Severe Rhino-orbital Mucormycosis Infection of anIntensive Care Unit Patient: A Case Report
Article Information
Ayse Sahin Tutak1*, Huseyin Avni Findikli1 , Sefer Aslan1 , Bilge Aydin Turk2, Mehmet sirik3 and Garip Bekfilavioglu1
Adsyaman University Training and Research Hospital, internal Medicine Department, Adiyaman , Turkey
*Corresponding Authors: Dr. Ayse Sahin Tutak, Adiyaman University Training and Research Hospital, internal Medicine Department, Adiyaman , Turkey
Received: 27 November 2017; Accepted: 08 December 2017; Published: 15 December 2017
Share at FacebookAbstract
Mucormycosis is an opportunistic fungal infection, which is occasionally seen in immunosuppressive patients, and has high morbidity and mortality rates despite treatment. The case is here reported of a patient admitted to our Intensive Care Unit (ICU) with diagnosis of diabetic ketoacidosis, acute kidney injury, acute cerebral infarct and rhino-orbital mucormycosis.This level of advanced rhino-orbital mucormycosis caused severe cutaneous and subcutaneous lesions has not been reported previously in literature and thus the case is evaluated in respect of the early diagnosis of mucormycosis and treatment.
Keywords
Mucormycosis, Acute kidney injury, Rhinocerebral, Cavernous sinus syndrome, Diabetes mellitus
Mucormycosis articles Mucormycosis Research articles Mucormycosis review articles Mucormycosis PubMed articles Mucormycosis PubMed Central articles Mucormycosis 2023 articles Mucormycosis 2024 articles Mucormycosis Scopus articles Mucormycosis impact factor journals Mucormycosis Scopus journals Mucormycosis PubMed journals Mucormycosis medical journals Mucormycosis free journals Mucormycosis best journals Mucormycosis top journals Mucormycosis free medical journals Mucormycosis famous journals Mucormycosis Google Scholar indexed journals Acute kidney injury articles Acute kidney injury Research articles Acute kidney injury review articles Acute kidney injury PubMed articles Acute kidney injury PubMed Central articles Acute kidney injury 2023 articles Acute kidney injury 2024 articles Acute kidney injury Scopus articles Acute kidney injury impact factor journals Acute kidney injury Scopus journals Acute kidney injury PubMed journals Acute kidney injury medical journals Acute kidney injury free journals Acute kidney injury best journals Acute kidney injury top journals Acute kidney injury free medical journals Acute kidney injury famous journals Acute kidney injury Google Scholar indexed journals Rhinocerebral articles Rhinocerebral Research articles Rhinocerebral review articles Rhinocerebral PubMed articles Rhinocerebral PubMed Central articles Rhinocerebral 2023 articles Rhinocerebral 2024 articles Rhinocerebral Scopus articles Rhinocerebral impact factor journals Rhinocerebral Scopus journals Rhinocerebral PubMed journals Rhinocerebral medical journals Rhinocerebral free journals Rhinocerebral best journals Rhinocerebral top journals Rhinocerebral free medical journals Rhinocerebral famous journals Rhinocerebral Google Scholar indexed journals Cavernous sinus syndrome articles Cavernous sinus syndrome Research articles Cavernous sinus syndrome review articles Cavernous sinus syndrome PubMed articles Cavernous sinus syndrome PubMed Central articles Cavernous sinus syndrome 2023 articles Cavernous sinus syndrome 2024 articles Cavernous sinus syndrome Scopus articles Cavernous sinus syndrome impact factor journals Cavernous sinus syndrome Scopus journals Cavernous sinus syndrome PubMed journals Cavernous sinus syndrome medical journals Cavernous sinus syndrome free journals Cavernous sinus syndrome best journals Cavernous sinus syndrome top journals Cavernous sinus syndrome free medical journals Cavernous sinus syndrome famous journals Cavernous sinus syndrome Google Scholar indexed journals Diabetes mellitus articles Diabetes mellitus Research articles Diabetes mellitus review articles Diabetes mellitus PubMed articles Diabetes mellitus PubMed Central articles Diabetes mellitus 2023 articles Diabetes mellitus 2024 articles Diabetes mellitus Scopus articles Diabetes mellitus impact factor journals Diabetes mellitus Scopus journals Diabetes mellitus PubMed journals Diabetes