stay in upright position, with the back naked, allowing the visualization of the natal cleft. Four green markers were attached on the reference anatomical landmarks (AL) (C7, PSIS and S1) according Navarro et al. [2]. The subjects were positioned with the back from the equipment, maintaining the upper limbs at the side of the body and the feet and knees together and parallel, but respecting the natural posture of the patient. The distance between the subject and the scanner was not standardized, because the equipment has a calibration system that allow a variation of patient position without change the results (Figure 1a).
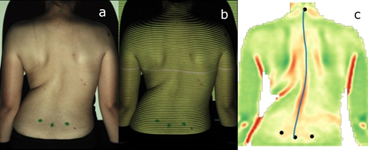
Figure 1: a) References anatomical landmarks; b) Projection of a pattern of structured light; c) Three-dimensional image obtained after the process.
To perform the exam a surface topography scanner called Vert3D version 2 (Miotec Equipamentos Biomédicos Ltda, Brasil) was used. A pattern of structured light was projected on the back of the subject for 2 minutes. The exam was repeated three times with an interval between them determined by the processing time of the system (around 20 seconds) (Figure 1b). After, a second blinded evaluator chose one topographic exam (Figure 1c) to compose the analysis based on the technical quality of the image (light, definition, absence of noise and others). The topographic scanner Vert3D version 2 has a dedicated own software to capture and to analyze the images. The software calculates the topographic parameters based on its own algorithms. The two parameters extracted from surface topography are recommended by SOSORT [15] in the 6th consensus: apex of the curve and trunk rotation (Figure 2).
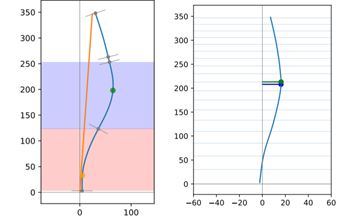
Figure 2: The green point represents the apex of the curve on the left image and the trunk rotation on the right image.
There are no cut-off points values for these two topographic parameters established. Based on the findings of this research, we will may suggest some cut-off points for apex of the curve and trunk rotation measured by means of surface topography.
2.5 Scoliometer examination
The subject was instructed to forward bend the trunk (Adam’s test) while the examiner glided the Scoliometer® on the back surface, keeping the spinous processes touching the cavity indicated in the instrument. From this procedure, it is possible to observe the clinical sign of prominence [16]. The ATR was obtained from the regions of evidence (Figure 3). Furthermore, the examiner identified the vertebral level where the clinical sign was found. The procedure was performed three times and the larger ATR was considered.
The ATR measured by means of Scoliometer® has been described in the literature as a useful parameter for screening and an early detection for spinal deformities. This is a very common tool used among the researchers and clinicians. The cut-off point is usually determined between 5° and 7° [17-20].
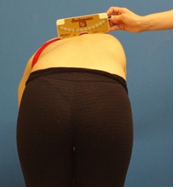
Figure 3: Measurement of the angle of trunk rotation using the Scoliometer®.
2.6 Analysis
There were no indeterminate results or missing data for both Scoliometer® and Surface Topography examinations. The data were analyzed using the Statistical Package for the Social Sciences (SPSS) v. 21.0. Initially, the Kolmogorov-Smirnov test was performed, followed by the descriptive analysis of the data, with measures of central tendencies and dispersion. A multiple linear regression analysis was conducted using a math method “backward”. The ATR provided by the Scoliometer® was the dependent variable and the thirteen parameters measured by means of surface topography were the independent variables.
Based on the highest values of standardized beta coefficients (β) in the model find with regression analysis two topographic parameters were chosen to compose the Receiver Operating Characteristic Curve (ROC curve). The ROC curve was utilized to determine the diagnostic accuracy and to establish the cut-off point for classifying the apex of the curve and trunk rotation using surface topography. The area under the curve (AUC) was classified according to Hanley and McNeil [21] as a poor (0.60 to 0.69), regular (0.70 to 0.79) and excellent (≥ 0.90). The significance level adopted was 0.05.
3. Results
3.1 Participants
The sample is described in the flow diagram (Figure 4) and it was composed of 77 subjects. The subjects were 60% females (n=46) and presented a mean age of 13 ± 3 years old, a mean body mass of 46 ± 15 kg and a mean height of 157 ± 15 cm. The mean ATR obtained through the Scoliometer® was 5° (min 0°-max 30°), the apex of the curve and the trunk rotation obtained through surface topography was 6.6 mm (min-15 mm-max 50 mm) and 3.8° (min 0°-max 28.3°), respectively.
