Nutritional Assessment of Children Aged 6 to 59 Months Admitted in Two Hospitals in the City of Ziguinchor/Senegal
Article Information
Diouf François Niokhor¹*, Ba Abou², Ndongo Pascale Njock¹, Poussy Pape Formose¹, Sow Amadou³, Senghor Seynabou¹
¹Department of Pediatrics, Ziguinchor Regional Hospital, Senegal
²Department of Pediatrics, Dalal Jamm National Health Center, Dakar, Senegal
³Pediatrics Abass Ndao Hospital, Avenue Cheikh Anta Diop Dakar fann gueule tapée, Senegal
*Corresponding Author: Diouf François Niokhor, Department of Pediatrics, Ziguinchor Regional Hospital, Dakar, Senegal.
Received: 22 December 2023; Accepted: 12 January 2024; Published: 24 January 2024
Citation: Diouf François Niokhor, Ba Abou, Ndongo Pascale Njock, Poussy Pape Formose, Sow Amadou, Senghor Seynabou. Nutritional Assessment of Children Aged 6 to 59 Months Admitted in Two Hospitals in the City of Ziguinchor/Senegal. Journal of Pediatrics, Perinatology and Child Health. 8 (2024): 05-09.
Share at FacebookAbstract
Introduction: Malnutrition is a major public health concern of developing countries. Very few studies on malnutrition have been conducted in the Southern part of Senegal. The objective of the study was to assess the nutritional status of children aged 6- 59 months in two hospitals of the city of Ziguinchor.
Material and methods: This was a prospective, two-center study assessing the nutritional status of children aged 6 to 59 months for a period of 4 months from December 1, 2020 to March 1, 2021.
Results: 103 children were enrolled at Ziguinchor regional hospital and 34 children at Ziguinchor Peace hospital representing a cohort of 137 children. 21, 2% were wasted, 18, 2% had stunted growth and 17, 5% were underweight. Among those malnourished children, 98,1% of mothers were over 20 years of age, 52,7% had low education level; 38,9% of fathers were unemployed; 79,6% of parents had a poor socio economic status and 90,7% were married. The sex ratio was 1.2.70, 3% of malnourished children aged less than 24 months, 94, 4% were fully vaccinated. Upon admission, 50 % of malnourished children had acute gastroenteritis (33, 3%) and pneumonia (11, 1%). HIV (11, 1%) and congenital heart diseases (7,4%) were the main concomitant pathologies. No death cases were reported.
Conclusion: In the context of public health policies of developing countries, knowledge of best attitudes and practices towards child nutrition and improvement of population’s quality of life must be a priority.
Keywords
Malnutrition; Emaciation; Children; Ziguinchor
Pediatrics articles Pediatrics Research articles Pediatrics review articles Pediatrics PubMed articles Pediatrics PubMed Central articles Pediatrics 2023 articles Pediatrics 2024 articles Pediatrics Scopus articles Pediatrics impact factor journals Pediatrics Scopus journals Pediatrics PubMed journals Pediatrics medical journals Pediatrics free journals Pediatrics best journals Pediatrics top journals Pediatrics free medical journals Pediatrics famous journals Pediatrics Google Scholar indexed journals Malnutrition articles Malnutrition Research articles Malnutrition review articles Malnutrition PubMed articles Malnutrition PubMed Central articles Malnutrition 2023 articles Malnutrition 2024 articles Malnutrition Scopus articles Malnutrition impact factor journals Malnutrition Scopus journals Malnutrition PubMed journals Malnutrition medical journals Malnutrition free journals Malnutrition best journals Malnutrition top journals Malnutrition free medical journals Malnutrition famous journals Malnutrition Google Scholar indexed journals Nutrients articles Nutrients Research articles Nutrients review articles Nutrients PubMed articles Nutrients PubMed Central articles Nutrients 2023 articles Nutrients 2024 articles Nutrients Scopus articles Nutrients impact factor journals Nutrients Scopus journals Nutrients PubMed journals Nutrients medical journals Nutrients free journals Nutrients best journals Nutrients top journals Nutrients free medical journals Nutrients famous journals Nutrients Google Scholar indexed journals Anthropometric articles Anthropometric Research articles Anthropometric review articles Anthropometric PubMed articles Anthropometric PubMed Central articles Anthropometric 2023 articles Anthropometric 2024 articles Anthropometric Scopus articles Anthropometric impact factor journals Anthropometric Scopus journals Anthropometric PubMed journals Anthropometric medical journals Anthropometric free journals Anthropometric best journals Anthropometric top journals Anthropometric free medical journals Anthropometric famous journals Anthropometric Google Scholar indexed journals Children articles Children Research articles Children review articles Children PubMed articles Children PubMed Central articles Children 2023 articles Children 2024 articles Children Scopus articles Children impact factor journals Children Scopus journals Children PubMed journals Children