Post-Traumatic Stress Disorder Management in a Patient while Undergoing Fracture Shaft Femur Surgery
Article Information
Debanjan Bose1, Nitu Yadav1*, Nandita Kad1, Manish Yadav2
1Department of Anaesthesia, Pgims Rohtak, India
2Department of Neurosurgery, Pgims Rohtak, India
*Corresponding Author: Nitu Yadav, Department of Anaesthesia, Pgims Rohtak, India
Received: 16 November 2021; Accepted: 06 December 2021; Published: 08 December 2021
Citation: Debanjan Bose, Nitu Yadav, Nandita Kad, Manish Yadav. Post-Traumatic Stress Disorder Management in a Patient while Undergoing Fracture Shaft Femur Surgery. Anesthesia and Critical Care 3 (2021): 83-87.
Share at FacebookAbstract
Post-Traumatic Stress Disorder (PTSD) is a psychiatric disorder that develops after a traumatic event. PTSD in a surgical patient can impact postoperative outcomes. Evidence suggests that the perioperative process can transiently exacerbate PTSD symptoms. Anaesthetist should be aware of its association with cardiovascular dysfunction, chronic pain, depression and cognitive dysfunction. So managing PTSD intraoperatively and trying not to provoke an acute episode perioperatively is extremely challenging for an anaesthetist. Here we are reporting a case of intraoperative onset and management of post-traumatic stress disorder during femur nailing.
Keywords
Post traumatic stress disorder, Anxiety, Management
Post traumatic stress disorder articles; Anxiety articles; Management articles
Post traumatic stress disorder articles Post traumatic stress disorder Research articles Post traumatic stress disorder review articles Post traumatic stress disorder PubMed articles Post traumatic stress disorder PubMed Central articles Post traumatic stress disorder 2023 articles Post traumatic stress disorder 2024 articles Post traumatic stress disorder Scopus articles Post traumatic stress disorder impact factor journals Post traumatic stress disorder Scopus journals Post traumatic stress disorder PubMed journals Post traumatic stress disorder medical journals Post traumatic stress disorder free journals Post traumatic stress disorder best journals Post traumatic stress disorder top journals Post traumatic stress disorder free medical journals Post traumatic stress disorder famous journals Post traumatic stress disorder Google Scholar indexed journals Anxiety articles Anxiety Research articles Anxiety review articles Anxiety PubMed articles Anxiety PubMed Central articles Anxiety 2023 articles Anxiety 2024 articles Anxiety Scopus articles Anxiety impact factor journals Anxiety Scopus journals Anxiety PubMed journals Anxiety medical journals Anxiety free journals Anxiety best journals Anxiety top journals Anxiety free medical journals Anxiety famous journals Anxiety Google Scholar indexed journals Management articles Management Research articles Management review articles Management PubMed articles Management PubMed Central articles Management 2023 articles Management 2024 articles Management Scopus articles Management impact factor journals Management Scopus journals Management PubMed journals Management medical journals Management free journals Management best journals Management top journals Management free medical journals Management famous journals Management Google Scholar indexed journals open reduction internal fixation articles open reduction internal fixation Research articles open reduction internal fixation review articles open reduction internal fixation PubMed articles open reduction internal fixation PubMed Central articles open reduction internal fixation 2023 articles open reduction internal fixation 2024 articles open reduction internal fixation Scopus articles open reduction internal fixation impact factor journals open reduction internal fixation Scopus journals open reduction internal fixation PubMed journals open reduction internal fixation medical journals open reduction internal fixation free journals open reduction internal fixation best journals open reduction internal fixation top journals open reduction internal fixation free medical journals open reduction internal fixation famous journals open reduction internal fixation Google Scholar indexed journals heart rate articles heart rate Research articles heart rate review articles heart rate PubMed articles heart rate PubMed Central articles heart rate 2023 articles heart rate 2024 articles heart rate Scopus articles heart rate impact factor journals heart rate Scopus journals heart rate