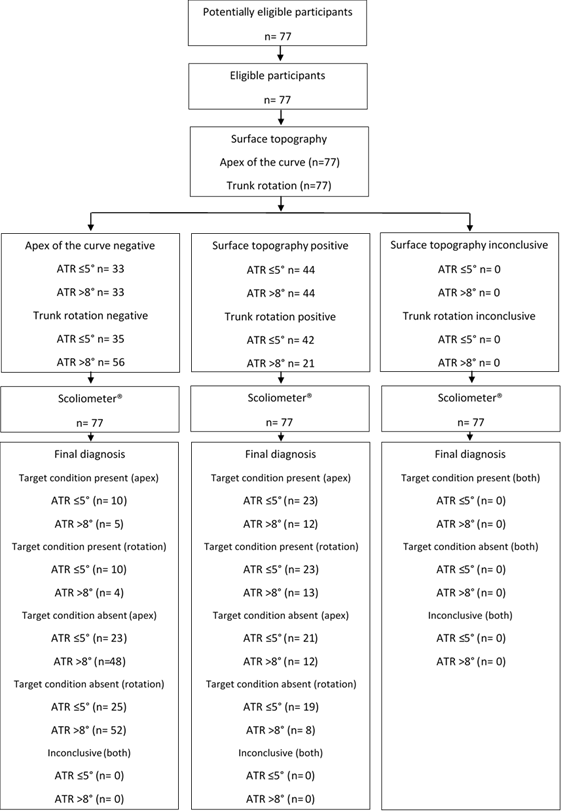
Figure 4: Flow diagram of the participants.
3.2 Test results
The ROC curve showed that, in surface topography, the cut-off point of the apex of the curve to identify the presence of scoliosis is ≥ 4.4 mm and that it is possible to classify the severity of scoliosis. The apex of the curve between 4.4 mm and 9.4 mm indicates mild to moderate scoliosis, whereas the apex of the curve above 9.4 mm indicates moderate to severe scoliosis. For this parameter all cut-off points presented an AUC ≥ 75%, with sensitivity and specificity measures greater than 71% and 67%, respectively (Table 1).
|
ATR |
Surface topography |
Cut-off point |
Sensitivity |
Specificity |
AUC |
|
≤ 5° |
Apex of the curve |
4.4 |
72% |
67% |
0.76** |
|
6° |
4.4 |
82% |
69% |
0.81** |
|
|
7° |
6.6 |
76% |
77% |
0.84** |
|
|
>8° |
9.4 |
71% |
85% |
0.84** |
|
|
≤ 5° |
Trunk rotation |
1.5 |
64% |
69% |
0.68* |
|
6° |
1.5 |
68% |
69% |
0.71* |
|
|
7° |
4.8 |
65% |
93% |
0.73* |
|
|
>8° |
4.8 |
65% |
93% |
0.73* |
ATR: angle of trunk rotation; AUC: area under the curve; *p ≤ 0.05; **p ≤ 0.01
Table 1: Data from the building of the receiver operating characteristics (ROC) curve.
For the parameter trunk rotation, the cut-off point to identify the presence of scoliosis is 1.5°. The trunk rotation between 1.5° and 4.8° indicates mild to moderate scoliosis, whereas the trunk rotation above 4.8° indicates moderate to severe scoliosis. For this parameter all cut-off points presented an AUC ≥ 65%, with sensitivity and specificity measures greater than 64% and 69%, respectively (Table 1).
4. Discussion
A good evaluation tool allows the professional to obtain results with the lowest probability of error possible, and therefore, a standardized protocol and established reference values are so important [11]. In this search, our aim was to establish reference values for the surface topography, which is a non-invasive technology to the assessment of IS. It is well known that the gold standard for the diagnosis and follow-up of IS is the X-ray examination, which provides the visualization of the structure of the spine, however, exposing the patient to a large amount of radiation [1-7, 22]. Whereas the surface topography makes a three-dimensional analysis through the dorsal surface [2, 12], [15], we choose to use the Scoliometer®, an already validated and easy-to-use instrument that also measures ATR across the body surface [12, 23, 24].
The scarcity of studies that validate the surface topography and make it standardized for its use has moved us to study it so that it can be widely used, both in clinical practice and in the scientific environment. In this sense, we seek to adopt a protocol for carrying out the surface topography, observing the two parameters based on the highest values of standardized beta coefficient (β) resulted from a previous regression. These parameters were the angle of trunk rotation and the apex of the curve, which are some of the most used on the other studies [2, 4, 6, 11]. Manca et al. has observed the same pattern with the rastersterography, showing that the highest Pearson’s correlated coefficients were the surface rotation and lateral deviation [11], that in the present study we pointed as trunk rotation and apex of the curve.