medical journals Children free journals Children best journals Children top journals Children free medical journals Children famous journals Children Google Scholar indexed journals Vaccination articles Vaccination Research articles Vaccination review articles Vaccination PubMed articles Vaccination PubMed Central articles Vaccination 2023 articles Vaccination 2024 articles Vaccination Scopus articles Vaccination impact factor journals Vaccination Scopus journals Vaccination PubMed journals Vaccination medical journals Vaccination free journals Vaccination best journals Vaccination top journals Vaccination free medical journals Vaccination famous journals Vaccination Google Scholar indexed journals Gastroenteritis articles Gastroenteritis Research articles Gastroenteritis review articles Gastroenteritis PubMed articles Gastroenteritis PubMed Central articles Gastroenteritis 2023 articles Gastroenteritis 2024 articles Gastroenteritis Scopus articles Gastroenteritis impact factor journals Gastroenteritis Scopus journals Gastroenteritis PubMed journals Gastroenteritis medical journals Gastroenteritis free journals Gastroenteritis best journals Gastroenteritis top journals Gastroenteritis free medical journals Gastroenteritis famous journals Gastroenteritis Google Scholar indexed journals Pneumonia articles Pneumonia Research articles Pneumonia review articles Pneumonia PubMed articles Pneumonia PubMed Central articles Pneumonia 2023 articles Pneumonia 2024 articles Pneumonia Scopus articles Pneumonia impact factor journals Pneumonia Scopus journals Pneumonia PubMed journals Pneumonia medical journals Pneumonia free journals Pneumonia best journals Pneumonia top journals Pneumonia free medical journals Pneumonia famous journals Pneumonia Google Scholar indexed journals Infectious articles Infectious Research articles Infectious review articles Infectious PubMed articles Infectious PubMed Central articles Infectious 2023 articles Infectious 2024 articles Infectious Scopus articles Infectious impact factor journals Infectious Scopus journals Infectious PubMed journals Infectious medical journals Infectious free journals Infectious best journals Infectious top journals Infectious free medical journals Infectious famous journals Infectious Google Scholar indexed journals Malnourished children articles Malnourished children Research articles Malnourished children review articles Malnourished children PubMed articles Malnourished children PubMed Central articles Malnourished children 2023 articles Malnourished children 2024 articles Malnourished children Scopus articles Malnourished children impact factor journals Malnourished children Scopus journals Malnourished children PubMed journals Malnourished children medical journals Malnourished children free journals Malnourished children best journals Malnourished children top journals Malnourished children free medical journals Malnourished children famous journals Malnourished children Google Scholar indexed journals child malnutrition articles child malnutrition Research articles child malnutrition review articles child malnutrition PubMed articles child malnutrition PubMed Central articles child malnutrition 2023 articles child malnutrition 2024 articles child malnutrition Scopus articles child malnutrition impact factor journals child malnutrition Scopus journals child malnutrition PubMed journals child malnutrition medical journals child malnutrition free journals child malnutrition best journals child malnutrition top journals child malnutrition free medical journals child malnutrition famous journals child malnutrition Google Scholar indexed journals Urban market articles Urban market Research articles Urban market review articles Urban market PubMed articles Urban market PubMed Central articles Urban market 2023 articles Urban market 2024 articles Urban market Scopus articles Urban market impact factor journals Urban market Scopus journals Urban market PubMed journals Urban market medical journals Urban market free journals Urban market best journals Urban market top journals Urban market free medical journals Urban market famous journals Urban market Google Scholar indexed journals Respiratory tract infections articles Respiratory tract infections Research articles Respiratory tract infections review articles Respiratory tract infections PubMed articles Respiratory tract infections PubMed Central articles Respiratory tract infections 2023 articles Respiratory tract infections 2024 articles Respiratory tract infections Scopus articles Respiratory tract infections impact factor journals Respiratory tract infections Scopus journals Respiratory tract infections PubMed journals Respiratory tract infections medical journals Respiratory tract infections free journals Respiratory tract infections best journals Respiratory tract infections top journals Respiratory tract infections free medical journals Respiratory tract infections famous