The Clinical Study on Short-Term Efficacy of Pelvic Magnetic Stimulation Combined with Pelvic Muscle Biofeedback on Female Idiopathic Overactive Bladder
Article Information
LIU Xiaofang1*, LIN Fang1, LUO Shuang1, LU Zongjie1, HE Quanjiang1, MU Yan1, PENG Qiao1
1Suining central Hospital, Sichuan, Suining 629000, China
*Corresponding author: LIU Xiaofang, Suining central Hospital, Sichuan, Suining 629000, China.
Received: 01 March 2023; Accepted: 06 March 2023; Published: 24 March 2023
Citation: LIU Xiaofang, LIN Fang, LUO Shuang, LU Zongjie, HE Quanjiang, MU Yan, PENG Qiao. The Clinical Study on Short-Term Efficacy of Pelvic Magnetic Stimulation Combined with Pelvic Muscle Biofeedback on Female Idiopathic Overactive Bladder. Journal of Women’s Health and Development 6 (2023): 31-35.
Share at FacebookAbstract
Objective: To evaluate the short-term efficacy of pelvic magnetic stimulation combined with pelvic muscle biofeedback on female Idiopathic Overactive Bladder (IOAB).
Methods: 96 cases of IOAB females were randomly divided into control group (magnetic stimulation treatment n=48) and observation group (magnetic stimulation with biofeedback n=48). All the patients were dealt with the sacralneuromagnetic stimulation (once, qod), with 5 times in total. Then the patients in observation group were processed with biofeedback (10 times). Overactive Bladder Symptom Score (OABSS), Patients Perception Bladder Condition (PPBC) and Incontinence Quality of Life Scale (I-QOL) were evaluated as the indexes.
Results: The effective rate of control group and observation group respectively were 89.58% and 93.75%. There were significant differences (P=0.67). The OABSS and PPBC of two groups were decreased, I-QOL were increased after treatment (P<0.05). Difference was statistically significant in OABSS three months after treatment between the two groups (P=0.00).The recurrence rate of three months after treatment of the two groups were 18.75% and 6.38% (P=0.04).
Conclusions: Both magnetic stimulation alone and magnetic stimulation with biofeedback were effective and safe in female patients with IOAB. Magnetic stimulation with biofeedback may reduce the recurrence rate and continue to improve the symptoms in a certain extent.
Keywords
Biofeedback; Magnetic Stimulation; Overactive Bladder
Biofeedback articles Biofeedback Research articles Biofeedback review articles Biofeedback PubMed articles Biofeedback PubMed Central articles Biofeedback 2023 articles Biofeedback 2024 articles Biofeedback Scopus articles Biofeedback impact factor journals Biofeedback Scopus journals Biofeedback PubMed journals Biofeedback medical journals Biofeedback free journals Biofeedback best journals Biofeedback top journals Biofeedback free medical journals Biofeedback famous journals Biofeedback Google Scholar indexed journals Magnetic Stimulation articles Magnetic Stimulation Research articles Magnetic Stimulation review articles Magnetic Stimulation PubMed articles Magnetic Stimulation PubMed Central articles Magnetic Stimulation 2023 articles Magnetic Stimulation 2024 articles Magnetic Stimulation Scopus articles Magnetic Stimulation impact factor journals Magnetic Stimulation Scopus journals Magnetic Stimulation PubMed journals Magnetic Stimulation medical journals Magnetic Stimulation free journals Magnetic Stimulation best journals Magnetic Stimulation top journals Magnetic Stimulation free medical journals Magnetic Stimulation famous journals Magnetic Stimulation Google Scholar indexed journals Overactive Bladder articles Overactive Bladder Research articles Overactive Bladder review articles Overactive Bladder PubMed articles Overactive Bladder PubMed Central articles Overactive Bladder 2023 articles Overactive Bladder 2024 articles Overactive Bladder Scopus articles Overactive Bladder impact factor journals Overactive Bladder Scopus journals Overactive Bladder PubMed journals Overactive Bladder medical journals Overactive Bladder free journals Overactive Bladder best journals Overactive Bladder top journals Overactive Bladder free medical journals Overactive Bladder famous journals Overactive Bladder Google Scholar indexed journals urinary urgency articles urinary urgency Research articles urinary urgency review articles urinary urgency PubMed articles urinary urgency PubMed Central articles urinary urgency 2023 articles urinary urgency 2024 articles urinary urgency Scopus articles urinary urgency impact factor journals urinary urgency Scopus journals urinary urgency PubMed journals urinary urgency medical journals urinary urgency free journals urinary urgency best journals urinary urgency top journals urinary urgency free medical journals urinary urgency famous journals urinary urgency Google Scholar indexed journals nocturia articles nocturia Research articles nocturia review articles nocturia PubMed articles nocturia PubMed Central articles nocturia 2023 articles