Oxygen Saturation Depletion Measured in Children Wearing Masks at School in France During the Covid-19 Pandemic Years 2020-2022
Article Information
Collectif Citoyens Oxytest1, Valère Lounnas2, Alexis Lacout3, Xavier Azalbert4, Christian Perronne5
1Pa Olivier DAHENNE, 8 route de Findrol, 74250 Marcellaz, France
2EMBL Heidelberg alumni, Meyerhofstraße 1, 69117 Heidelberg, Germany
3Centre de diagnostic ELSAN, 15000 Aurillac, France
4Ecole d'Economie de Toulouse - TSE, 1988 Econometrics, France
5Infectious and Tropical Diseases, Paris, France
*Corresponding author: Valère Lounnas, EMBL Heidelberg alumni, Meyerhofstraße 1, 69117 Heidelberg, Germany.
Received: 03 June 2023; Accepted: 13 June 2023; Published: 19 June 2023
Citation: Collectif Citoyens Oxytest, Valère Lounnas, Alexis Lacout, Xavier Azalbert, Christian Perronne. Oxygen Saturation Depletion Measured in Children Wearing Masks at School in France During the Covid-19 Pandemic Years 2020-2022. Archives of Microbiology and Immunology. 7 (2023): 76-82
Share at FacebookAbstract
Pulse oximeters were used to assess peripheral blood saturation in children at elementary school exit. 249 children were tested in 9 different collective citizenship actions organized in five cities. Oximetric measurements were performed with the children parents agreement under the supervision of a general practitioner or professional nurse in the presence of an usher or a sworn civil public officer. A questionnaire on the side effects and symptoms of wearing a mask at school for prolonged hours was offered to the children and their parents. 84.7% of the children declared having experienced one side effect such as headache, difficulty concentrating, abnormal fatigue, drowsiness, irritability, itching, skin eruption, anxiety... Difficulty breathing during the day (suffocation in one case) was reported by 56.4% (119/211) of the children who answered the questionnaire and 14.5% had a pathological oxygen saturation value SpO2 ≤ 95%. This study describes the profound physiological and psychological discomfort children have experienced wearing masks at school from end Oct. 2020 to Apr. 2022.
Keywords
Covid-19, mask, elementary school, children, pulse oximetry, hypoxemia, SpO2, oxygen saturation, wearing masks, side effects, psycho-social impact
Article Details
1. Introduction
On October 29th, 2020, the prime minister of France announced that wearing a mask was mandatory at elementary school for children of age 6-11 years. This obligation along with a whole series of drastic restrictions on individual freedom (lock-downs, vaccine and Covid-19 passport to access hospitals, shopping centers and having the right to travel) lasted one and a half year till April 2022. This public health measure was taken on the speculative assertion that masks would prevent the spread of the pandemic throughout families, and thus would spare the lives of many frail and older people as well as adults at risk. This decision seems to have been made on an ill-defined ground without any study or consideration for the potential immediate side effects and long-term impact on the physiological and psychological well-being of young children. It became all the more questionable when the French minister of health surprisingly declared in April 2021 that, in fact, children were contaminated only a little and subject to contaminating each others only a little as well. As of today, there is still no evidence published on the public health benefit of young children wearing a mask at school. In contrast, several studies in France and in Europe have brought to the fore a number of symptoms of immediate discomfort and potential long-term impact on cognitive and social abilities children have experienced after wearing masks at school all day long for prolonged periods of time [1-4].
As soon as December 2020, a manifesto issued by a group of professional nurses specialized in pediatrics had warned about a number of issues related to children wearing masks at school [5]. Although this manifesto was thoroughly documented and communicated to the French government, no nationwide study was initiated. One year later, another assessment with further analysis of the impact of the Covid-19 sanitary measures on children health was conducted by the Enfance et Libertés public association, reflecting the legitimate concern growing in the public about the children health. It was published in February 2021 but still was left without any response from the government [6]. This is why we have undertaken to further investigate the physiological effects and the here-above mentioned risks of wearing a mask at school, directly, by oximetric measurement on the children and using a questionnaire, both performed on a voluntary basis by their parents. The objective of the Collectif Citoyens Oxytest, our group of citizens, was to supervise and provide support to a nationwide inquiry with the help of general practitioners (GPs) and professional nurses, under the control of ushers and duly sworn persons to insure irreproachable ethics.