journals Respiratory tract infections Google Scholar indexed journals Digestive infections articles Digestive infections Research articles Digestive infections review articles Digestive infections PubMed articles Digestive infections PubMed Central articles Digestive infections 2023 articles Digestive infections 2024 articles Digestive infections Scopus articles Digestive infections impact factor journals Digestive infections Scopus journals Digestive infections PubMed journals Digestive infections medical journals Digestive infections free journals Digestive infections best journals Digestive infections top journals Digestive infections free medical journals Digestive infections famous journals Digestive infections Google Scholar indexed journals Pulmonary infections articles Pulmonary infections Research articles Pulmonary infections review articles Pulmonary infections PubMed articles Pulmonary infections PubMed Central articles Pulmonary infections 2023 articles Pulmonary infections 2024 articles Pulmonary infections Scopus articles Pulmonary infections impact factor journals Pulmonary infections Scopus journals Pulmonary infections PubMed journals Pulmonary infections medical journals Pulmonary infections free journals Pulmonary infections best journals Pulmonary infections top journals Pulmonary infections free medical journals Pulmonary infections famous journals Pulmonary infections Google Scholar indexed journals
Article Details
1. Introduction
Malnutrition is a pathological state resulting from absolute or relative deficiency or excessive of one or more essential nutrients, whether manifested clinically of detectable only by anthropometric or physiological biochemical analysis [1]. It is one of the main public health challenges in developing countries [2]. Worldwide, 56 % of deaths among under 5 years of age are attributable to malnutrition [3]. In Africa, the prevalence is 20 %, 39 % of which are in Sub-Saharan Africa [4,5]. In Senegal, in 2018, 19% of children under the age of five were stunted, 8% were wasted and 15% were underweight. Very few studies have been conducted on malnutrition in the city of Ziguinchor, in the Southern Senegal, where we continue to wonder about the real impact of this disease. The aim of the study was to assess the nutritional status of children aged 6-59 in two hospitals in the city of Ziguinchor.
2. Materials and Methods
2.1 Study design and area
This was a prospective two-center analytical study aimed at nutritional assessment of children aged 6 to 59 months examined in consultations or admitted to two hospitals in the city of Ziguinchor for a period of 4 months from December 1, 2020 to 1 March 2021. Ziguinchor city has two hospitals classified as level 2 hospitals according to the Senegal health pyramid, the regional and peace hospitals, both separated from about 1 km. In addition, Ziguinchor is the rainiest city in the country. The landscape is green and the main activities are agriculture, fishing and livestock.
2.2 Study population
All children aged 6-59 months, seen at consultation or admitted in the paediatrics wards of the 2 hospitals and who had parental consent for the study were included in this work. We excluded from our study children whose parents did not consent and those who did not meet the age criteria.
2.3 Data collection
For each enrolled child, we used a data collection form that recorded child and parent’s information. The following parameters were collected and analysed:
In children: Age, gender, vaccination status, weight for height, weight for age, height for age indices, concomitant pathologies and the outcome
In mother: Age, education level, marital status
In father: Profession, Residence, socio economic level
The indicators wasting, stunting, and underweight were following WHO standard definitions. The socio economic level was considered low if parents did not have access to drinking water and electricity. Anthropometric parameters were determined based on WHO criteria and tools
2.4 Data analysis
The data were analysed using Epi info 7 statistical software. proportions were compared using Pearson Chi² or Fisher’s exact test depending on validity conditions with a P value <0.05 considered as statistically significant.
3. Results
3.1 Epidemiological data
137 children were enrolled in the paediatric wards of two hospitals of which 103 were in regional hospital and 34 in peace hospital. The sex ratio was 1, 28 in favour of boys. Children age average was 22.4 ±12.9 months with 67, 9 % of children under 24 months. According to the Expended program on immunization in Senegal, children’s vaccination status were completed in 98% of cases. 98, 1% of mothers were over 20 years old, and almost half (46%) were over 30 years old. In 53, 7 % of cases, the education level was low. More than half of parents (76, 6%) had a poor socio economic level and 59, 3% were from rural areas. Fathers were unemployed in 38, 9% (Figure 1).
