Post-Pembrolizumab Optic Neuritis in a 57-Year Old Female with non-small cell lung carcinoma
Article Information
Artur Manasyan BS, Nyree Khachikyan BS, Stephanie Gaytan BS and Nafiseh Hashemi MD*
Neuro-ophthalmology Clinic, Hashemi Eye Care, Encino, USA
*Corresponding author: Nafiseh Hashemi, Neuro-ophthalmology Clinic, Hashemi Eye Care, Encino, USA
Received: 18 April 2022; Accepted: 25 April 2022; Published: 06 May 2022
Citation: Artur Manasyan, Nyree Khachikyan, Stephanie Gaytan and Nafiseh Hashemi. Post-Pembrolizumab Optic Neuritis in a 57-Year Old Female with non-small cell lung carcinoma. Journal of Ophthalmology and Research 5 (2022): 74-80
Share at FacebookAbstract
Pembrolizumab, also known as Keytruda, is a novel immunotherapeutic used for the treatment of certain cancers like non-small cell lung adenocarcinoma, melanoma, among other types. It is a checkpoint inhibitor that targets the PD-1/PD-L1 interaction and suppresses immune resistance of cancerous cells. We present a case of 57-year-old female who was treated with pembrolizumab for non-small cell lung adenocarcinoma and subsequently developed bilateral optic neuritis. The patient developed worsening vision and a constricted field of vision as a result. Pembrolizumab therapy was stopped, followed by immediate administration of corticosteroid therapy. As a result, the patient’s vision experienced moderate improvement without full remission due to the consequential post-swelling optic atrophy. Although pembrolizumab is a very effective and FDA approved treatment, reports of such rare cases are important in helping guide treatment plans of future patients.
Keywords
Pembrolizumab, check point inhibitor, PD-1/PD-L1, optic neuritis, vision loss, non-small cell carcinoma
Article Details
1. Intruduction
Pembrolizumab is a humanized antibody that was initially utilized as immunotherapy for melanoma [1]. Although melanoma was the first type of cancer that Keytruda was approved for, it is also currently being used in cases of non-small cell lung carcinoma, head and neck squamous cell carcinoma. [2]. Similar to other biologics like nivolumab (Opdivo), ipilimumab (Yervoy), and atezolizumab (Tecentriq), Keytruda functions primarily as a checkpoint inhibitor [2]. It targets the PD-1/PD-L1 interaction that is responsible for immune resistance. Tumor cells express the PD-L1 ligand that has binding activity with the known PD-1 protein found on T cells [3]. PD-1 functions as a checkpoint inhibitor that inhibits immune activity to prevent potential autoimmune-induced damage [4]. Tumor cells expressing PD-L1 have obtained ability in mitigating T cell-induced immune targeting of such cancerous cells through the PD-1/PD-L1 interaction and subsequent immune down regulation.
2. Related Reported Cases
Immunotherapy-induced optic neuritis has been reported in multiple isolated case reports. One of the patients, a 76-year-old man, was on pembrolizumab for non-small cell lung carcinoma. The patient presented with left-sided vision loss and subsequent ophthalmic evaluation demonstrated left optic nerve swelling. His vision decreased to 20/200 in the affected eye. Pembrolizumab therapy was stopped and corticosteroids were given over a nine-week period, resulting in the optic neuritis resolving and his vision being restored to normal [5]. Similarly, a 63-year-old man was diagnosed with pembrolizumab-induced unilateral retrobulbar optic neuritis, which was also suppressed by prednisolone, and later, dexamethasone. While his visual field disorder was not returned back to normal, his condition was kept from exacerbating and his overall vision improved [6].
Recovery from vision loss is seen often with discontinuing of medication and administering steroids regardless of mechanism of vision loss. A 58-year-old man recovered fully after stopping pembrolizumab and taking steroids for two months from vision loss caused by drug-induced choroidal effusion and retinal detachment. Another 57-year-old man also recovered fully after having bilateral uveitis and right optic disc edema from pembrolizumab, by stopping the medication and getting on steroids [7].
In some cases, corticosteroids do not improve the condition of optic neuritis and only stop the progression. In one case, a woman in her 70’s taking pembrolizumab for metastatic melanoma, with history of thyroid cancer and hypothyroidism follow-ing thyroid removal, presented with rapid deterioration of vision and pain in both eyes follow-ing treatment. The corticosteroids administered did not improve her vision. Her light perception vision in one eye minimally improved following plasm-apheresis [8].
Another 61-year-old female developed optic neuritis bilaterally after ipilimumab/nivolumab admin-istration, with normal vision of 20/20 in the right eye and decreased vision of 20/100 in the left eye. Immunotherapy was discontinued and corticosteroids were administered [9]. Atezolizumab, another checkpoint inhibitor, has also been associated with ophthalmic adverse reactions in an isolated case study. A 64 year-old developed unilateral optic neuritis in the left eye 12 months after starting immunotherapy. The patient had a sudden onset of decreased vision in the left eye and was demonstrated to have enlarged blind spot and nasal visual field defects. As with other cases, immunotherapy was ceased and steroid therapy was administered, resulting in recovery of optic nerve swelling and recovery of visual field defects [10].
