Relationship between Mortality and Albumin, Alkaline Phosphatase, Phosphorus and Calcium Values that May Change with Renal Function and Nutrition in Intensive Care Setting
Article Information
Ayse Sahin Tutak*
Department of Internal Medicine, Adiyaman University School of Medicine, Adiyaman, Turkey
*Corresponding Author: Ayse Sahin Tutak, Department of Internal Medicine, Adiyaman University School of Medicine, Adiyaman, Turkey
Received: 16 November 2021; Accepted: 26 November 2021; Published: 06 December 2021
Citation: Tutak SA. Relationship between Mortality and Albumin, Alkaline Phosphatase, Phosphorus and Calcium Values that May Change with Renal Function and Nutrition in Intensive Care Setting. Anesthesia and Critical Care 3 (2021): 74-82.
Share at FacebookAbstract
Abstract
Objective
To investigate the relationship between mortality and laboratory values that may change with renal function and nutrition, namely creatinine, ALP, albumin, phosphorus and calcium, in patients admitted to the intensive care unit (ICU).
Method
A total of 2549 patients older than 18 years of age, who were followed up in the ICU of our hospital between 2015-2018, had no history of malignancy or pregnancy, had a length of ICU stay longer than 24 hours, and had laboratory values available at the time of admission to ICU, were included in the study.
Results
The results of our study showed that advanced age and prolonged length of stay are associated with mortality (p<0.001). Low albumin and calcium values and high creatinine and ALP values at the time of ICU admission were a risk factor for mortality (p<0.001). Phosphorus value was not an important risk factor for mortality (p: 0.753).
Conclusion
In ICU patients, the relationship between mortality and renal function and laboratory values that may change with renal function and nutrition, namely creatinine, albumin, calcium, and ALP has been shown while no such relationship was observed between phosphorus values and mortality.
Keywords
Albumin, Alkaline phosphatase (ALP), Calcium; Creatinine, Intensive care unit (ICU), Phosphorus
Albumin articles; Alkaline phosphatase (ALP) articles; Calcium; Creatinine articles; Intensive care unit (ICU) articles; Phosphorus articles
Albumin articles Albumin Research articles Albumin review articles Albumin PubMed articles Albumin PubMed Central articles Albumin 2023 articles Albumin 2024 articles Albumin Scopus articles Albumin impact factor journals Albumin Scopus journals Albumin PubMed journals Albumin medical journals Albumin free journals Albumin best journals Albumin top journals Albumin free medical journals Albumin famous journals Albumin Google Scholar indexed journals Alkaline phosphatase articles Alkaline phosphatase Research articles Alkaline phosphatase review articles Alkaline phosphatase PubMed articles Alkaline phosphatase PubMed Central articles Alkaline phosphatase 2023 articles Alkaline phosphatase 2024 articles Alkaline phosphatase Scopus articles Alkaline phosphatase impact factor journals Alkaline phosphatase Scopus journals Alkaline phosphatase PubMed journals Alkaline phosphatase medical journals Alkaline phosphatase free journals Alkaline phosphatase best journals Alkaline phosphatase top journals Alkaline phosphatase free medical journals Alkaline phosphatase famous journals Alkaline phosphatase Google Scholar indexed journals Calcium articles Calcium Research articles Calcium review articles Calcium PubMed articles Calcium PubMed Central articles Calcium 2023 articles Calcium 2024 articles Calcium Scopus articles Calcium impact factor journals Calcium Scopus journals Calcium PubMed journals Calcium medical journals Calcium free journals Calcium best journals Calcium top journals Calcium free medical journals Calcium famous journals Calcium Google Scholar indexed journals Creatinine articles Creatinine Research articles Creatinine review articles Creatinine PubMed articles Creatinine PubMed Central articles Creatinine 2023 articles Creatinine 2024 articles Creatinine Scopus articles Creatinine impact factor journals Creatinine Scopus journals Creatinine PubMed journals Creatinine medical journals Creatinine free journals Creatinine best journals Creatinine top journals Creatinine free medical journals Creatinine famous journals Creatinine Google Scholar indexed journals Intensive care unit articles Intensive care unit Research articles Intensive care unit review articles Intensive care unit PubMed articles Intensive care unit PubMed Central articles