2. Methods
A protocol was setup to measure the peripheral blood oxygen level in children with a pulse oximeter at the moment they leave school. A pulse oximeter is a non-invasive device that measures blood oxygen saturation (SpO2) via a beam of light that crosses the skin of the tip of a finger [7].
The participation in the study was made on a voluntary basis by parents who agreed on the protocol beforehand via an associative network of citizens sharing the same concern about the health of their children. Measurements were performed by the child's parents (or legal representative) assisted by a GP or a nurse under the control of a sworn civil public officer. They all signed the individual oximetric data collection form (Appendix A1).
A kit, together with a tutorial on YouTube, was provided on internet with the aim to make the oximetric measurement easy to access, effective and reproducible [8,9]. The whole measurement protocol was performed as follows under the supervision of a GP or a professional nurse assisting the child's parent:
- The health professional made sure the hands of the child were correctly warmed.
- The oximeter was appropriately disinfected before every measurement.
- The oximeter was placed on the child's index finger. It was started. Two digital measurements were rapidly indicated: the pulse and the oxygen saturation, usually between 99% and 95%. The healthcare professional waited measurements are stabilized before recording them.
- The two values were recorded with the other information on the individual data collection form.
- Particular attention was paid to oxygen saturation values below or equal to 95%:
- if the saturation value is between 96% and 99% it was simply recorded and the test stops, if the saturation value was below or equal to 95% it should then be carefully noted and it was advised to attach a photography of the oximeter to the data collection form.
- After the test, the child removed its mask and was offered to breath without wearing a mask for 10-15 minutes, for instance by running and playing normally.
- A second test was performed thereafter and results were noted.
- All other information were noted. It was possible to bring a weighing scale if one wished to record the child's weight more accurately than the parents declaration.
- The parents (or the legal representative), the general practitioner and the sworn civil public officer signed the individual data collection form.
A questionnaire (Appendix 1) was offered to the children and their parents to record side effects and symptoms experienced by the children including: headaches, abnormal fatigue, drowsiness, irritability, discomfort, nosebleeds, itching, problem wearing glasses and difficulty breathing, with an open question on the other possible symptoms the children may have experienced.
3. Results
3.1 Locations of data collection actions
Nine oximetric data collection actions were performed in France during the school year 2020-2021: one in Fillinges (Department of Haute-Savoie) on 26 March 2021 with the presence of 3 GPs, 3 nurses and 1 sworn public officer; two in Gennevilliers (Department of Val d’Oise, Greater Paris region) on 20 May and 22 June 2021 with the presence of 2 GPs, 1 nurse and sworn locally elected authorities; four in Montfermeil (Department of Seine-Saint-Denis, Greater Paris region) in June 2021, 3 of which having taken place in recreational centers after school, one in Narbonne (Department of Aude) on 3 June 2021 with the presence of 1 GP, 1 nurse and 1 sworn public officer. The last one has taken place at school exit in Cuxac-d'Aude (Department of Aude) on 4 June 2021 with the presence of 1 GP, 1 nurse and 1 sworn public officer.
3.2 Tested children population
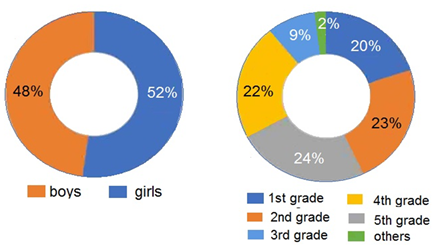
249 pupils from 1st grade to 5th grade (mean age 7.1 years) were tested (Figure 1). The mean duration of wearing a mask was 7.37 h/day, 14% of the masks worn were cloth masks and 86% surgical masks.