Besides determining the diagnostic accuracy of surface topography using two parameters, we identified through the ROC curve the reference values to identify the presence or absence of the scoliosis and classify the severity. We established a cut-off point to a mild to severe curve, for the trunk rotation parameter, on the surface topography, the value 1.5° and 4.8°, respectively, and to the apex of the curve, the values 4.4 mm and 9.4 mm. For that, the values on the Scoliometer® were between 5° and 8º, to classify mild to moderate scoliosis, and above 8° to severe scoliosis. The accuracy of the examination for both the ATR and the apex of the curve was higher in individuals with severe scoliosis than in mild scoliosis, considering values <5° for the absence of scoliosis and ≥ 8° for severe scoliosis, as measured by the Scoliometer®. Some degrees of spinal rotation are more difficult to perceive, since it is a surface measurement [6]. One factor that hinders accuracy of the data is the elevated amount of adiposity and/or muscle mass of the individuals, which can distort the true shape of the spine in the dorsal region [10, 25, 26].
It is of huge clinical importance that other instruments for evaluating scoliosis, other than x-ray, be studied and validated in order to reduce exposure to radiation and the harm brought by it, especially in the period of evolution of the scoliotic curve, that is, in childhood and adolescence [2, 27, 28]. Another positive point in reducing the number of rays is low in environmental pollution, so social factors are also involved in the improvement of the equipment [29]. It is worth mentioning that the surface topography is a complementary instrument to evaluate the IS, does not exclude the need for radiographs eventually, it only reduces their frequency [6, 10]. Knott et al. [10] found that patients with little variation in the curve during the monitoring by the topography can reduce the frequency of x-rays while those that had the highest variation between the tests must be cautious as to decrease the frequency. However, more longitudinal studies should be carried out to verify this statement [6, 10].
Even with the adoption of a standard protocol for surface topography, there are some factors that should be considered for the accuracy of this tool, such as the question of obesity already mentioned, and the experience of the evaluator in the palpation of anatomical markers [10, 12, 25]. Based on Navarro et al. four surface markers are used by the software to evaluate the IS (C7, PSIS and S1) [2]. Therefore, in addition to a well-established protocol with a high correlation with the gold standard of evaluation, training of the evaluator is equally important for a reliable result [10, 25]. Therefore, it is necessary further studies to verify the reproducibility inter and intra-rater and repeatability of this exam. In this study, we limited the verification of the diagnostic accuracy and establishment of reference values for cases of IS in the thoracic region, we recommend that more studies search if the findings will repeat for lumbar and thoracolumbar curvatures. The scarcity of studies that verify the diagnostic accuracy of this tool is considered as a limitation to predict its accuracy.
5. Conclusion
The present study showed that the surface topography is an adequate instrument to identify the presence of idiopathic scoliosis in the thoracic region by two parameters, trunk rotation and apex of the curve, and it can be used in clinical practice. Reference values and cut-off points have been established for both parameters, guided by the values obtained by the Scoliometer®. A standardized protocol is essential for the diagnostic accuracy of any assessment tool, therefore the importance of this study.
Acknowledgments
No acknowledgments to declare.
References
- Don R, Capodaglio P, Cimolin V, et al. Instrumental measures of spinal function: is it worth? A state-of-the art from a clinical perspective. Eur J Phys Rehabil Med 48 (2012): 255-273.
- Navarro I, Rosa BND, Candotti CT. Anatomical reference marks, evaluation parameters and reproducibility of surface topography for evaluating the adolescent idiopathic scoliosis: a systematic review with meta-analysis. Gait Posture 69 (2019): 112-120.
- Goldberg CJ, Kaliszer M, Moore DP, et al. Surface topography, Cobb angles, and cosmetic change in scoliosis. Spine 26 (2001): 55-63.
- Mohokum M, Schulein S, Skwara A. The Validity of Rasterstereography: A Systematic Review. Orthop Rev 7 (2015): 5899.
- Poncet P, Delorme S, Ronsky JL, et al. Reconstruction of laser-scanned 3D torso topography and stereoradiographical spine and rib-cage geometry in scoliosis. Comput Methods Biomech. Biomed Engin 4 (2000): 59-75.
- Schulte TL, Hierholzer E, Boerke A, et al. Raster stereography versus radiography in the long-term follow-up of idiopathic scoliosis. J Spinal Disord Tech 21 (2008): 23-28.