mellitus medical journals Diabetes mellitus free journals Diabetes mellitus best journals Diabetes mellitus top journals Diabetes mellitus free medical journals Diabetes mellitus famous journals Diabetes mellitus Google Scholar indexed journals treatment articles treatment Research articles treatment review articles treatment PubMed articles treatment PubMed Central articles treatment 2023 articles treatment 2024 articles treatment Scopus articles treatment impact factor journals treatment Scopus journals treatment PubMed journals treatment medical journals treatment free journals treatment best journals treatment top journals treatment free medical journals treatment famous journals treatment Google Scholar indexed journals Intensive Care Unit articles Intensive Care Unit Research articles Intensive Care Unit review articles Intensive Care Unit PubMed articles Intensive Care Unit PubMed Central articles Intensive Care Unit 2023 articles Intensive Care Unit 2024 articles Intensive Care Unit Scopus articles Intensive Care Unit impact factor journals Intensive Care Unit Scopus journals Intensive Care Unit PubMed journals Intensive Care Unit medical journals Intensive Care Unit free journals Intensive Care Unit best journals Intensive Care Unit top journals Intensive Care Unit free medical journals Intensive Care Unit famous journals Intensive Care Unit Google Scholar indexed journals diabetic ketoacidosis articles diabetic ketoacidosis Research articles diabetic ketoacidosis review articles diabetic ketoacidosis PubMed articles diabetic ketoacidosis PubMed Central articles diabetic ketoacidosis 2023 articles diabetic ketoacidosis 2024 articles diabetic ketoacidosis Scopus articles diabetic ketoacidosis impact factor journals diabetic ketoacidosis Scopus journals diabetic ketoacidosis PubMed journals diabetic ketoacidosis medical journals diabetic ketoacidosis free journals diabetic ketoacidosis best journals diabetic ketoacidosis top journals diabetic ketoacidosis free medical journals diabetic ketoacidosis famous journals diabetic ketoacidosis Google Scholar indexed journals kidney articles kidney Research articles kidney review articles kidney PubMed articles kidney PubMed Central articles kidney 2023 articles kidney 2024 articles kidney Scopus articles kidney impact factor journals kidney Scopus journals kidney PubMed journals kidney medical journals kidney free journals kidney best journals kidney top journals kidney free medical journals kidney famous journals kidney Google Scholar indexed journals pulmonary articles pulmonary Research articles pulmonary review articles pulmonary PubMed articles pulmonary PubMed Central articles pulmonary 2023 articles pulmonary 2024 articles pulmonary Scopus articles pulmonary impact factor journals pulmonary Scopus journals pulmonary PubMed journals pulmonary medical journals pulmonary free journals pulmonary best journals pulmonary top journals pulmonary free medical journals pulmonary famous journals pulmonary Google Scholar indexed journals
Article Details
1. Introduction
Mucormycosis is the common name given to diseases caused by the Mucorales order of fungi, particularly mucor, rhizopus and absidia, which show a clinical course in the form of organ involvement. Mucorales are saprobic soil organisms, the majority of which are found on rotting organic material and are endemic throughout the world. These organisms become opportunistically pathogenic in individuals with a suppressed immune system, such as in diabetes and ketoacidosis, and can cause acute angio-invasive infections [1, 2].
Mucormycosis can be seen in 6 different forms as rhinocerebral, pulmonary , central nervous system (CNS), gastrointestinal, subcutaneous and occasionally in a disseminated form. Rhinocerebral mucormycosis is the most commonly encountered form and is examined in 3 subgroups of rhino-maxillary, rhino-orbital and rhino-orbitocerebral. Generally the findings and symptoms of rhino-cerebral mucormycosis (RCM) are headache, rhinorrhea, intranasal or intraoral black necrotic areas and epistaxis. As the disease progresses, orbital cellulitis, orbital apex syndrome, cavernous sinus syndrome and CNS involvement may be observed [3].