Intensive care unit 2023 articles Intensive care unit 2024 articles Intensive care unit Scopus articles Intensive care unit impact factor journals Intensive care unit Scopus journals Intensive care unit PubMed journals Intensive care unit medical journals Intensive care unit free journals Intensive care unit best journals Intensive care unit top journals Intensive care unit free medical journals Intensive care unit famous journals Intensive care unit Google Scholar indexed journals Phosphorus articles Phosphorus Research articles Phosphorus review articles Phosphorus PubMed articles Phosphorus PubMed Central articles Phosphorus 2023 articles Phosphorus 2024 articles Phosphorus Scopus articles Phosphorus impact factor journals Phosphorus Scopus journals Phosphorus PubMed journals Phosphorus medical journals Phosphorus free journals Phosphorus best journals Phosphorus top journals Phosphorus free medical journals Phosphorus famous journals Phosphorus Google Scholar indexed journals
Article Details
1. Introduction
The mortality rate is the most reliable indicator of performance in intensive care unit (ICU). ICUs serve a seriously ill patient population exposed to a large number of complex interventions. Therefore, ICUs have the highest mortality compared to other departments of any given hospital [1]. Elderly patients admitted to ICU constitute a complicated patient group. More often than not, elderly patients are hospitalized for acute exacerbations of comorbidities as well as underlying chronic diseases and nutritional disorders. Therefore, an increased risk of mortality is expected in older patients [2,3]. In addition, ICU stays tend to be longer and mortal in the elderly. Furthermore, malnutrition, renal dysfunction and electrolyte disorders are common in this group of patients. In the present study, we aimed to investigate the effects of renal function and alkaline phosphatase (ALP) values, which may change with renal dysfunction as well as the effects of albumin, phosphorus and calcium values, which may change with nutrition, on mortality in patients admitted to the ICU.
2. Methods
Our study was conducted among the patients admitted to the Internal Medicine ICU of our hospital between 2015 and 2018. Patients older than 18 years of age were enrolled in the study. Patients, who were pregnant, had a history of malignancy and did not have laboratory data available, were excluded. A total of 2549 patients were included in the study by retrospectively retrieving data from the electronic registry system.
3. Results
Of the 2549 patients included in our study, 48.3% (n=1231) were female while females accounted for 47.3% (n=320) of those with a fatal outcome. Regardless of gender, there was a statistically significant difference between the mean age of the deceased group (76±16 years) and that of survivors (66±36 years) (p<0.001). Again, a statistically significant difference was observed between the deceased (6±12 days) and the survivors (3±5 days) in terms of length of stay (p<0.001). The association of albumin levels showed a statistically significant difference between the group of deceased patients (2.6±0.8 g/dL) and those who survived (3±0.9 g/dL) (p <0.001) (Table 1). ALP values were significantly higher in the deceased group (86±57; p<0.001.). Creatinine values were significantly lower in the group of survivors (0.8±0.3; p<0.001). There was no significant difference between the deceased group and the survivors in terms of phosphorus levels (p=0.753). Calcium levels were lower with a statistically significant difference in the deceased group (8.6±1; p<0.001) (Table 1).
|
Total |
Alive |
Exitus |
P |
||
|
(n=2549) |
(n=1872 %73.45) |
(n=677 %26.55 ) |
|||
|
n (%) |
n (%) |
n (%) |
|||
|
Gender |
|||||
|
Female |
1231 (48,3) |
911 (48,7) |
320 (47,3) |
0,560p |
|
|
Male |
1318 (51,7) |
961 (51,3) |
357 (52,7) |
||
|
n (Median±IQR) |
n (Median±IQR) |
n (Median±IQR) |
|||
|
Age |
2549 (70±28) |
1872 (66±36) |
677 (76±16) |
<0,001u |
|
|
Time of stay hospital |
2549 (3±6) |
1872 (3±5) |
677 (6±12) |
<0,001u |
|
|
Albumin |
2082 (2,9±1) |
1599 (3±0,9) |
483 (2,6±0,8) |
<0,001u |
|
|
ALP |
1860 (80,5±49) |
1393 (78±47) |
467 (86±57) |
<0,001u |
|
|
Creatinine |
1704 (0,8±0,5) |
1287 (0,8±0,3) |
417 (0,9±0,8) |
<0,001u |
|
|
Phosphorus |
1465 (3,5±1,2) |
1092 (3,5±1,2) |
373 (3,5±1,3) |
0,753u |
|
|
Calcium |
1881 (8,8±1) |
1418 (8,9±1) |
463 (8,6±1) |
<0,001u |
|
|
pPearson Chi-Square Test(Exact), u Mann whitney U test(Monte Carlo), IQR: Interquartile Range |
