Seizure Controlled after Laparoscopic Sleeve Gastrectomy Operation: A Case Report of an Obese Epileptic Patient
Article Information
Feng Cao, Chuang Yang, Pengwei Cao, Yanyan Xu*, Yong Wang*
Department of General Surgery, The Second Hospital of Anhui Medical University, Hefei, China
*Corresponding author: Yong Wang, Department of General Surgery, The Second Hospital of Anhui Medical University, Hefei, 230000, China
Yanyan Xu, Department of General Surgery, The Second Hospital of Anhui Medical University, Hefei, 230000, China
Received: 20 July 2020; Accepted: 27 July 2020; Published: 06 August 2020
Citation:
Feng Cao, Chuang Yang, Pengwei Cao, Yanyan Xu, Yong Wang. Seizure Controlled after Laparoscopic Sleeve Gastrectomy Operation: A Case Report of an Obese Epileptic Patient. Archives of Internal Medicine Research 3 (2020): 178-182.
Share at FacebookAbstract
Background: Laparoscopic sleeve gastrectomy(LSG) has been widely used for treating severe obesity, but the recovery of epilepsy after surgery still remained unclear.
Case presentation: We herein described a case of a 31-year-old female obese patient with epilepsy who received laparoscopic sleeve gastrectomy in The Second Hospital of Anhui Medical University in 2018. After follow-up for one year, her body mass index was dropped from 63.9 kg/m2 to 38.6 kg/m2. Besides she had complete seizure remission and had complete freedom from medication. Her electroencephalogram (EEG) records were normal and showed no recurrence of epilepsy.
Conclusions: We believe that the improvement of epilepsy by such surgery further emphasize majority of the researchers, and eventually investigate the relevant and clear underlying mechanism.
Keywords
Bariatric Surgery, LSG, Epilepsy, Case Reports
Article Details
1. Introduction
Since 1975-2016, the global prevalence of obesity (BMI≥30kg/m2) has been dramatically increased. The number of obese people has increased from 100 million to 671 million [1]. Since the first laparoscopic sleeve gastrectomy surgery by Feng et al in 1999 for severely patients with obesity [2], LSG has become widely popularized in clinics. And it has become the main stay of weight reduction surgery now. Epilepsy is a chronic and complex neurological disease. The treatment of epilepsy mainly includes drug therapy, surgical resection of epileptic lesions, and vagus nerve stimulation. Nucleus solitarius (NST) is the main locus of vagus nerve in the brain that accepts most of the afferent vagus nerves [3]. Partial disconnection of the vagus nerve leads to increased vagal excitability, which is in turn transmitted to the NST and its ascending reticular structure, and then down to the amygdala hippocampal complex in the hypothalamus and diffused in the cerebral cortex [4]. We herein reported a case of obese patients with epilepsy who have completely stopped the use of anti-epileptic drugs after LSG.
2. Case Presentation
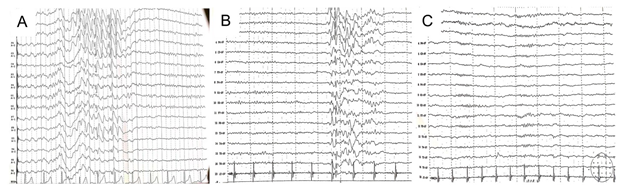
A 31-year-old female patient with morbid obesity for more than 20 years visited our hospital. Her preoperative BMI was 63.9 kg/m2, and had a history of epilepsy for more than 10 years. She was diagnosed with epilepsy at Xuan wu Hospital of Capital Medical University in 2006. The video electroencephalography (VEEG) report indicated abnormal epileptiform discharge in the brain (Figure 1A). She has been taking sodium valproate tablets and phenobarbital tablets for epilepsy for more than 10 years. The dosage of sodium valproate tablets was 0.5g three times a day, and the dosage of phenobarbital tablets was 30mg twice a day. But she had seizures once a week or two. For obesity treatment, the patient received laparoscopic sleeve gastrectomy in the second Affiliated Hospital of Anhui Medical University in March 2018. The patient's preoperative sodium valproate plasma concentration was 58μg/ml (effective range of blood concentration: 50-100 µg/ml), and the blood concentration of phenobarbital was 12μg/ml (effective range of blood concentration: 10-40µg/ml). EEG examination indicated a single high and extra-high potential of 3.6-4.1Hz spinous slow wave was occasionally released in the bilateral cerebral hemisphere during sleep, and it was much more severe in the frontal lobe area, causing epileptic discharge (Figure 1B). The patient continued to take antiepileptic drugs for one month after surgery, but no seizure occurred. The patient was advised to gradually reduce the dose until the drug has been stopped, and there were no epileptic seizures occurred to her either. The BMI one month after surgery has been dropped to 56.4 kg/m 2, 3 months after surgery was 48.2 kg/m 2, after half a year was dropped to 44.5 kg/m 2, and one year after was dropped to 38.6 kg/m 2. In the process of regular follow-up, the patient had stopped antiepileptic drugs for more than a year, and blood concentrations showed very low levels of valproic acid and phenobarbital sodium. Interestingly, we found that no recurrence of seizures and no abnormalities were observed in EEG records (Figure 1C).