PubMed journals heart rate medical journals heart rate free journals heart rate best journals heart rate top journals heart rate free medical journals heart rate famous journals heart rate Google Scholar indexed journals Blood pressure articles Blood pressure Research articles Blood pressure review articles Blood pressure PubMed articles Blood pressure PubMed Central articles Blood pressure 2023 articles Blood pressure 2024 articles Blood pressure Scopus articles Blood pressure impact factor journals Blood pressure Scopus journals Blood pressure PubMed journals Blood pressure medical journals Blood pressure free journals Blood pressure best journals Blood pressure top journals Blood pressure free medical journals Blood pressure famous journals Blood pressure Google Scholar indexed journals respiratory rate articles respiratory rate Research articles respiratory rate review articles respiratory rate PubMed articles respiratory rate PubMed Central articles respiratory rate 2023 articles respiratory rate 2024 articles respiratory rate Scopus articles respiratory rate impact factor journals respiratory rate Scopus journals respiratory rate PubMed journals respiratory rate medical journals respiratory rate free journals respiratory rate best journals respiratory rate top journals respiratory rate free medical journals respiratory rate famous journals respiratory rate Google Scholar indexed journals Selective Serotonin Reuptake Inhibitors articles Selective Serotonin Reuptake Inhibitors Research articles Selective Serotonin Reuptake Inhibitors review articles Selective Serotonin Reuptake Inhibitors PubMed articles Selective Serotonin Reuptake Inhibitors PubMed Central articles Selective Serotonin Reuptake Inhibitors 2023 articles Selective Serotonin Reuptake Inhibitors 2024 articles Selective Serotonin Reuptake Inhibitors Scopus articles Selective Serotonin Reuptake Inhibitors impact factor journals Selective Serotonin Reuptake Inhibitors Scopus journals Selective Serotonin Reuptake Inhibitors PubMed journals Selective Serotonin Reuptake Inhibitors medical journals Selective Serotonin Reuptake Inhibitors free journals Selective Serotonin Reuptake Inhibitors best journals Selective Serotonin Reuptake Inhibitors top journals Selective Serotonin Reuptake Inhibitors free medical journals Selective Serotonin Reuptake Inhibitors famous journals Selective Serotonin Reuptake Inhibitors Google Scholar indexed journals
Article Details
1. Introduction
Post-Traumatic Stress Disorder (PTSD) is an anxiety disorder that can occur after experiencing or witnessing a traumatic event which involves threatened death or serious injury [1,2]. The presence of PTSD in a surgical patient before, during and after perioperative period is associated with co-morbidities including cardiovascular dysfunction, chronic pain, depression and cognitive dysfunction, all of which can influence the risk of peri and postoperative morbidity and mortality [3]. So management of comorbidities associated with PTSD and prevention of evoking post-traumatic symptoms in the intraoperative period by interacting with patients and ameliorating anxiety is important for anaesthetist.
2. Materials and Methods
A 17 years male patient presented with fracture left shaft of femur following road-side accident a day back with history of loss of consciousness for 10 minutes. There was no associated history of ear, nose, throat bleed, eye injury, vomiting and seizures. The patient had a minor uneventful surgery of a right leg swelling under local anaesthesia 8 years back. There is no history of any major medical illness like asthma, hypertension, diabetes, tuberculosis, any active cold and cough, fever, drug allergy and previous blood transfusion. On clinical examination, patient was alert, conscious, co-operative and oriented to time, place and person with heart rate (HR): 76/min , blood pressure (BP): 110/78 mm of Hg, on auscultation chest was bilaterally clear, with air entry equal and with normal heart sounds with no murmurs, Mallampatti grade was II, with teeth, neck, spine showing no abnormalities. Investigations revealed hemoglobin 13.5 gm%, bleeding time 2 min 30 sec, clotting time 4 min 20 sec, urine complete examination, x-ray cervical spine USG whole abdomen and NCCT Head showed no significant abnormality. X-Ray left lower limb revealed fracture left shaft of femur. Therefore, open reduction internal fixation (ORIF) with nailing under sub-arachnoid block was planned.