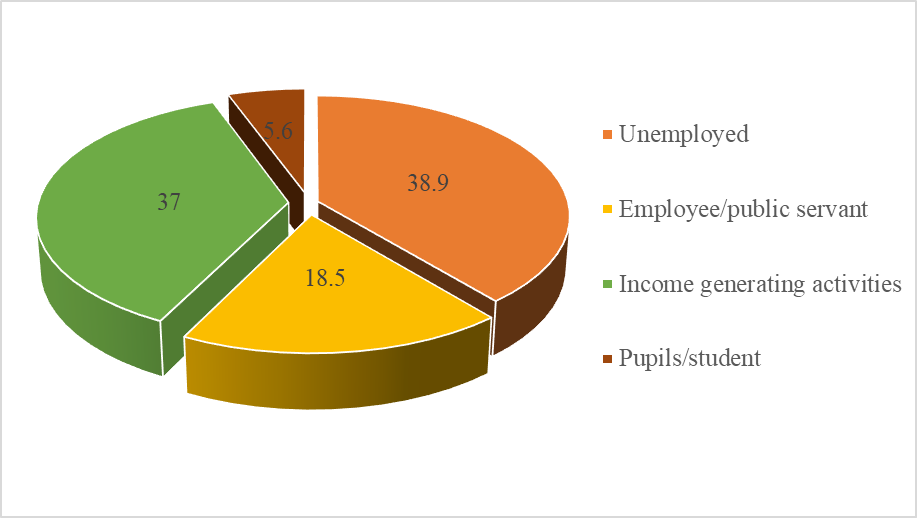
Figure 1: Distribution of malnourished children according to fathers professional activity.
In hospitalized children, 70,3% of infectious complications occurred, mainly acute gastroenteritis (33,3%) and pneumonia (11,1%).
3.2 Nutritional data
|
Indicators |
Nutritional status |
Effective |
Percentage (%) |
|
Weight/Height (z-score) |
|||
|
> –2 |
Normal |
108 |
78,8 |
|
–3 et –2 |
Moderate malnutrition |
13 |
9,5 |
|
< –3 |
Severe acute malnutrition |
16 |
11,7 |
|
Total |
137 |
100 |
|
|
MUAC (cm) |
|||
|
≥ 12,5 |
Normal |
111 |
81 |
|
11,5–12,5 |
Moderate acute malnutrition |
17 |
12,4 |
|
< 11,5 |
Severe acute Malnutrition |
9 |
6,6 |
|
Total |
137 |
100 |
|
|
Height/Age (z-score) |
|||
|
> –2 |
Normal |
112 |
81,8 |
|
–3 et –2 |
Moderate stunting |
15 |
10,9 |
|
< –3 |
Severe stunting |
10 |
7,3 |
|
Total |
137 |
100 |
|
|
Weight/Age (z-score) |
|||
|
> –2 |
Normal |
113 |
82,5 |
|
–3 Z et –2 |
Moderate under nutrition |
13 |
9,5 |
|
< –3 |
Severe under nutrition |
11 |
8 |
|
Total |
137 |
100 |
|
Table 1: Distribution of children anthropometric parameters.
3.3 Data on malnourished children
54 cases of malnutrition were diagnosed with a prevalence of 39, 4 % of which 11, 7 % had severe acute malnutrition. The sex ratio was 1.2 favouring males. The age related malnutrition cases is shown in Table 2.
|
Age range |
Nutritional status |
Total |
P |
||
|
Normal |
Malnutrition |
||||
|
6-12 months |
n(%) |
18 (21,7) |
18 (33,3) |
36 (26,3) |
0,175 |
|
13-24 months |
n(%) |
37 (44,6) |
20 (37) |
57 (41,6) |
|
|
25-36 months |
n(%) |
15 (33,3) |
11 (20,4) |
26 (19) |
|
|
37-59 months |
n(%) |
13 (18,1) |
5 (9,3) |
18 (13,1) |
|
|
Total |
n(%) |
83 (60,6) |
54 (39,4) |
137 (100) |
|
Table 2: distribution of nutritional status according to children’s age.
Almost all (94,4%) malnourished children were fully vaccinated. 90,7% of theirs mothers were married and 46.3% over 30 years of age. On the other hand, 31, 5% of mothers had no education and only 22% obtained low level of education. In the same vein, 38,9% of cases, fathers were unemployed. Furthermore, 59,3% malnourished children were from rural areas meanwhile in 79,6% of cases, the socio economic situation of their parents was poor. Half (50%) of the 36,4% malnourished children were followed as outpatients, while the remaining were in paediatrics wards. No death case was reported.