2. Case
A 61-year old male was found unconscious at home and was brought to the Emergency Department. According to information from the family, he lived alone most of the time despite being a patient needing nursing care. The medical records revealed a diagnosis of diabetes mellitus. At the time of admittance, the patient was unconscious, there were scattered necrotic scars on the left eye and periorbital area, temperature was 39.2°C, blood pressure 75/50 mm Hg, pulse 113 beats/minute, and respiratory rate was 19 breaths/minute with oxygen saturation of 86% on room air. The patient was admitted to the Internal Medicine ICU. The results of the hematological examination on admittance were Hb(hemoglobin): 8.5 g/dL, Htc(hematocrit): 28.3%, WBC (white blood cell count) 21,000/mm, Plt (platelet count): 72 × 104/mm3. Urinalysis showed keton ++, blood chemistry test results showed an elevated blood glucose level of 580 mg/dL, creatinine 4.2 mg/dL, urea: 158 mg/dl , sodium 128 mg/dL, potassium 5.9 mg/dL, arterial blood gas analysis; pH 7.16, HCO3: 12.
As a result of the biochemical tests, the patient was evaluated as acute renal failure (ARF) and diabetic ketoacidosis (DCA). On the requested magnetic resonance imaging (MRI), a wide area compatible with the area irrigated by the left middle cerebral artery (MCA) was evaluated as acute infarct (Figure 1A and 1B), and widespread tissue necrosis was observed in the rhino-orbital region (Figure 2) was consistent with rhino-orbital mucormycosis (ROM). Biopsy material was taken from the necrotic areas and sent to the microbiology laboratory for histopathological examination. The microscopic examination of the biopsy material showed hyphae which were pleomorphic, irregular, thick and branching without septa within the characteristic squamous epithelium and keratin (Figure 3). Treatment was started of intravenous insulin infusion and Amphotericin B 0.3 mg/kg/day and because of the impaired kidney function, there could be no staged dose increase. As the patient had thrombocytopenia and was receiving anticoagulant treatmnt, a limited amount of necrotic tissue debridement could be made. During the follow-up, the DCA recovered and VE ARF partially regressed and the patient was accepted as ex on the 14th day after admission.
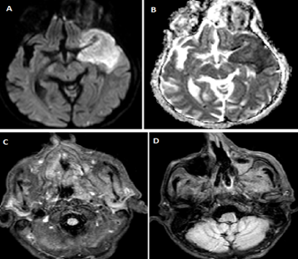
Figure 1 (A, B, C, D): On diffusion weighted images, acute ischaemia with compatible diffusion restriction observed in the left temporal lobe. (A, B). On axial FLAIR images, air-fluid levelling in the left maxillary sinus and hyperintense signal changes were observed compatible with intense oedema secondary to infection in the superficial and deep soft tissue planes in the left hemifacial area (C, D).
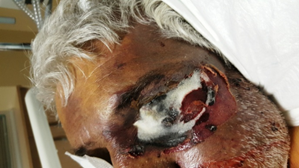
Figure 2: Image showing the tissue necrosis and mold was observed in the rhino-orbital region.
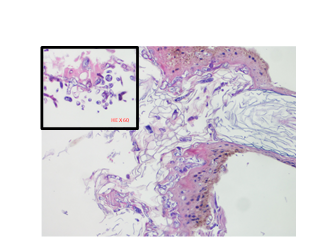
Figure 3: On the haematoxylin and eosin stained preparate (x40-50), hyphae which were pleomorphic, irregular, thick and branching without septa within the characteristic squamous epithelium and keratin.
3. Discussion
Mucormycosis is an opportunistic infection that emerges in immune-compromised patients. Predisposing factors for mucormycosis include uncontrolled diabetes (especially ketoacidosis patients), malignancies such as lymphoma and leukaemia, renal failure, organ transplantations, long-term corticosteroid and immunosuppressive treatment, cirrhosis, protein energy malnutrition and AIDS. Mucormycosis often affects patients with uncontrolled diabetes, and of reported rhino-cerebral mucormycosis cases, 88% have been determined with uncontrolled diabetes and of those, 53.3% with diabetic ketoacidosis [4-7]. The mechanisms held responsible for the more frequent occurrence of mucormycosis in diabetic patients are the reduced iron-binding capacity of transferrin in this patient group and the rapid production of fungi in ketoacidotic and/or hyperglycemic conditions with fungi more easily using iron in the serum to be able to reproduce more quickly, thereby creating a vicious circle with the increased numbers of fungi making more vascular invasion and increasing ischaemia and acidosis [8]. In the currrent case, the predisposing factors for ROM were found together (diabetes, DCA, acute renal failure).