Figure 1: Results of electroencephalogram examination at different stages: (A), the video electroencephalography (VEEG) report indicated that there was abnormal epileptiform discharge at Xuan wu Hospital of Capital Medical University in 2006; (B) the electroencephalogram (EEG) suggested epileptic discharge in the second Affiliated Hospital of Anhui Medical University in March 2018; (C) the electroencephalogram records showed no abnormalities in the second Affiliated Hospital of Anhui Medical University in March 2019.
3. Discussion
The principle behind LSG is the use of laparoscopic to cut the stomach big bend vertically, making the stomach to form a small gastric pouch of about 60-80ml. Normally, this weight reduction surgery makes the stomach volume to shrink and reduce the secretion of gastric acid, accelerate gastric emptying and gastrointestinal drug transport [5]. Weight-loss surgery may influence the pharmacokinetics, affecting drug absorption. At present there is no study that has reported the effects of LSG operation on valproic acid and phenobarbital sodium blood drug concentration. The preoperative blood drug concentration of epileptic patient was in effective range with effective blood drug concentration, and she had epileptic seizures once a week or two. One year after the operation, she did not take any drugs, and her blood drug concentration was too low to be measured. Moreover, she did not have any attacks of epilepsy again, the changes of EEG before and after operation inferred improvement in the symptoms of epilepsy, which might be caused due to surgery. When it comes to the mechanism about LSG improving the symptoms of epilepsy, there are no related studies put forwarded so far. We hypothesized that the epilepsy of the patient was improved after surgery, which might possibly be due to the cutoff of some stomach vagus nerves by LSG. The formation of a wide distribution of vagus nerve may be stimulated to improve the seizure basis. Some studies have reported that after stimulation of the vagus nerve, the excitability of the brain is altered through the brain muscarinic receptor-mediated changes, resulting in decreased cortical synchronization and increased norepinephrine secretion [6]. In addition, stimulation of vagus nerve causes the brain stem and cerebral cortex to release gamma-aminobutyric acid (GABA) and glutamate as chemical drivers to regulate human epileptic seizure activity, and plays an anti-epileptic role [7]. Part of epileptic seizures may be caused by inflammation [8]. Previous studies have shown that stimulation of vagus nerve can inhibit the production of inflammatory factors and cytokines such as TNF, IL-1 and IL-6 in the peripheral blood of epileptic patients [9], and the reduction of inflammatory response may also be one of the mechanisms.
4. Conclusion
The postoperative epilepsy symptoms in this case were alleviated without recurrence, and her quality of life was significantly improved. But the specific reasons underlying the success were still unclear. With the gradual promotion of weight loss surgery, more and more obese patients with epilepsy can undergo weight loss surgery. We believe that the improvement of epilepsy by such surgery further emphasize majority of the researchers, and eventually investigate the relevant and clear underlying mechanism.
Ethics Approval and Consent to Participate
The study was approved by the Ethics Committee of Medical Ethics Committee of the Second Affiliated Hospital of Anhui Medical University. All patients were informed of the surgical method and potential adverse events, during the study, and written informed consent was acquired.
Consent for Publication
All authors (Feng Cao, Chuang Yang, Pengwei Cao, Yanyan Xu, Yong Wang) have approved this manuscript.
Availability of Data and Material
All datas are true and reliable.
Funding Sources
The study have no funding sources.
Acknowledgments
We thank Rebecca Porter, PhD, from Liwen Bianji,
Edanz Editing China (www.liwenbianji.cn/ac), for editing the English text of a draft of this manuscript.
Declaration of Interest
The authors have no financial or other conflicts of interest to disclose.
References
- Sung H, Siegel RL, Torre LA, et al. Global patterns in excess body weight and the associated cancer burden. CA Cancer J Clin 69 (2019): 88-112.
- Feng JJ, Gagner M. Laparoscopic biliopancreatic diversion with duodenal switch. Semin Laparosc Surg 9 (2002): 125-129.
- Paton JF, Li YW, Deuchars J, et al. Properties of solitary tract neurons receiving inputs from the sub-diaphragmatic vagus nerve. Neuroscience 95 (2000): 141-153.
- Peyron C, Luppi PH, Fort P, et al. Lower brainstem catecholamine afferents to the rat dorsal raphe nucleus. J Comp Neurol 364 (1996): 402-413.
- Azran C, Wolk O, Zur M, et al. Oral drug therapy following bariatric surgery: an overview of fundamentals, literature and clinical recommendations. Obes Rev 17 (2016): 1050-1066.
- Nichols JA, Nichols AR, Smirnakis SM, et al. Vagus nerve stimulation modulates cortical synchrony and excitability through the activation of muscarinic receptors. Neuroscience 189 (2011): 207-214.
- Bradford HF. Glutamate, GABA and epilepsy. Prog Neurobiol 47 (1995): 477-511.
- Rana A, Musto AE. The role of inflammation in the development of epilepsy. J Neuroinflammation 15 (2018): 144.
- Koopman FA, Chavan SS, Miljko S, et al. Vagus nerve stimulation inhibits cytokine production and attenuates disease severity in rheumatoid arthritis.Proc Natl Acad Sci U S A 113 (2016): 8284-8289.