Medication Errors in Neonatal Intensive Care Unit and Strengthening Education of Registered Nurses
Article Information
Sarmad Muhammad Soomar*, Roman Raees, Kiran Muhammad Abbas
Aga Khan University School of Nursing and Midwifery (AKUSONAM), Karachi Pakistan
*Corresponding Author: Sarmad Muhammad Soomar, Aga Khan University School of Nursing and Midwifery (AKUSONAM), Karachi Pakistan
Received: 24 July 2019; Accepted: 09 August 2019; Published: 12 August 2019
Citation:
Sarmad Muhammad Soomar, Roman Raees, Kiran Muhammad Abbas. Medication Errors in Neonatal Intensive Care Unit and Strengthening Education of Registered Nurses. Journal of Pediatrics, Perinatology and Child Health 3 (2019): 130-139.
Share at FacebookAbstract
Medication error is a very common issue of practice in hospitals. Involving nurses, doctors, administrators and pharmacy team there are a lot more loops into this very significant clinical issue. On a regular base, we see issues of medication and errors related to it in hospital setup. Unfortunately, these incidences sometimes cannot be prevented and proven as fatal and sentinel. Looking at the vulnerable populations like neonates, they are on more risk of getting effected by any of these errors as they are not immune enough or not that much stronger to bear these consequences and the body responds quickly in a negative manner to these errors. Role of nurses in identifying this kind of issue at any level and intervening it, is very essential. In addition, nurses’ role as educator and advocate become very much highlighted here and for that purpose they need to seek support from team, colleagues and leadership in the clinical area. Also, timely referring to resources like medication books, pamphlets or posters for understanding of common medication and their related information is very essential. Continuous session and debriefings on discussing concentrations, infusions, mathematical calculations of dosage and reviewing electronic systems would be beneficial for them. The paper identifies this issue as significant and discusses about insights from an academic project and details retrieved from a simple survey form created during the project and filled by the Registered Nurses in the neonatal intensive care unit of a tertiary teaching hospital. The project concluded with the implementation of creating resources and educational strengthening of the nurses and the paper mentions about it as well.
Keywords
Medication, Error, Neonate, Nurse, Incidences, Quality, Healthcare
Medication articles, Error, Neonate articles, Nurse articles, Incidences articles, Quality articles, Healthcare articles
Article Details
Abbreviations:
EMAR-Electronic Medical Administration Record; BCS-Bar Code Scan; NICU-Neonate Intensive Care Unit; RNs-Registered Nurses1. Introduction
For quality assurance purpose, there are different protocols in various tertiary hospitals. Medication error prevention and their safe handling is one of the essential practices which is standardized and recommended by majority of quality assurance institution. To maintain these quality protocols, hospital management’s responsibility is to do strategic planning [1]. It has seen that majority of the medical errors done in a practice setting comprise of the errors of medicine preparation or administration [2]. When it comes to neonates it’s highly risky and in literature, it has said to be 8 times more harm providing in comparison of adults [3]. This is why a proper understanding on the medication preparation (dose, dilution, calculation, compatibility etc.) is necessary. To maintain this quality, Electronic Medical Administration Record (EMAR) with facility of Bar Code Scan (BCS) has been also introduced in hospitals in Pakistan. Including this technology has made this process smoother, easy and error free. In neonates it is widely seen that incorrect dilution, additional dosages, and misidentification of patients is done because of either in stress, hurry or far access to medication record [4].
The EMAR decreases this effort and bring the medication system near to bedside and the BSC brings a feasibility of checking and rechecking proper drug rights, and lock after a proper process of administration. Thus, it decreases chances of error and increases quality of patient care. Also, it’s a moral and professional responsibility of nurses, that where these systems are not available they should strive to know the basic processes of drug preparation and administration so the harm of patient can be decreased at a higher extent [5]. They must know about the information that is related to specific medication used in their clinical areas like Neonate Intensive Care Unit (NICU). Newborn patients require the right care at first place for their survival. The neonates born preterm are often surrounded by multiple health problems which make them dependent on healthcare facilities to save their lives [6]. The holistic treatment influences the health outcome and plays a significant role to promote early recovery in neonates. They are too small and vulnerable due to low immunity, that any significant error during care provision can prolong their hospital stay leading to morbidity and mortality [7].
Medication error is considered as the most widely recognized among the additional recorded errors in NICU proven to increase the risk of injury. Medication errors are defined as an event occurred due to an error in prescription, dispense and/ or in an administration process of a medication leading to adverse consequences of a drug dose and its effects at maximum to patients of any age [8]. When it comes to neonates, pharmacotherapy is important in newborns to generate therapeutic effects to neonatal indications that should cautiously be administered after a proper drug dose calculation and to be monitored for their desired results [9]. Neonates produce responses to lower drug dose in comparison to an adult, as their developing organ limits their capacity to metabolize drugs [10]. The medication process in NICU is more cautiously performed as the dose gets prepared in specific dilutions, depending on the weight and the condition of neonates. They are so delicate and receptive in showing sensitivity at a shorter drug exposure that any minute change of decimals can bring huge hazards leading to sentinel clinical events [11]. It becomes very sudden and easy during drug preparation to create a mistake and cause any error that can change the formulation of the drug and affect the dosage, leading to toxicity [12]. Toxicity in the early period of neonatal life
can interfere with their growth and developmental phases, which is not at all good for their future functioning [13].