3.3 Measurement synthesis
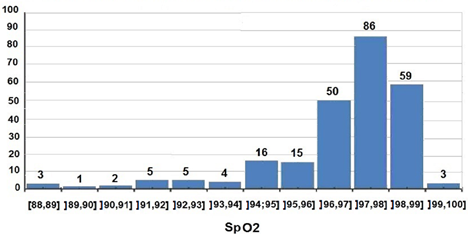
Figure 2 gives the distribution of peripheral blood oxygen saturation (SpO2) measured at school exit in outdoor environment with children keeping wearing their masks: 51 children had a SpO2 value ≤ 96% and 36 a SpO2 value ≤ 95%.
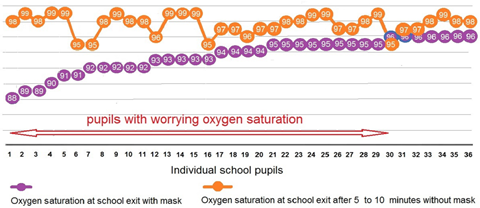
A second measurement could be performed after a recovery time of 5 to 10 minutes without mask in only 36 children, among the 51 ones with a SpO2 value ≤ 96%. All but 4 children have recovered a SpO2 value ≥ 96% (Figure 3). We note that in the group of children with worrying hypoxemia, there was the same proportion of cloth masks (13.9%) as in the overall children population tested.
Figure 3 compares SpO2 saturation values at school exit with those obtained after a recovery time of at least 5 minutes without mask for 36 children with an initial saturation ≤ 96%.
3.4 Questionnaire results
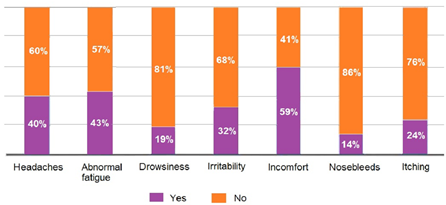
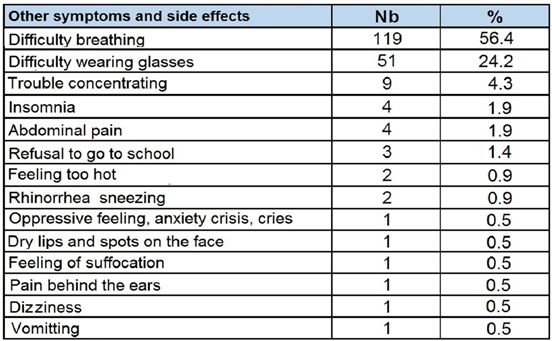
The questionnaire results were collected in Figure 4 and Table 1. The children from Narbonne and Cuxac-d'Aude (n=38) were not questioned about possible side effects and thus the percentages of Table 1 were calculated for only 211 children. In total, 84.7% of children (211/249) (100% of the children questioned) have answered having experienced one symptom listed in Figure 4 and 80.3% (200/249) (94,7% of those who answered the questionnaire) declared having experienced at least one other symptom listed in Table 1. 57% (142/249) have experienced 3 symptoms or more. Difficulty breathing during the day were reported by 56.4% (119/211) of the children questioned on side effects, and suffocation was reported in one case. Problem wearing glasses was reported in 24.2% (51/211). Some had stopped wearing glasses in class.
4. Discussion
The present study was initiated after some parents had decided on their own to measure the oxygen saturation in their children weakened after a day at school with a mask. Discovering with astonishment low SpO2 values in their children, they became whistle blowers. Of note, 50 associations or children parents have attempted to conduct similar actions in other French cities, but they were confronted with refusal from the French national education (Ministère de l’Education Nationale) and sometimes their action was forbidden by the city authorities or by pressure from the departmental prefect.