|||||
Table 1: Association of mortality with gender, age and laboratory values (normal ranges of the lab:phosphorus, 2.6-5.5 mg/dL; urea, 10-50 mg/dL; calcium, 8.4-10.8 mg/dL; ALP, 30-128 U/L)
|
Dependent Variable is Mortality |
B |
SE |
P |
OdssRatio |
95,0% CI forOdssRatio |
||
|
Lower |
Upper |
||||||
|
Albumin (↓) |
-0,37169 |
0,12382 |
0,003 |
1,450 |
1,138 |
1,848 |
|
|
ALP |
0,00025 |
0,00042 |
0,553 |
1,000 |
0,999 |
1,001 |
|
|
Creatinine (↑) |
0,20821 |
0,04826 |
<0,001 |
1,231 |
1,120 |
1,354 |
|
|
Calcium |
0,08041 |
0,06430 |
0,211 |
1,084 |
0,955 |
1,229 |
|
|
1 / 2 / 3 / 5 – year survival rates (SE): 68,8 (0.025) / 39,7 (0.037) / 21,1 (0.037) / 6,2 (0,026) - Base Line Hazard: 0,040 Cox Regression-Enter Model, C.I. :Confidence interval B: regression coefficients SE: Standard error |
|||||||
Table 2: Laboratory values associated with mortality
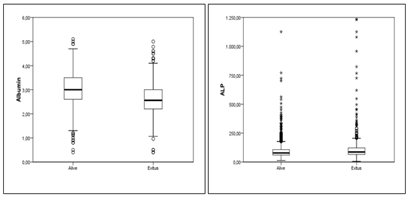
Figures 1,2: Association of albumin and ALP values with mortality.
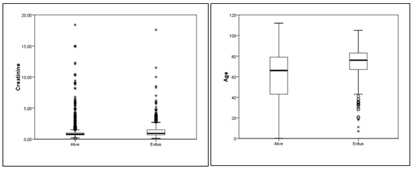
Figures 3,4: Association of creatinine and age with mortality rates
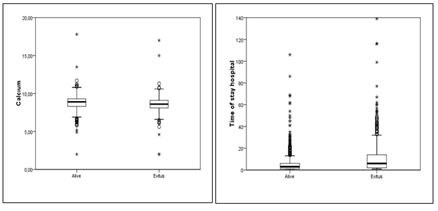
Figures 5,6: Association of calcium and length of stay with mortality rates.
4. Discussion
Mortality rates in the ICU have been reported to vary between 22.5% and 61.5% across different studies [4,5] The mortality rate in our ICU was 26.55%, which is consistent with the literature (Table 1). The parameters investigated as risk factors for ICU mortality in our study were reported, in general, as risk factor in the studies investigating advanced age as a variable [6,7]. In the present study, the mortality rate was statistically significantly higher in patients aged 76 (±16) years or older (p<0.001) (Table 1, Figure 4). Studies investigating the length of hospital stay have reported that length of stay is another parameter associated with mortality [8,9]. Inour study, increased mortality was observed with increasing number of in-hospital days (p<0.001) (Table 1, Figure 6). A number of factors, including age, diet, exercise, stress, pregnancy and kidney disease, may affect serum creatinine levels. Both low creatinine values [10] and high creatinine levels are an independent risk factor for mortality [11] in hospitalized patients. Although it was shown in our study cohort that high creatinine values were an independent risk factor in the deceased group for mortality, consistent with the literature (Tables 1,2 Figure 3), we could not form a different group to demonstrate the effect of low creatinine values on mortality, due to the limited number of patients. Calcium is the most abundant mineral in the human body and has several essential functions. This mineral is involved in vital events such as muscle function, nerve conduction, intracellular signaling and vascular mediation, including contraction and vasodilation [12,13]. In addition, intracellular calcium concentration has an effect on cardiac contractility [14,15]. Abnormal calcium irregularities and changes in serum calcium levels have a prevalence of 88% in clinical practice, especially among critically ill patients [16]. Decreased serum calcium levels correlate with the severity of disease and nutrition [16-18]. Previous studies have shown the effect of serum calcium levels, including hypocalcemia and hypercalcemia, on in-hospital mortality [19]. In our study, calcium levels were lower in the deceased group compared to the survivors; however, the ratio of low calcium values was not at a level to support this parameter as an independent risk factor for mortality (Table 1, Figure 5). The low calcium levels may be due to renal dysfunction as well as malnutrition. Phosphorus is the main substrate of mineralization. Serum phosphorus levels correlate with age and various nutritional markers [20] and it is known that young patients tend to consume more phosphorus [21] while elderly patients are usually hypophosphatemic due to their intake of less phosphorus, often associated with malnutrition [22] In our study, the effect of hypophosphatemia on mortality decreased after adjusting for nutritional markers [23] and this may explain how the relationship between serum phosphorus values and mortality changes with age. However, studies have shown that both hyperphosphatemia (≥7.0 mg/dL) and hypophosphatemia (<3.0 mg/dL) increase mortality rates through a bidirectional effect of serum phosphorus levels on mortality [24];and it has been reported that low phosphorus levels are an important