- Ronckers CM, Land CE, Miller JS, et al. Cancer mortality among women frequently exposed to radiographic examinations for spinal disorders. Radiat Res 174 (2010): 83-90.
- Levy AR, Goldberg MS, Hanley JA, et al. Projecting the lifetime risk of cancer from exposure to diagnostic ionizing radiation for adolescent idiopathic scoliosis. Health Phys 66 (1994): 621-633.
- Stokes IA. Three-Dimensional Terminology of Spinal Deformity: A Report Presented to the Scoliosis Research Society by The Scoliosis Research Society Working Group on 3-D Terminology of Spinal Deformity. Spine 19 (1994): 236-248.
- Knott P, Sturm P, Lonner B et al. Multicenter Comparison of 3D Spinal Measurements Using Surface Topography with Those from Conventional Radiography. Spine Deform 4 (2016): 98-103.
- Manca A, Monticone M, Cugusi L, et al. Back surface measurements by rasterstereography for adolescent idiopathic scoliosis: from reproducibility to data reduction analyses. Eur Spine J 27 (2018): 2130-2138.
- Chowanska J, Kotwicki T, Rosadzinski K, et al. School screening for scoliosis: can surface topography replace examination with scoliometer?. Scoliosis 7 (2012): 9.
- Bossuyt PM, Reitsma JB, Bruns DE, et al. STARD 2015: an updated list of essential items for reporting diagnostic accuracy studies. Radiology 277 (2015): 826-832.
- Samuelsson L, Noren L. Trunk rotation in scoliosis the influence of curve type and direction in 150 children. Acta Orthop Scand 68 (1997): 273-276.
- Kotwicki T, Negrini S, Grivas TB, et al. Methodology of evaluation of morphology of the spine and the trunk in idiopathic scoliosis and other spinal deformities-6 th SOSORT consensus paper. Scoliosis 4 (2009): 26.
- Adams W. Lectures on the pathology and treatment of lateral and other forms of curvature of the spine. John Churchill (1865).
- Amendt LE, Ause-Ellias KL, Eybers JL, et al. Validity and reliability testing of the Scoliometer®. Phys Ther 70 (1990): 108-117.
- Cote P, Kreitz BG, Cassidy JD, et al. A study of the diagnostic accuracy and reliability of the Scoliometer and Adam’s forward bend test. Spine 23 (1998): 796-802.
- Huang SC. Cut-off point of the Scoliometer in school scoliosis screening. Spine 22 (1997): 1985-1989.
- De Wilde L, Plasschaert F, Cattoir H, et al. Examination of the back using the Bunnell scoliometer in a Belgian school population around puberty. Acta Orthop Belg 64 (1998): 136-143.
- Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143 (1982): 29-36.
- Stefano Negrini, Sabrina Donzelli, Angelo Gabriele Aulisa, et al. 2016 SOSORT guidelines: orthopaedic and rehabilitation treatment of idiopathic scoliosis during growth. Scoliosis Spinal Disord 13 (2018): 3.
- Bonagamba GH, Coelho DM, De Oliveira AS. Confiabilidade interavaliadores e intra-avaliador do escoliômetro. Rev Bras Fisioter 14 (2010): 432-437.
- Grossman TW, Mazur JM, Cummings RJ. An evaluation of the Adams forward bend test and the scoliometer in a scoliosis school screening setting. J Pediatr Orthop 15 (1995): 535-538.
- Dohnert MB, Tomasi E. Validade da fotogrametria computadorizada na detecção de escoliose idiopática adolescente. Rev Bras Fisioter 12 (2008): 290-297.
- Sedrez JA, Candotti CT, da Rosa MIZ, et al. Validation of a topography system for evaluation spine in sagittal plane for children in different nutrient profiles. Fisioter E Pesqui 23 (2016): 163-171.
- Steve CN Hui, Jean-Philippe Pialasse, Judy YH Wong, et al. Radiation dose of digital radiography (DR) versus micro-dose x-ray (EOS) on patients with adolescent idiopathic scoliosis: 2016 SOSORT-IRSSD ‘John Sevastic Award’ Winner in Imaging Research. Scoliosis Spinal Disord 11 (2016): 46.
- Knott P, Pappo E, Cameron M, et al. SOSORT 2012 consensus paper: reducing x-ray exposure in pediatric patients with scoliosis. Scoliosis 9 (2014): 4.
- Mota SM, de Magalhaes CS, Pordeus IA, et al. Impact of health care waste on man and the environment. Arq Odontol 40 (2004): 159-173.