As of April 2023, it is indisputably admitted that wearing a mask for long hours during the day has immediate detrimental adverse effects on health, including: itching, headache, and restriction of oxygen in two thirds of the people [4]. "Extended mask-wearing by the general population could lead to relevant effects and consequences in many medical fields and cause contamination in public spaces due to improper mask disposal" [3]. Here, the results show very clearly the negative impact of wearing a mask on peripheral blood oxygen saturation in school children. The proportion of children, between 6 and 11 years old, reporting immediate side effects and symptoms was very high (84.7%). Main symptoms were: headaches, difficulty breathing (including one case of suffocation), trouble concentrating, drowsiness, insomnia. Not less than 36 children (14.5 %) had a pathological SpO2 value ≤ 95%. The detrimental effect on health was not dependent on the type of mask, cloth mask or surgical mask.
Despite the fact that oxygen saturation returned to at least 96% in most children after 5 to 10 minutes of free breathing, it is legitimate, medically speaking, to raise concerns that hypoxemia, repeated every day for a year and a half, may have had a long term detrimental effect on the children normal cognitive and social development [5,6,10], with possible effect on the development of their brain capacity. In the latter respect there is a total absence of clinical and epidemiological data since this is the first time since the Spanish flu of 1918-1919 that such a social hysteria and mass-coercion existed [11]. A study on mice subjected to chronic mild hypoxia (i.e. constant oxygen deprivation) over a period of two weeks showed cerebrovascular remodeling [12]. Here, the children were subjected to wearing a mask as long as one third of the day, and certainly the damages on their learning process and psychology should be our prime concern. Nonetheless, scientific studies should be undertaken on the physiological effects of wearing a mask, not only measuring oxygen saturation but also the possible development of germs along with other physiological parameters.
Masks and induced hypoxemia may have medical implications. It is conceivable that masked adults, especially the elderly, may have also suffered from potential mask-induced chronic hypoxemia, as did children. Hypoxemia has been shown to be a risk factor for progression to the dangerous inflammatory phase of COVID 19; conversely, oxygen therapy would be protective [13,14]. In the elderly hypoxemia could significantly promote the onset of inflammation and increase the morbidity and mortality of the disease. In children, the consequences are quite certainly negligible in this respect, as almost all have benign forms.
In fact, the general social issue of constantly wearing masks with its implications on how western societies can treat their children is so sensitive that a complete article can be found in the Science section of the broad-public audience National Geographic magazine that claims that wearing mask at school on a permanent basis is of absolutely no harm for the children, regardless of the aspect considered : medical, cognitive, social and psychological [15]. Of course, this cannot be true as human beings are by nature not meant to breath through a mask.
In the French manifesto for the children of Dec. 2020, the negative effects observed by professionals in pediatric are very clearly defined. Children have had difficulty to understand and listen to other persons, in particular when listening to the referent adults. They develop also difficulties in learning, especially learning phonemes in the first and second grades, and their capacity to recognize and acquire emotions is hampered. In addition, perturbations have been observed on the psychological and social relationship levels with children perceiving their environment as anxiety-provoking, implying perturbations in their relationships to other persons due to physical distancing and the loss of the sense of touch along with the idea that other persons are dangerous. The worse psychological torment inflicted was undoubtedly the feeling that they may cause the death of a relative. All these psychological torments may have an impact on the personality development [5,16-19].
We have noted that children were particularly happy and comforted that adults get interest in them and have all answered the questionnaire with interest. Surprisingly, we have noted that most of the parents did not discuss with their children the problems they encountered with wearing a mask at school and that they discovered the discomfort of their children on that occasion. They were surprised and sometimes very concerned as well about the answers of their children to the questionnaire. We cannot help thinking.
5. Conclusion
The side effects of hypoxemia in children wearing mask at school have been dramatically underestimated and unduly disregarded by the French health authorities and government during the Covid-19 crisis.
Acknowledgments
There are many thanks for this study because of the involvement and participation of many collective groups of citizens and collaborative associations. We thank all the people who had the idea of these collective citizenship actions, who have brought their support and have promoted them. We thank the people who have helped set up the communication tools and the making of the actions report.
We thank the parents and grandparents, associations of parents who have put their energy with great personal involvement to setup an oximetry action in their city. We also thank the few city majors, city councilors and parliament members that have accepted and given their support to these collective citizenship actions. Thanks as well to the ushers who have helped us and have allowed us to present here indisputable results that could be used legally.