A third checkpoint inhibitor, dabrafenib, has been reported to cause bilateral uveitis in a patient that was using the treatment for metastatic melanoma. With steroids and cessation of dabrafenib treatment, the patient’s symptoms resolved. A few months later, the patient was started on pembrolizumab treatment which again caused her recurrent bilateral uveitis, treated with steroids [11]. In a case report involving 31 patients from 14 different institutions on various PD-1, PD-L1, and CTLA-4 inhibitors resulted in the patients developing neuro-ophthalmic complications, such as inflammatory orbital/extraocular muscle involvement, involvement of the optic nerve, cranial nerve palsy, and neuromuscular junction dysfunction causing ocular problems. Corticosteroids, as with prior reported cases, improved most of the patients who suffered from optic neuropathy, but other conditions yielded more variable results [12].
Along with optic neuritis, neuroretinitis, giant cell arteritis, myasthenia gravis, among other ophthalmic conditions, have also been reported [13]. The entire class of immune checkpoint inhibitors is associated with ophthalmic inflammatory adverse reactions in approximately 1% of the receiving patient population [14].
3. Case Summary
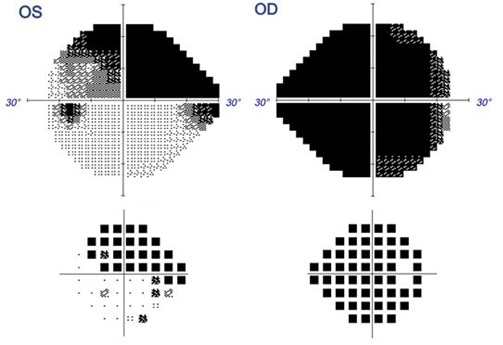
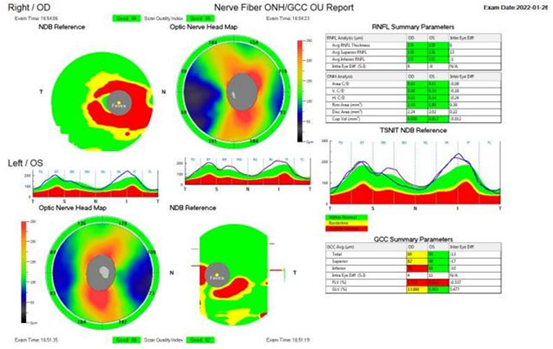
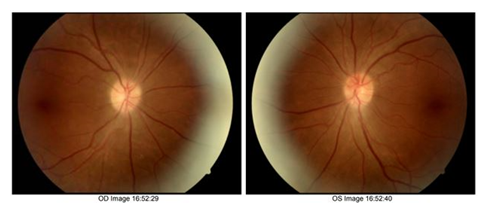
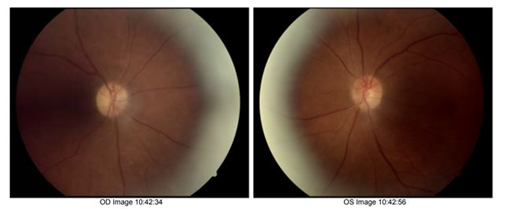
The patient is a 58-year old female who was referred for a neuro-ophthalmology consultation as a result of visual symptoms mainly involving vision loss in the right eye. She had a history of non-small cell lung cell carcinoma and has been receiving pembrolizumab (Keytruda) infusions every two weeks for a period of two months. Prior MRI was reported to be unremarkable. Central visual acuity was limited to hand motion (HM) in the right eye and 20/40 in the left eye. Color vision was also limited in the right eye (0/11) and full in the left eye (11/11). Visual field testing revealed a constricted visual field defect OD and superior altitudinal defect OS [Figure 1]. Optical coherence tomography (OCT) of the macula was done to confirm that there was no macular edema. OCT for the assessment of the optic nerve showed retinal nerve fiber layer (RNFL) thickness 135 microns in the right eye and 129 microns in the left eye, indicating optic nerve swelling or optic neuritis, with more significant swelling in the right optic nerve [Figure 2]. Fundus photo also showed RNFL thickening (superior and inferior arcade) [Figure 3].