nocturia 2024 articles nocturia Scopus articles nocturia impact factor journals nocturia Scopus journals nocturia PubMed journals nocturia medical journals nocturia free journals nocturia best journals nocturia top journals nocturia free medical journals nocturia famous journals nocturia Google Scholar indexed journals muscle articles muscle Research articles muscle review articles muscle PubMed articles muscle PubMed Central articles muscle 2023 articles muscle 2024 articles muscle Scopus articles muscle impact factor journals muscle Scopus journals muscle PubMed journals muscle medical journals muscle free journals muscle best journals muscle top journals muscle free medical journals muscle famous journals muscle Google Scholar indexed journals oversensitivity articles oversensitivity Research articles oversensitivity review articles oversensitivity PubMed articles oversensitivity PubMed Central articles oversensitivity 2023 articles oversensitivity 2024 articles oversensitivity Scopus articles oversensitivity impact factor journals oversensitivity Scopus journals oversensitivity PubMed journals oversensitivity medical journals oversensitivity free journals oversensitivity best journals oversensitivity top journals oversensitivity free medical journals oversensitivity famous journals oversensitivity Google Scholar indexed journals pharmacotherapy articles pharmacotherapy Research articles pharmacotherapy review articles pharmacotherapy PubMed articles pharmacotherapy PubMed Central articles pharmacotherapy 2023 articles pharmacotherapy 2024 articles pharmacotherapy Scopus articles pharmacotherapy impact factor journals pharmacotherapy Scopus journals pharmacotherapy PubMed journals pharmacotherapy medical journals pharmacotherapy free journals pharmacotherapy best journals pharmacotherapy top journals pharmacotherapy free medical journals pharmacotherapy famous journals pharmacotherapy Google Scholar indexed journals rehabilitation articles rehabilitation Research articles rehabilitation review articles rehabilitation PubMed articles rehabilitation PubMed Central articles rehabilitation 2023 articles rehabilitation 2024 articles rehabilitation Scopus articles rehabilitation impact factor journals rehabilitation Scopus journals rehabilitation PubMed journals rehabilitation medical journals rehabilitation free journals rehabilitation best journals rehabilitation top journals rehabilitation free medical journals rehabilitation famous journals rehabilitation Google Scholar indexed journals pelvic organ articles pelvic organ Research articles pelvic organ review articles pelvic organ PubMed articles pelvic organ PubMed Central articles pelvic organ 2023 articles pelvic organ 2024 articles pelvic organ Scopus articles pelvic organ impact factor journals pelvic organ Scopus journals pelvic organ PubMed journals pelvic organ medical journals pelvic organ free journals pelvic organ best journals pelvic organ top journals pelvic organ free medical journals pelvic organ famous journals pelvic organ Google Scholar indexed journals
Article Details
Overactive bladder (OAB) is a syndrome characterized by symptoms of urinary urgency, often with urinary frequency and nocturia, and may be accompanied by urge incontinence [1, 2]. Its urodynamics are often characterized by overactivity of the bladder's forced urinary muscles. The etiology of OAB is unknown, and those with a disease duration of more than six months are called idiopathic OAB, while those with a clear etiology are called secondary OAB. The incidence of OAB is higher in women than in men, and men with OAB are often associated with prostate disease. Furthermore, pelvic floor muscle dysfunction is a particular risk factor for OAB in women, and the causes of OAB in women include overactivity of detrusor muscle and oversensitivity of bladder. Treatments advocated by the International Advisory Committee on Incontinence include behavioral therapy, pharmacotherapy, pelvic floor muscle biofeedback, and magnetic electrical stimulation. However, single-means therapies may have limitations. Single behavioral therapy requires patients to master the correct method and operate consistently. Single-drug therapy is prone to drug tolerance and cannot be applied long-term; pelvic floor muscle biofeedback is difficult to improve OAB caused by overactivity of the detrusor muscle. Magnetic stimulation is an in vitro neuromodulation technique, and magnetic stimulation at the S2-S4S level has been reported to inhibit excessive contraction of the detrusor muscle [3] , but the long-term efficacy needs further validation. As a result, magnetic stimulation and biofeedback training are different therapeutic targets and treatment modalities, and this prospective randomized controlled study was used to observe the short-term efficacy and safety of magnetic stimulation combined with pelvic floor muscle biofeedback.