4. Discussion
The prevalence of malnutrition in this work was 39.4% of which 11.9% were severe acute malnutrition. This finding was similar to the those reported in 2010 by the MICS ( multiple indicators clusters surveys ) conducted on different regions of Mali where 6,8% of severe malnutrition cases occurred at Kaye, 9,4% at Koulikoro, 10,9% at Gao and 12,5 % à Ségou [7]. In Guinea, the prevalence of acute malnutrition in 2006 was 12% [8]. Much higher prevalence (63,1%) was reported in Chad with 37 % accounting for severe forms [10]. However an Algerian study revealed much lower prevalence (2,8%) of which 0, 6% were severe forms [9].
In our study the stunting percentage was 18.2%, of which 7.3% were severe forms. This finding was similar to values found in Algeria and Chad with stunting percentages respectively of 18% and 16, 1% [9,10]. Agbere et al. [11] found 22, 4% of children with moderate stunting and 44.6% with severe stunting [11]. It should be noted that in Senegal the mean stunting percentage is 9.1% for children aged 6 to 59 months [12].
The prevalence of under nutrition was 17, 5% of which 8% was severe form. Much higher rate (38, 02%) was found by Agbere et al [11] of which 12, 5% was severe under nutrition [11]. Similarly, Kante [13] showed 46% of under nutrition cases of which 31% were severe forms [13].On the other hand, much lower rates 6% were revealed in Algeria of which 1, 3% represented the severe forms.
In this study, almost all mothers (98,1%) of malnourished children aged above 20 years. In the same trend, Kanté [13] found 81, 9 % while on the hand, Ake Tano et al. [14] reported that only 60 % of mothers were over 20 years old. 53, 7% mothers of malnourished children in this study had a low education level and that was statistically significant (P=0.014).
There is close link between mothers’ educational level and child malnutrition explained by the fact that valuable nutritional knowledge, attitudes and practices of mothers brings satisfaction towards child nutritional needs. More often, the higher the mothers’ education, the more they appreciate these various nutritional child needs in a timely manner and provide the appropriate response.
In this work 38,9% fathers of malnourished children were unemployed. Much higher (51%) percentage was found in Mali in 2020 by Guindo [15]. We also reported that 59,3% of malnourished children came from rural areas. Malnutrition is greater in rural areas than urban areas [16]. This difference can be explained by the availability and diversity of food products on the urban market. Parents’ low socio-economic status has also been associated with malnutrition. In 79,6% of cases, parents in this study had a poor socio economic status.
There is a close relation between malnutrition (under), respiratory tract infections, digestive infections and HIV in children [17]. This was highlighted in our study where we found 33,3% of acute gastroenteritis, 11,1% acute respiratory tract infections and 11.1% HIV cases. Similarly, Guindo M in Mali found 41,7% cases of acute gastroenteritis and 30,2% cases respiratory infection[15]. Pulmonary infection is a frequent complication of malnutrition as demonstrated by Sow in Senegal who reported 26.6% of respiratory tract infections among malnourished children.
The sex ratio 1.2 in the study favored male gender. There is substantial overlap between the result of this study and those reported by the Smart survey [20] and the Central African Republic children nutritional status. However, Diarra reported a female predominance [22]. 70.3 % of children aged 6-24 months were malnourished. This same trend (89.6%) was observed by Guindo [15]. Indeed, introduction of complementary feeding and weaning occurs at this period. However, early pregnancies, poor socio-economic status and cultural beliefs restrict good practices [23]. Complete vaccination does not exclude malnutrition. Actually, 94.4% of malnourished children in this study were fully vaccinated. Many authors had the same findings [24,25].
In this study 19,7% of malnourished children fully recovered and no death cases were reported. Sissoko [26] found a much lower percentage (8.6%). This can be explained by our low sample size but also low patients’ attendance across health facilities during COVID 19 pandemic.
5. Conclusion
Knowledge of good attitudes and practices towards child nutrition as well as improving the quality of life of populations must be a public health priority in developing countries like Senegal. Our work results provide a data base that can help putting in place or improve corrective actions on children malnutrition at the local, regional and national level.
References
- Jelliffe DB. Assessment of the nutritional status of populations (mainly by survey) in developing countries. Geneva: WHO 53 (1969): 286.
- N'Diaye S, Ayad M. Demographic and health survey, Senegal 2005. Ministry of Health and Medical Prevention, Research Center for Human Development 487 (2006).
- Nutrition Highlight of recent activities in the context of the World Declaration and plan of action for nutrition. WHO/NUT/95.2 (1995): 3-4.