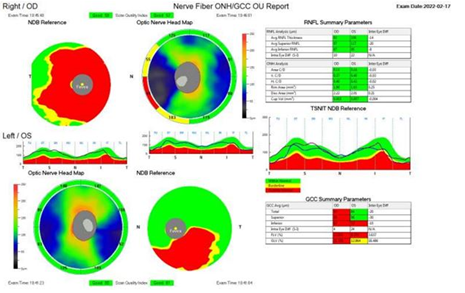
There was also significant ganglion cell layer loss in both eyes, with greater severity in the right relative to the left. Subsequent bloodwork for autoimmune markers was ordered but revealed no remarkable findings. After discussing the visual loss with the oncologist, Pembrolizumab treatment was disco-ntinued. The patient received corticosteroid infusions a week after symptom onset, followed by 60 mg of oral prednisone, tapering down to 20 mg. In a three-week follow up, the patient presented with somewhat improved vision to counting fingers at 1 foot distance (CF 1ft) in the right eye and 20/25 in the left eye. OCT revealed RNFL thickness of 92 microns and 106 microns in the right and left eye, respectively, indicating reduced optic nerve swelling [Figure 4]. On dilated slit lamp examination, there was diffuse optic atrophy of the right optic nerve and temporal pallor of the left optic nerve [Figure 5].
4. Conclusion
Pembrolizumab (Keytruda) is a novel biologic currently used for the treatment of non-small lung cell carcinoma. Such immunotherapy has shown to be effective in improving clinical outcomes in cancer patients. Nevertheless, it is vital to understand the potential side effects to provide the most appropriate individualized clinical approach. Cease of immunotherapy treatment, ophthalmic evaluation, and use of steroid therapy is currently the recommended plan for associated optic neuritis. There have been a few cases of optic neuritis reported in association with other potential side effects like ocular pain, itchiness, and uveitis. While in the other case reports of optic neuritis associated with pembrolizumab, the vision restored after discontinuing of medication and steroid therapy, in our case the vision has not improved significantly. We suggest that the medication should stop as soon as the patient notices any visual changes and steroid treatment to be start promptly. Routine frequent screening eye exam may help to prevent vision loss as complication of cancer therapy with immune check inhibitors.
References
- Raedler LA. Keytruda (Pembrolizumab): First PD-1 Inhibitor Approved for Previously Treated Unresectable or Metastatic Melanoma. Am Health Drug Benefits 8 (2015): 96-100.
- Alsaab HO, Sau S, Alzhrani R, Tatiparti K, et al. PD-1 and PD-L1 Checkpoint Signaling Inhibition for Cancer Immunotherapy: Mechanism, Combinations, and Clinical Outcome. Front Pharmacol 8 (2017):
- Borst J, Busselaar J, Bosma DMT, Ossendorp F. Mechanism of action of PD-1 receptor/ligand targeted cancer immunotherapy. Eur J Immunol 51 (2021): 1911-1920.
- Jubel JM, Barbati ZR, Burger C, Wirtz DC, Schildberg FA. The Role of PD-1 in Acute and Chronic Infec Front Immunol 11 (2020): 487.
- Makri OE, Dimitrakopoulos FI, Tsapardoni F, Tsekouras I, et al. Isolated optic neuritis after pembrolizumab administration for non-small-cell lung carcinoma. Int J Neurosci 14 (2020): 1-6.
- Kawakado K, Tamura T, Nakanishi M, Makimoto G, Kuyama S. Retrobulbar Optic Neuritis Induced by Pembrolizumab in a Patient with Lung Adenocarcinoma. Internal Medicine 60 (2021): 3941-3945.
- Telfah M, Whittaker TJ, Doolittle GC. Vision loss with pembrolizumab treatment: A report of two cases. Journal of Oncology Pharmacy Practice 25 (2019): 1540-1546.
- Nassar A, Rivera N, Mora J, Martinez A. A bilateral optic neuritis side effect of biological treatment with pembrolizumab in a patient with metastatic melanoma. Journal of Neurology and Stroke 10 (2020): 177-181.
- Kim JM, Materin MA, Sznol M, Kluger HM, Weiss S, Chow J, et al. Ophthalmic Immune-Related Adverse Events of Immunotherapy: A Single-Site Case Series. Ophthalmology 126 (2019): 1058-1062.
- Mori S, Kurimoto T, Ueda K, Enomoto H, Sakamoto M, at al. Optic Neuritis Possibly Induced by Anti-PD-L1 Antibody Treatment in a Patient with Non-Small Cell Lung Case Rep Ophthalmol 20 (2018): 348-356.
- Taylor SC, Hrisomalos F, Linette GP, Rao KP. A case of recurrent bilateral uveitis independently associated with dabrafenib and pembrolizumab therapy. American Journal of Ophthalmology 2 (2016): 23-25.
- Sun MM, Seleme N, Chen JJ, Zekeridou A, Sechi E, Walsh RD, Beebe JD, et al. Neuro-Ophthalmic Complications in Patients Treated with CTLA-4 and PD-1/PD-L1 Checkpoint Blockade. Journal of Neuro-Ophthalmology 41 (2021): 519-530.
- Yu CW, Yau M, Mezey N, Joarder I, Micieli JA. Neuro-ophthalmic Complications of Immune Checkpoint Inhibitors: A Systematic Review. Eye Brain 12 (2020): 139-167.
- Francis JH, Jaben K, Santomasso BD, Canestraro J, Abramson DH,. Immune Checkpoint Inhibitor-Associated Optic Neuritis. Ophthalmology 127 (2020): 1585-1589.