1. Materials and Methods
1.1 Clinical Data
Ninety-eight patients with OAB treated at our pelvic floor rehabilitation center from January 2019 to January 2020 were grouped by complete randomization using the random number table method according to the inclusion and exclusion criteria. They were divided into control group (magnetic stimulation alone n=48) and observation group (magnetic stimulation combined with biofeedback n=48). (Ethical review approval number: 2016-15)
1.2 Inclusion and Exclusion Criteria
1.2.1 Inclusion Criteria: (1) women over 20 years of age; (2) disease duration of more than 6 months; (3) no relevant medication or physical therapy in the three months prior to being enrolled in this study (4) patients diagnosed with idiopathic OAB according to the International Association of Urological Control guidelines; (5) willing to cooperate to complete treatment and follow-up.
1.2.2 Exclusion Criteria: (1) those with moderate or higher pelvic organ prolapse; (2) patients diagnosed with secondary OAB; (3) those with metal or electronic devices in the body; (4) those with severe heart, liver, or kidney disease. (5) those with a history of epilepsy or Parkinson's disease.
1.3 Apparatus and Methods
1.3.1 Pelvic Floor Magnetic Stimulation: The pelvic floor magnetic stimulation equipment was the MS 080 magnetic stimulator (6.0 Tesla, 80 Hz) from Wuhan Ossef Medical Technology Co., Ltd. During treatment, the patient was placed in a lithotomy position so that the magnetic field of the electromagnetic coil could stimulate the sacrococcygeal nerve. The stimulation intensity was adjusted to just induce the S3 neuroreflex response of bilateral hip wind-like movement and foot toe flexion reflex, the stimulation frequency was 20 Hz, and the single treatment was 4200 pulses for 20 min once every other day.
1.3.2 Pelvic Floor Muscle Biofeedback Treatment: After the end of magnetic stimulation treatment in the observation group patients, the B4plus biostimulation counter was sequentially applied to the pelvic floor muscle biofeedback training by Nanjing McLand Medical Technology Co. Patients were instructed to maintain a semi-recumbent position with both lower limbs slightly abducted and relaxed, vaginal electrodes were inserted, and patients were instructed to contract and relax according to the treatment plan. The patient was instructed to perform contraction and relaxation training according to the treatment plan with 2-3 times per week, and 10 times in total.
1.4 Observation Indexes
1.4.1 Quantitative Indicators: The Overactive Bladder Scale (OABSS) was used as a quantitative diagnostic tool [4]. Patients with urinary urgency symptoms of 2 or more points and an overall OABSS score >3 were diagnosed with OAB; OAB patients were graded for severity: scores ≤5 mild, 6-11 moderate, ≥12 severe. The Patient Perception of Bladder Condition PPBC (PPBC) questionnaire assessed changes in OAB symptoms [5]. Incontinence Quality of Life Questionnaire (I-QOL) was used to assess the quality of life of patients [6].