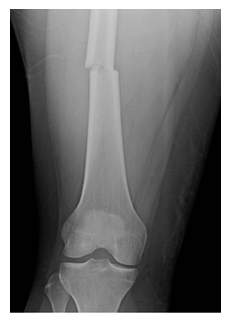
Figure 1: X- Ray left lower limb
2.1 Anaesthetic management
Patient was planned for ORIF with nailing under sub-arachnoid block for fracture left shaft of femur. 2.6 ml of 0.5% heavy Bupivacaine was injected in the sub-arachnoid space. Desired and adequate level of anaesthesia was achieved. Intra-operative vitals were monitored and maintained. Surgery lasted for 2 hours. Towards the end of the surgery, patient became anxious, agitated and started shaking, had tachypnea of 33 breaths/min and tachycardia with HR of 130 beats/min. He suddenly started responding less to commands and had difficult to arouse on commands. He was given 100% O2 through Bain’s circuit. Vitals were monitored. However, patient continued to be agitated and tachypnea persisted with respiratory rate (RR) 40 breaths/min. An ABG was sent which revealed pH=7.513, pCO2= 22.4 mm of Hg, pO2= 118.9 mm of Hg, HCO3=26.8 mmol/l, SpO2=99%, BE= 2.1mmol/l. Auscultation of chest revealed normal vesicular breath sounds with bilateral chest clear and normal heart sounds. Patient was irritable so was given injection midazolam 1mg i.v. His father was called in operating room to calm him and to make him feel safe. After some time his RR settled down to 20 breaths/min. He was conscious, responding to all the commands and maintaining his vitals. However, tachycardia persisted with HR 106 beats/min. He was observed in the HDU. Repeat ABG showed pH=7.4, pCO2=39, pO2=90, HCO3= 24 mmol/l, SpO2= 98%, BE= 0.4 mmol/l. Blood sugar, urea, creatinine were sent. Urine for fat globules, d-dimer, fibrinogen degradation products were sent to rule out fat embolism. All blood reports came normal. ECG, chest x-ray and fundus examination were all normal. After ruling out all medical causes, psychiatric consultation was sorted. The provisional diagnosis of PTSD was made by the psychiatrist. Injection lorazepam 1mg i.v. was given 2 hours post-operatively as advised by psychiatrist, after which patient was comfortable. Vitals were normal and then he was shifted to the general ward by afternoon. Oral benzodiazepines were prescribed by consulting psychiatrist as a part of the regular post-operative treatment regimen and were continued for 4 weeks. On regular follow ups in out-patient department, the patient complained of intermittent difficulty in sleeping and concentrating at work, having flash backs of the operating room scenes, not being interested in any daily chore, getting irritable and avoiding recall of the road traffic accident he underwent. The diagnosis of post-traumatic stress disorder was confirmed by the psychiatrists and appropriate treatment with regular follow up was continued for the patient.