- Aubry P, Gauzère BA. Protein energy malnutrition. Diploma in tropical medicine from Indian Ocean countries. Med Trop 27 (2020): 1-13.
- The State of World Food and Agriculture 2001. Food and Agriculture Organization of the United Nations [online]. [Accessed June 1, 2021]; available at: https://dhsprogram.com/pubs/pdf/FR197/12Chaptre12.pdf. Food & Agriculture Org 2001; 33:313.
- National Agency for Statistics and Demography (ANSD). Senegal, Demographic and Continuous Health Survey (EDS-Continue 2018) (2020): 454.
- Ministry of Health. MICS survey report from 2010 Mali; nutrition component 20.
- Mondot Bernard J. Malnutrition, the scourge of early childhood. Nutrition and diet [online]; [accessed June 1, 2021] Paris: CIHEAM (Mediterranean Options; no. 29); available at: http://om.ciheam.org/om/pdf/r29/CI010627 1975 (75-79).
- National Institute of Public Health (Algeria). Survey on the objectives of the end of the decade: maternal and child health. EDG Algeria 2OOO/MICS2, Summary report (2001): 187.
- Renaudin P. Assessment of the nutritional status of children under 5 years old in Moundou, Chad. Semantics Scholar 57 (1997): 49-54.
- Agbere AR. Infant and young child feeding practices. Standard operating procedures for the management of breast milk substitutes for children 0 to 23 months in refugee situations. UNHCR 48 (2015).
- Fall AS, Savy M, Seye M, et al. Causal study of the persistence of malnutrition and food insecurity in the regions of Matam, Kolda, Sedhiou , Ziguinchor and the department of Podor. Final Report (2014).
- Kanté L. Evaluation of the nutritional status of children aged 2 to 59 months, hospitalized in the paediatric department of CHU Gabriel Touré. University of Bamako; Med. Thesis, Bamako (2008): 82.
- Ake-Tano O, Tiembé I, Konan Y, et al. Chronic malnutrition among children under 5 years old in northern Ivory Cost. Public health 22 (2010): 213-220.
- Guindo M. Severe acute malnutrition with complication in children aged 6 to 59 months in the paediatric department of Nianankoro hospital Fomba of Segou. University of Sciences, Techniques and Technologies of Bamako (USTTB); Med. Thesis, Bamako (2020): 110.
- Tanang TP. Explanatory factors of malnutrition among children under five years of age in Cameroon. Yaoundé: Professional Master's Thesis in Demography (2009).
- Jesson J. Malnutrition and paediatric HIV infection in West Africa [online]; [accessed June 1, 2021] HAL. available at: https://tel.archives-ouvertes.fr/tel-01474730/document (2017): 235.
- Azoumah KD, Guedehoussou T, Tsolenyanu E, et al. Epidemiological and diagnostic aspects of severe acute malnutrition in children under 5 years of age in the commune of Kara. African Journals Online 14 (2012): Series D.
- Sow D. Malnutrition and infection - Epidemiological aspects. Med Afr Black 36 (1989): 360-366.
- Government of the Republic of Mali. Retrospective nutritional and mortality survey, Mali 2012. SMART Mali (2012).
- Litte-Ngounde E. Impact of women's educational level on the nutritional status of children under three in the Central African Republic. IFORD; DESSD dissertation, Yaoundé, 2004: 26th Promotion 104.
- Diarra I. Evaluation of the management of severe acute malnutrition in children aged 6 to 5 months at the URENI of the CS Ref Of Koutiala. University of Sciences, Techniques and Technologies of Bamako (USTTB); Med. Thesis, Bamako (2014): 87.
- Bouville JF. Relational aetiologies of childhood malnutrition in a tropical environment. Become 15 (2003): 27-47.
- Adedire EB, Ajayi I, Fawole OI, et al. Immunization coverage and its determinants among children aged 12-23 months in Atakumosa -west district, Osun State Nigeria: a cross-sectional study. BMC Public Health 16 (2016): 905.
- Toe A. Knowledge and practices of mothers of children aged 6 to 59 months regarding child nutrition at the URENI reference health center. Baroueli. University of Sciences, Techniques and Technologies of Bamako (USTTB); Med. Thesis, Bamako (2014): 80.
- Sissoko F. Review of URENI activities for severely malnourished children aged 0 to 59 months hospitalized in the paediatric department of CHU GT. Med. Thesis, Bamako 22 (2010): 75-76.