1.4.2 Clinical Efficacy Indexes: Cured: the patient's symptoms of urinary frequency, urinary urgency and urinary incontinence disappears (the number of urination <8 times in 24h, nocturia <2 times, urine volume >200ml each time). Apparent Effect: the patient's symptoms of urinary frequency and urgency are relieved, and the number of urinary incontinence is reduced by 50%. Ineffective: patients had no relief of symptoms such as urinary frequency and urgency and no reduction in the number of urinary incontinence. Total effective rate = (cured + apparent effect)/total number of cases.
1.4.3 Follow-up: the patients in both groups are followed up by OABSS 3 months after treatment.
1.5 Statistical Methods
SPSS17.0 statistical software was applied for analysis and processing, and the measurement data were expressed as (±s) with t-test or paired t-test. Rates were expressed as percentages (%), and rates were compared using the pearson chi-square test, and the analysis of pre- and post-treatment and follow-up of OABSS in the two groups was performed using SNK ANOVA for comparison between groups and within groups before and after treatment. Differences were considered statistically significant at P < 0.05.
2. Results
2.1 General Information of the Two Groups
There was no statistically significant difference between the two groups in terms of age, pregnancy, delivery and mode of delivery (P > 0.05). (Table 1)
|
Group |
Age |
History of childbirth |
Different mode of delivery |
||
|
Gravida |
Times of childbirth |
Eutocia |
Cesarean delivery |
||
|
Control group |
42.23±9.44 |
3.60±0.58 |
2.42±0.62 |
26 |
22 |
|
Observation group |
41.18±9.47 |
3.84±0.47 |
2.27±0.34 |
23 |
25 |
Table 1: Comparison of the general conditions of the two groups.
2.2 Follow-up Results
There were 96 cases in total. In the observation group, 1 case was terminated due to leaving the treatment place in the middle of the treatment, and the remaining 95 cases completed the treatment and follow-up, and the lost rate was 1%. During the treatment period, one case complained of dizziness after treatment, but the rest did not have any adverse reactions, and the average follow-up time was 3 months.
2.3 Qualitative Efficacy of Two Groups
In the control group, 16 cases were cured, 27 cases had significant effect and 5 cases had no effect among 48 patients, with an effective rate of 89.58%. Among 47 patients in the observation group, 19 were cured, 26 were effective, and 2 were invalid, with an effective rate of 93.75%. There was no statistical difference in the treatment efficiency between the two groups (P=0.67).
2.4 Observation of Quantitative Indexes in the Two Groups
The three indexes of OABSS, PPBC and I-QOL were compared between the two groups of patients before and after treatment (Table 2). The results showed that there was no statistically significant difference between the three indexes of OABSS, PPBC, and I-QOL before treatment between the two groups (P > 0.05); the OABSS score decreased from (9.50 ± 2.56) to (7.32 ± 1.67), PPBC decreased from (4.96 ± 1.12) to (2.13 ± 0.72), and I-QOL decreased from ( 18.80±15.37) to (34.40±12.24), with statistically significant differences (P<0.05). In the observation group, OABSS score decreased from (9.41±2.38) to (7.59±1.47), PPBC decreased from (4.85±1.03) to (1.80±0.75), and I-QOL increased from (20.86± 14.40) to (38.25±13.01), with a statistically significant difference (P<0.05). Using the SNK method, an ANOVA was performed for two-way comparison of OABSS before and after treatment in both groups, and there was a statistically significant difference between the two groups in OABSS scores before treatment, at the end of treatment and at 3 months after treatment (P=0.00). (Table 3)
Table 2: Comparison of observed indicators before and after treatment between two groups of OAB patients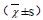 .
.
Notes: OABSS- Overactive Bladder Symptom Score; PPBC- Patient Perception of Bladder Status Questionnaire; I-QOL- Quality of Life Questionnaire for Urinary Incontinence.
|
Group |
Before treatment |
End of treatment |
At 3 months after treatment |
F-value |
P-value |
|
Control group |
9.50±2.56 |
7.32±1.67 |
8.95±1.79 |
7.217 |
0 |
|
Observation group |
9.41±2.38 |
7.59±1.47 |
7.59±1.56 |
7.951 |
0 |
Table 3: Comparison of OABSS scores between and within groups at 3 months after treatment in both groups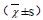 .