3. Discussion
Post-Traumatic Stress Disorder (PTSD) is a psychiatric disorder whose diagnostic criteria include exposure of the patient to a traumatic event that evoked feelings of horror, fear and intense hopelessness (b) presence of at least one symptom of re-experiencing (c) avoidance or emotional numbing (d) persistant arousal (e) symptoms persisted for at least one month (f) these symtoms significantly impacted functioning or resulted in significant distress to the patient [4]. The presence of PTSD in a surgical patient can be of importance because it is associated with use of psychoactive medications and presence of psychological symptoms e.g. depression, chronic pain, cognitive dysfunction and occasionally cardiovascular co-morbidities which may increase the risk of peri-operative morbidity [3]. In preoperative assessment anaesthetist should focus on presence of cardiovascular disease, history of substance abuse, depression, use of psychoactive medications, presence of chronic pain [3]. To avoid withdrawal, psychoactive medications should generally be continued throughout the perioperative period [5]. Multimodal analgesia should be used in surgery. Patients with PTSD are anxious around unfamiliar people and unfamiliar environments [6]. So for evoking symptoms of PTSD the operating room team should interact with the patient to establish trust, ameliorate anxiety and should assure the patient that the environment is very safe. Staff should minimize loud noises and movements to avoid gaining the attention of patient. Also, whole team should emphasize that its goal is to make the patient comfortable during surgery. Triggers which precipitate acute anxiety should be avoided [7]. Evidence suggests that the perioperative process can transiently exacerbate PTSD symptoms [3]. There is a case report in which a young woman developed PTSD after sexual assault. She became acutely agitated and was physically violent towards operation room staff. Later she reported reexperiencing her prior abuse during that episode [7]. So surgery and anaesthesia can exacerbate posttraumatic symptom severity. PTSD patients stay undiagnosed and so do not receive psychological help [8]. In our patient, after ruling out the possible cardiovascular, respiratory system and psychological causes for the symptoms, patient was referred to the psychiatrist who made the diagnosis of PTSD and prescribed benzodiazepines (BDZ). Patient favourably responded to BDZ which relieves the symptoms of irritability, insomnia, anxiety and panic. Other treatment modalities include Selective Serotonin Reuptake Inhibitors (SSRI), Monoamine Oxidase Inhibitors (MAOI), Tri-cyclic Anti-depressants (TCAD), atypical anti-psychotics and anti-convulsants [8]. Nonpharmacological treatment of PTSD includes various forms of cognitive behavior therapy, reprocessing and desensitization of eye movements [9]. In spite the high frequency and potential severity of the psychological consequences of road traffic accidents, psychological services for patients are not provided in a routine comprehensive way. Often severity of psychological distress is undermined in these patients [10]. In our patient extensive pre-operative psychological interview would have benefitted. If diagnosed in early preoperative period, factors provoking PTSD would have been avoided in intraoperative period.
4. Conclusion
The diagnosis and anaesthetic management of a patient with PTSD can be challenging. The operative team comprising the anaesthesiologists and operating surgeons should establish trust while interacting with patient. Team should introduce themselves and should explain their respective roles in the surgery, calmly. They should reassure the patient that environment is safe there. Staff should minimise un-expected loud noise and extra movements. Pain and anxiety should be ameliorated. In future more research should be there to find PTSD implications in postoperative morbidity and mortality and to find ways to diagnose and treat it perioperatively.
Conflict of interest
None
References
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. (4th edtn), American Psychiatric Association (1994), Washington, DC, USA
- Lange JT, Lange CL, Cabaltica RB. Primary care treatment of posttraumatic stress disorder. Am Fam Physician 62 (2000): 1035-1040.
- Wofford K, Hertzberg M, Vacchiano C. The perioperative implication of posttraumatic stress disorder. AANAJ 80 (2012): 463-470.
- American Psychiatric Association. Desk reference to the diagnostic criteria from DSM-IV-TR. American Psychiatric Association 12 (2000): 218-220.
- Warner CH, Bobo W, Warner C, et al. Antidepressant discontinuation syndrome. Am Fam Physician 74 (2006): 449-456.
- Foa EB, Keane TM, Friedman MJ. Guidelines for treatment of PTSD. J Trauma Stress 13 (2000): 539-588.
- Crosby SS, Mashour GA, Grodin MA, et al. Emergence flashback in a patient with posttraumatic stress disorder. Gen Hosp Psychiatry 29 (2007): 169-171.
- American Psychiatric Association. Practice guidelines for the treatment of patients with acute stress disorder and posttraumatic stressdisorder. Am J Psychiatry 16 (2004): 1-31.
- Bradley R, Greene J, Russ E, et al. A multidimensional meta-analysis of psychotherapy or PTSD. Am J Psychiatry 162 (2005): 214-227.
- Stallard P, Velleman R, Baldwin S. Prospective study of post-traumatic stress disorder in children involved in road traffic accident. Br Med J 317 (1998): 1619-1623.