risk factor for increased morbidity and mortality in ICU patients [25]. Phosphorus level was not an independent risk factor for mortality in our patients (Table 1). While we would expect the patients in the deceased group to be hypophosphatemic resulting from malnutrition due to the advanced age, we believe that the reason for the normal phosphorus levels of the patients is the hyperphosphatemia expected in relation to the renal dysfunction in this group, which balances the serum phosphorus levels. Alkaline Phosphatase (ALP) is particularly abundant in the liver, bone, kidney, and placenta [26]. High serum ALP levels are associated with increased mortality in the general population. It is estimated that the pathogenesis between serum ALP values and mortality includes not only high-turnover bone diseases, but also vascular calcification, myocardial contractility disorders, and valvular calcification [27-29]. In our study, ALP values were significantly high in the deceased group (p<0.001); however, it was not an independent risk factor for mortality (Tables 1,2; Figure 2). In our study, we believe that this may be due to high-turnover bone disease due to high creatinine or malnutrition. Albumin, the main component of plasma proteins, maintains microvascular permeability, oncotic pressure, acts as a buffer, transports cations, and plays a role in preventing platelet aggregation [30,31]. In addition to publications showing that serum albumin level has a high sensitivity in predicting ICU mortality, there are publications reporting a low sensitivity in this regard [32-34]. In our study, albumin levels were an independent risk factor for mortality (Table 2) and albumin values were significantly lower in the deceased group compared to survivors (p<0.001) (Table 1, Figure 1). We believe that the hypoalbuminemia in our patients may be related to the severity of disease, renal dysfunction and inadequate nutritional level. In our study investigating the association of mortality with phosphorus, albumin, calcium, and ALP values that can change with renal function and nutrition, we observed albumin and creatinine to be independent risk factors for mortality. In the deceased group, ALP levels were high, while calcium values were low. Consistent with the literature, we concluded that calcium and albumin values, which are related to the nutritional level in ICU patients, are both important parameters for mortality in these patients.
References
- Siddiqui S. Mortality profile across our Intensive Care Units: A 5-year database report from a Singapore restructured hospital. Indian J Crit Care Med 19 (2015): 726-727.
- Unal AU, Kostek O, Takir M, et al. Prognosis of patients in a medical intensive care unit. North Clin Istanbul 2 (2015): 189-195.
- Uysal N, Gundogdu N, Borekci S, et al. Prognosis of Patients in a Medical Intensive Care Unit of a Tertiary Care Centre. Yogun Bakim Derg 1 (2010): 1-5.
- Bueno-Cavanillas A, Delgado-Rodriguez M, Lopez-Luque A, et al. Influence of nosocomialinfection on mortality rate in an intensivecareunit. Crit Care Med 22 (1994): 55-60.
- Akkus NM. Infections seen in Internal Diseases Intensive Care Unit patients: Involved systems, risk factors, causative microorganisms, effects on mortality rate, length of stay and cost. Master thesis. Izmir (1995).
- Craven DE, Kunches LM, Lichtenberg DA, et al. Nosocomial infection and fatality in medical and surgical intensive care unit patients. Arch Intern Med 148 (1988): 1161-1168.
- Leon-Rosales SP, Molinar-Ramos F, Dominguez-Cherit G, et al. Prevalance of infections in intensive care units in Mexico: A multicenter study. Crit Care Med 28 (2000): 1316-1321.
- Craven DE, Kunches LM, Lichtenberg DA, et al. Nosocomial infection and fatality in medical and surgical intensive care unit patients. Arch Intern Med 148 (1988): 1161-1186.
- Vincent JL, Bihari DJ, Suter PM, et al. The prevalence of nosocomial infection in intensive care units in Europe. Results of the European prevalence of Infection in Intensive Care (EPIC) study. JAMA 274 (1995): 639-641.
- Thongprayoon C, Cheungpasitporn W, Kittanamongkolch W. Prognostic importance of low admission serum creatinine concentration for mortality in hospitalized patients. Am J Med 130 (2017): 545-554.
- Cakar MA, Gunduz H, Vatan MB, et al. The effect of admission creatinine levels on one-year mortality in acute myocardial infarction. Scientific World Journal (2012): 186495.
- Beto JA. The Role of Calcium in Human Aging. Clin Nutr Res 4 (2015): 1-8.