As the reported mortality rate for mucormycosis has been stated in a wide range of 50%-100%, this rate can of course be changed positively with early diagnosis [9]. In the diagnosis of the disease, histopathology or culture are accepted as the gold standard [10]. In the treatment of disease showing an agressive and mortal course, it is recommended that the underlying disease is brought under control, antifungal treatment is administered in addition to surgical debridement, and Amphotericin B is recommended as the prmary antifungal treatment [11]. In the current patient, by providing blood glucose regulation, the DCA was improved and conventional Amphotericin B treatment was started at the same time as the application of surgical debridement. As the disease had a known aggressive and mortal course and because of the comorbidities of ischaemic stroke and acute renal failure, the patient was ex on the 15th day of hospitalisation.
The majority of Mucorales group fungi spread as an agressive focus of infection from the paranasal sinuses to the orbital or cranial area. As they are naturally angiophillic in character, this can lead to early invasion of blood vessels, vascular occlusion, tissue necrosis and ischaemia or haemorrhage [12]. In the current patient, widespread tissue necrosis was observed in the rhino-orbital region, and necrotic scarring filling the intranasal area, the orbital cavity and the sinuses, which was associated with tissue necrosis developing after vascular invasion (Figure 1C, 1D and Figure 2). Although very few cases have been reported in literature [13, 14], even if there are cases of mucormycosis which developed cerebral infarct because of vascular invasion, in the current case there were no cerebral imaging findings or findings of cerebral vascular invasion which could show a reason for the acute ischaemic stroke.
It must be stated that ROM, which is seen in the diabetic patient group in particular, could be a reflection of poor diabetic control, poor socio-economic factors, patient education and low awareness. This case was presented with the aim of reminding that mucormycosis is an opportunistic infection with high morbidity and mortality and of creating a high index of suspicion in clinicians for individuals who have predisposing factors, live alone and neglect their care.
References
- Turhan O, Inan D, Saba R, et al. Rinoserebral mukormikoz: bir olgu sunumu. ANKEM Derg 18 (2004): 228-230.
- Yen M, Baugh W. Rhinocerebral Mucormycosis [Internet],[Place unknown]: Medline Avaliable from: left angle bracket (2011).
- Goldstein EJ, Spellberg B, Walsh TJ, et al. Recent advances in the management of mucormycosis: from bench to bedside. Clinical Infectious Diseases 48 (2009): 1743-1751.
- Solano T, Atkins B, Tambosis E, et al. Disseminated mucormycosis due to Saksenaea vasiformis in an immunocompetent adult. Clin Infect Dis 30 (2000): 942-943.
- Pinto, M.E., et al., Hyperglycemic hyperosmolar state and rhino-orbital mucormycosis. Diabetes Res Clin Pract, 2011. 91(2): p. e37-9.
- Parfrey NA. Improved diagnosis and prognosis of mucormycosis. A clinicopathologic study of 33 cases. Medicine (Baltimore) 65 (1986): 113-123.
- Lee FY, Mossad SB, Adal KA. Pulmonary mucormycosis: the last 30 years. Arch Intern Med 159 (1999): 1301-1309.
- Buchta V, Kalous P, Otcenasek M, et al. Primary cutaneous Absidia corymbifera infection in a premature newborn. Infection 31 (2003): 57-59.
- Goel S, Palaskar S, Shetty VP, et al. Rhinomaxillary mucormycosis with cerebral extension. Journal of oral and maxillofacial pathology: JOMFP 13 (2009): 14.
- Pagano L, Ricci P, Tonso A, et al. Mucormycosis in patients with haematological malignancies: a retrospective clinical study of 37 cases. British journal of haematology 99 (1997): 331-336.
- Saydam L, Erpek G, Kizilay A. Calcified Mucor fungus ball of sphenoid sinus: an unusual presentation of sinoorbital mucormycosis. Annals of Otology, Rhinology & Laryngology 106 (1997): 875-877.
- Mizutari K, Nishimoto K, Ono T. Cutaneous mucormycosis. The Journal of dermatology 26 (1999): 174-177.
- Fu KA, Nguyen PL, Sanossian N. Basilar Artery Territory Stroke Secondary to Invasive Fungal Sphenoid Sinusitis: A Case Report and Review of the Literature. Case Reports in Neurology 7 (2015): 51-58.
- Kumar NS, Padala RK, Tirupati S, et al. Rhinocerebral Mucormycosis with Top of Basilar Artery Syndrome. J Stroke Cerebrovasc Dis 25 (2016): 378-382.