.
Note: Analysis of variance between and within groups by SNK method
2.5 Comparison of Recurrence Rates between the Two Groups
Patients were evaluated by OABSS 3 months after treatment in both groups, with 9 recurrence cases in the control group and 3 recurrence cases in the observation group, the recurrence rates in the two groups were 18.75% and 6.38%, respectively, and the difference was statistically significant (P=0.04).
3. Discussion
The pelvic floor musculature, nerves, and fascia form the overall structure of the female pelvic floor, which maintains urination, defecation, and sexual function. Once the overall structure is damaged, it may lead to the development of pelvic floor dysfunctional disorders. Overactive bladder (OAB), on the other hand, is a common abnormality in urinary function, and aging, changes in hormone levels in women, pregnancy and childbirth, and pelvic surgery can exacerbate OAB symptoms [7]. Because the etiology of idiopathic OAB is unknown, the current treatment goal is to improve clinical symptoms, and commonly used noninvasive treatments include pharmacotherapy, behavioral therapy, and Chinese medicine [8, 9,10], but the side effects of long-term pharmacotherapy seriously reduce patients' medication compliance [11]. In the face of patients with refractory OAB, clinicians consider invasive means such as forced urinary muscle toxin injection, sacral nerve electrical stimulation, and tibial nerve electrical stimulation, so as to inhibit nerve reflexes and suppress forced urinary muscle effects [12,13]. As the population ages and people's standard of living improves, more and more female patients want a long-term tolerable and non-invasive way to relieve their symptoms and improve their quality of life [14]. Electrical stimulation or magnetic stimulation has been used clinically to treat patients with OAB and has achieved certain results. Overactive bladder disorder is often associated with instability of the detrusor muscle and increased sensitivity of afferent nerve fibers, and extracorporeal magnetic stimulation uses a high intensity pulsed magnetic field outside the body to stimulate the nerves associated with the pelvic floor innervation, increase the mucosal M receptors at the nerve endings, inhibit the overactivity of the detrusor muscle, and improve the function of the innervated muscles and organs thereby achieving a therapeutic effect [15, 16,17]. Some foreign scholars have proposed that the effect of magnetic stimulation to inhibit the detrusor muscle by stimulating the sacral nerve roots is significantly stronger than that of electrical stimulation [18], which may be related to the physical properties of electrical stimulation, where the current density is highest where the electrodes are in close contact and decays rapidly with the depth of the tissue, and the effect is correspondingly weakened. In 2007, CHOE proposed that the cure rate of patients with OAB treated with magnetic stimulation alone after 2 weeks of treatment could reach 56.3% [19]. In this study, magnetic stimulation combined with biofeedback was observed for the first time in comparison with magnetic stimulation alone, and the results showed that both magnetic stimulation alone and magnetic stimulation combined with biofeedback were significantly effective in the treatment of idiopathic OAB, with an effective rate of 89.58% and 93.75%, respectively, with no statistically significant difference between the two groups (P=0.67). The cure rate of magnetic stimulation alone was 33.33%, which was lower than the results of the CHOE study and may be related to the shorter treatment course in this study. The OABSS, PPBC, and I-QOL indexes were significantly improved at the end of treatment in both groups compared with those before treatment, and the OABSS index was still better than that before treatment at 3 months after treatment (P < 0.05). The difference in OABSS between the two groups at 3 months after treatment was statistically significant (P=0.00), and in terms of the relapse rate at 3 months, the relapse rate in the two groups was 18.75% versus 6.38%, respectively, with a statistically significant difference (P=0.04), indicating that in the short term, magnetic stimulation combined with biofeedback treatment can reduce the relapse rate to a certain extent and is more conducive to sustained symptom improvement.