- Thongprayoon C, Cheungpasitporn W, Chewcharat A, et al. Hospital mortality and long-term mortality among hospitalized patients with various admission serum ionized calcium levels. Postgrad Med 132 (2020): 385-390.
- Eisner DA, Caldwell J, Kistamás K, et al. Calcium and Excitation-Contraction Coupling in the Heart. Circ Res 121 (2017): 181-195.
- Mc Clellan G, Kulikovskaya I, Winegrad S. Changes in cardiac contractility related to calcium-mediated changes in phosphorylation of myosin-binding protein C. Biophys J 81 (2001): 1083-1092.
- Collage RD, Howell GM, Zhang X, et al. Calcium Supplementation During Sepsis Exacerbates Organ Failure and Mortality via Calcium/Calmodulin-Dependent Protein Kinase Kinase Signaling. Crit Care Med 41 (2013): 352-360.
- Zivin JR, Gooley T, Zager RA, et al. Hypocalcemia: A pervasive metabolic abnormality in the critically ill. Am. J. Kidney Dis 37 (2001): 689-698.
- Israel R. Prevalence and clinical implications of hypocalcemia in acutely ill patients in a medical intensive care setting. J Emerg Med 6 (1988): 558.
- Thongprayoon C, Cheungpasitporn W, Hansrivijit P, et al. Impact of Changes in Serum Calcium Levels on In-Hospital Mortality. Medicina (Kaunas) 56 (2020): 106.
- Verbeke F, Van Biesen W, Honkanen E, et al. Prognostic Value of aortic stiffness and calcification for cardiovascular events and mortality in dialysis patients: outcome of the Calcification Outcome in Renal Disease (CORD) Study. Clin J Am Soc Nephrol 6 (2011):153-159.
- Murtaugh MA, Filipowicz R, Baird BC, et al. Dietary phosphorus intake and mortality in moderate chronic kidney disease: NHANES III. Nephrol Dial Transplant 27 (2012): 990-996.
- Kalantar-Zadeh K, Kuwae N, Regidor DL, et al. Survival predictability of time-varying indicators of bone disease in maintenance hemodialysis patients. Kidney Int 70 (2006): 771-780.
- Nakai S, Akiba T, Kazama J, et al. Effects of serum calcium, phosphorous, and intact parathyroid hormone levels on survival in chronic hemodialysis patients in Japan. Ther Apher Dial 12 (2008):49-54
- Chang JF, Feng YF, Peng YS, et al. Combined Alkaline Phosphatase and PhosphorusLevels as a Predictor of Mortality in Maintenance Hemodialysis Patients. Medicine 93 (2014): 106.
- Inal MT, Memis D, Süt N. Solunum Yetmezlikli Yogun Bakim Hastalarinda Fosfat Düzeyleri. J Turk Soc Intens Care 9 (2011).
- Lomashvili KA, Garg P, Narisawa S, et al. Upregulation of alkaline phosphatase and pyrophosphate hydrolysis: potential mechanism for uremic vascular calcification. Kidney Int 73 (2008): 1024-1030.
- Schoppet M, Shanahan CM. Role for alkaline phosphatase as an inducer of vascular calcification in renal failure?. Kidney Int 73 (2008): 989-991.
- Kovesdy CP, Ahmadzadeh S, Anderson JE, et al. Secondary hyperparathyroidism is associated with higher mortality in men with moderate to severe chronic kidney disease. Kidney Int 73 (2008): 1296-1302.
- Lomashvili KA, Garg P, Narisawa S, et al. Upregulation of alkaline phosphatase and pyrophosphate hydrolysis: Potential mechanism for uremic vascular calcification. Kidney Int 73 (2008): 1024-1030.
- Limaye K, Yang JD, Hinduja A. Role of admission serum albumin levels in patients with intracerebral hemorrhage. Acta Neurologica Belgica 116 (2016): 27-30.
- Nicholson J, Wolmarans M, Park GJ. The role of albumin in critical illness. Br J Anaesth 85 (2000): 599-610.
- Atrash AK, de VasconcellosII K. Low albumin levels are associated with mortality in the critically ill: A retrospective observational study in a multidisciplinary intensive care unit. South Afr j crit care 36 (2020) 74-79.
- Padkins M, Breen T, Anavekar N, et al. Association Between Albumin Level and Mortality Among Cardiac Intensive Care Unit Patients. J Intensive Care Med 36 (2020): 1475-1482.
- Yap FH, Joynt GM, Buckley TA, et al. Association of serum albumin concentration and mortality risk in critically ill patients. Anaesth Intensive Care 30 (2002): 202-207.