We will not forget either the GPs and benevolent professional nurses who have helped organize and participated in these actions with great courage and professionalism. Finally, and the thanks that are closer to our heart go to the children and their parents that have accepted to participate in these oximetry tests with great honesty, sharing their anxiety with us and encouraging us to pursue this action to the end.
Funding
This work was entirely benevolent. The authors declare that this study received funding from Association Bon Sens to cover the publication fees. The persons voting to provide funds were not involved in the study design, collection, analysis, interpretation of data, the writing of this article or the decision to submit it for publication.
References
- Fontanet A, Grant R, Tondeur L. et al. SARS-CoV-2 infection in primary schools in northern France: A retrospective cohort study in an area of high transmission 15 (2021).
- Piquard-Kippfer A, Cavadini T, Sprenger-Charolles L, Gentaz E. Impact of lip-reading on speech perception in French-speaking children at risk for reading failure assessed from age 5 to 7. Annee Psychologique 121 (2021): 3-18.
- Kai Kisielinski, Paul Giboni, Andreas Prescher, et al. Is a Mask That Covers the Mouth and Nose Free from Undesirable Side Effects in Everyday Use and Free of Potential Hazards?18 (2021): 4344.
- Naveen Athrappully. Masks Cause Headaches, Itching, and Lower Oxygen Intake: Study The Epoch Times April 9 (2023).
- Cabot L, Desmoyers C, Dodelin Bricout C, et al. Manifeste pour les enfants 15 (2020).
- Masque Enfants https://enfance-libertes.fr/masques/
- Jubran A. Pulse oximetry.Tobin MJ (ed). Principles and Practice of Intensive Care Monitoring. New York: McGraw Hill, Inc(1998): 261–287.
- Opération oxymétrie https://enfance-libertes.fr/oxymetrie/
- Pourquoi et comment organiser une “opération oxymétre” à l'école. https://www.youtube.com/watch?v=-Te1le40wZY
- Cooper M. Enquête empirique et théorique sur les effets psychologiques du port du masque Thesis (1999).
- Christine Hauser The Mask Slackers of 1918, The New York times PublishedAug. 3, 2020, UpdatedDec 10 (2020).
- Sebok K. Halder Richard Milne the impact of chronic mild hypoxia on cerebrovascular remodelling; uncoupling of angiogenesis and vascular breakdown.
- Chauhan A, Kaur R, Chakrbarti P, Pal A. "Silent Hypoxemia" Leads to Vicious Cycle of Infection, Coagulopathy and Cytokine Storm in COVID-19: Can Prophylactic Oxygen Therapy Prevent It? Indian J Clin Biochem 36 (2021): 468-472. Epub 2021 Mar 15. Erratum in: Indian J Clin Biochem 29 (2021): 1.
- Michard F, Shelley K, L'Her E. COVID-19: Pulse oximeters in the spotlight. J Clin Monit Comput 35 (2021): 11-14. Epub 2020 Jun 23. Erratum in: J Clin Monit Comput 21 (2020).
- Amy McKeever Do masks really harm kids? Here's what science says. National Geographic Science Coronavirus coverage. Published February 17 (2022).
- Aude Henry Dépression, tentative de suicide chez les ados: l'alarmante bombe à retardement de la crise Covid.
- Jeffrey A. Bridge, PhD, Donna A. Ruch, PhD, Arielle H. Sheftall, PhD et al. Youth Suicide During the First Year of the COVID-19 Pandemic PEDIATRICS 151 (2023): e2022058375.
- Michela Bersia, Emanuele Koumantakis, Paola Berchialla et. al. Suicide spectrum among young people during the COVID-19 pandemic: A systematic review and meta-analysis eClinicalMedicine 54 (2022): 101705.
- Ryunosuke Goto, Yusuke Okubo and Norbert Skokauskas reasons and trends in youth’s suicide rates during the COVID-19 pandemic The Lancet Regional Health - Western Pacific 27 (2022): 100567.
Appendix