The present study and related domestic and international studies confirmed that magnetic stimulation was effective in the treatment of OAB, and that extracorporeal magnetic stimulation combined with biofeedback can be the first choice for the clinical treatment of idiopathic OAB because of its non-invasive, safe, and patient-friendly characteristics. Since the follow-up period of this study was relatively short and there were differences in individual behavioral patterns of patients, a larger sample and long-term follow-up are needed to confirm the effectiveness of magnetic stimulation combined with biofeedback on the sustained improvement of symptoms and the recurrence rate of OAB patients.
References
- Haylenbt, De Ridder D, Freeman RM, et al. AnInternationalUrogynecologicalAssociation(IUGA)/InternationalContinenceSociety(ICS)joint report on theterminologyfor female pelvic floor dysfunction[J]. Neurourol Urodyn 29 (2010): 4-20.
- Lee UJ,Scott VC, Rashid R, et al. Defining and managing overactive bladder: disagreement among the experts[J].Urology 81 (2013): 257-262.
- Chancellor MB, Chartier-Kastler EJ. Principles of Sacral Nerve Stimulation (SNS) for the Treatment of Bladder and Urethral Sphincter Dysfunctions. Neuromodulation 3 (2000): 16-26.
- Yamaguehi O, Nishizawa O, Takeda M, et a1.Clinical guidelines for overactive bladder[J].Int J Urol 16 (2009): 126-142.
- Oyne KS, Matza LS, Kopp Z, et a1. The validation of the patient perception of bladder conditionl(PPBC)a single-item global measure for patients with overactive bladder.Eur Urol 49 (2006): 1079-1086.
- Partrick DL, Martin ML, Bushnell DM, et al. Cultural adaptation of a quality of life measure for urinary incontinence[J]. Eur Urol 36 (1999): 427-435.
- Jone HW. The risk of stress incontinence 5 years after first delivery[J].Obste Gynecol Surv 57 (2002): 81-82.
- Osman NI, Chapple CR.Overactive bladder syndrome:current pathophysiological concepts and therapeutic approaches[J].Arab J Urol 11 (2013): 313-318.
- Corcos J, Przydacz M, et a1. CUA guideline on adult overactive bladder[J]. Can Urol As-soc J 11 (2017): 142-173.
- Xiaolong W, Shuang H. Therapeutic effect of warming needle moxibustion on idiopathic overactive bladder in elderly women [J]. Chinese Journal of Gerontology 3 (2016): 1160-1161.
- Sicras PW, Navarro AR, Ruiz TA, et al. Persistence and concomitant medication in patients with overactive bladder treated with antimuscarinic agents in primary care: an observational baseline study[J]. Actas Urol Esp 40 (2016): 96-101.
- Shalom DF, Alamarri N, Xue X, et a1. Sacralnerve stimulation reduces elevated urinary nerve growth factor levels in women with symptomatic detrusor overactivity[J]. Am J Obstet Gynecol 211 (2014): 561-565.
- Guoqing C, Limin L. Application of sacral neuromodulation in neurogenic bladder [J]. Journal of Clinical Surgery 24 (2016): 102-104.
- Yeo EK, Hashim H, Abrams P.New therapies in the treatment of overactive bladder[J].Expert Opin Emerg Drugs 18 (2013): 319-337.
- Yamanishi T, Sakakibara R, Uchiyama T, et a1. Comparative study of the effects of magnetic versus electrical stimulation on inhibition of detrusor over- activity[J].Urology 56 (2000): 777-781.
- Haferkamp A, Dorsam J, Elbadawi A. Ultrastructural diagnosis of neuropathic detrusor overactivity: validation of a common myogenic mechanism[J].Adv Exp Med Biol 539 (2003): 281-291.
- Birder L, Andersson KE. Urothelial signaling[J].PhysiolReviews 93 (2013): 653-680.
- Mcfarlane JP, Foley SJ, De Winter P, et a1. Acute suppression of idiopathic detrusor instability with magnetic stimulation of the sacral nerve roots[J].British J Urol 80 (1997): 734.
- Choe JH, Choo MS, Lee KS.Symptom change in women with overactive bladder after extracorporeal magnetic stimulation:a prospective trial[J].Int Urogynecol J 18 (2007): 875-880.