1.1 Clinical significance
Medication Administration and nursing are paired like anything, they never get separated in any context. They are never seen alone, where you hear about nursing, especially clinical nursing and in the context of Pakistan, medicine or medication administration comes in every one’s mind. Nurses’ have been a key person in healthcare who are responsible for medication preparation, administrating and disposal. Not with adults, children, or women, but with babies of neonatal intensive care unit (NICU), nurses are masters of all sort of work with medication. Still, after this expertise nurses are considered as personal responsible for medication errors among health care staff. Either with high dosages, administering medicine to wrong patients, or picking up an incorrect medicine, nurses have been listed as one of culprit in literature who are related to errors of the medication. Even though the high quality standard protocols, equipment and digital medication systems have been introduced to maintain quality of work, but still chances of error remain and that actually occurs. Mistakes with adults in medication preparation and administration are very impactful, so it’s imagined that how impactful it could be with Neonates.
Since in Pakistan EMAR and BCS are introduced and are in practice, it is very important to work on it in the relevant clinical setting to make a best use of it. Nurses have learned through their academic programs and pre job orientations about these systems and the clinical leadership and service setting management also provides lots of educational stuff related to this for nurses’ convenience. But due to busy schedules, many cannot read those charts or papers. Also, the recurrent addition of new nurses in the area creates a vacuum and they require follow up on the knowledge learnt in their orientation related to EMAR, BCS and other relevant medication preparation and administration related guidelines. Also, it is very less seen the addition of any separate NICU related program in nursing academic courses or orientation program which has details about differences in adult and neonate drug administration and preparation modes and methods. The clinical significance of this basic study along with an educational program for NICU nurses regard medication administration and EMAR was very much highlighted and that is why it was emphasized to implement in the clinical setup of NICU.
2. Literature Review
Administering medication in busy long shifts is challenging as this requires a comprehensive communication among RNs to break the chain of error and protect neonate’s life [14]. Their practices are expected to be vigilant and organized to operate by following the fundamental principles to perform medication process. However, medication errors are the end results of some known factors in healthcare settings [15]. These factors can be categorized commonly as [16]:
- Increased workload of RNs dealing with multiple admissions, shifts and assignments, making themselves inattentive to review drugs before administrating.
- The level of staff expertise varies with the practice and experience, for example the major errors might happen from a novice nurse rather from a senior RN. Although, experience doesn’t guarantee, in any case that senior RNs can never admit errors in medications preparation or administration.
- Many healthcare facilities offer medication administration via uncertified professionals that are unsafe and illegal. These facilities have no proper administration record or no any filing for medication prescription and administration. EMAR is a huge Information technology support in this case, which keeps a track of doctor, nurse and pharmacist at a similar time making a loop of medication safety.
- It has been found that often staff’s practice medicine through different techniques in different steps as they lack expert training in neonatal management, which ultimately fails to follow the medication administration safety policies in professional practice intended to ensure greater impact on lives.
The medications used in a particular country, including their formulation and determined doses depend upon the availability and convenience of a drug in different areas and the guidelines of NICU can also show the variation in the utilization of drug at different units [17]. Medication safety remains the concern to ensure the effective utilization of drug in the right conditions. The type of medication error in NICU includes prescribed errors that usually occur when a wrong drug is prescribed to a wrong patient, through a wrong route, at the wrong time without keeping in consideration patient tolerance and their individual factors such as age, weight, allergies, comorbidities, and previously administered drug record [18]. It’s a significant concern that many doctors prescribe the drug while they lack adequate information about the drug mechanism of actions and their interactions with other drugs. The neonate routinely gets treated with initial high doses in this type of situations and often with incorrect medication prescriptions that turns into a clear problem due to either ineffective communication or improper check while preparation and administration [19]. In addition, it is seen that RNs due to fear of being labeled as incompetent don’t seek help from instructors, heads or colleagues on the clinical floor while preparing drugs. In certain cases this increases the chances of error and brings harmful impacts [20].
The setup where we were processing the survey has more or less this kind of situation. Also, they have no any substitutes like booklets, charts or posters in the setup where they can refer to drug dosages or calculation matrix, if they are not seeking help from anyone during preparation. Medication safety is recognized with the five (5) rights of medication preparation and administration. This practice safeguards healthcare professionals from doing and error and patients from getting potential and unintended harm [21]. These rights include right patient, right drug, right dosage, right route and right time. Documentation has eventually become another right in order to have a clinical record and safety both at similar time. Using EMAR and BCS systems improves this quality of work and decreases the harm by serving as an online record or documentation. RNs who are licensed to work on medications are expected to fill out nursing notes as well to ensure the correct details of medication and any related incidences either positive or negative relating to that administration experience. In addition, taking care identifying patients with their correct name and complete names or possible the medical record numbers is another quality standard for safety [22].
The patient’s drug administration time varies in consideration to the demands and their response to doses. It is critical to check doctor’s order prior to prepare the right medication at the right time. This will allow neonates to gradually get settled with their medication regime and will allow a nurse to prepare medication right before administration to keep the patient away from any unsafe drug administration. This is also recommended that nurses should use their role of advocates whenever they feel something is not proper, while reviewing the orders [23]. Many researches indicated that 96% of nurses and more than 90% of doctors, hospital administrators and pharmacists believed that nurses have a primary responsibility to ensure patient safety. Nurses have identified many risky practices and errors and have notified these errors to prevent them in future. NICU nurses are trained to perform basic and advanced life care procedures responsible to practice safe medication with the right knowledge and practice to minimize the medication error in NICU’s. The Neonatal Intensive Care Units should promote the application of 5 rights of medication administration in their care to meet their vision of quality care provision for human survival [24].
2.1 Theoretical integration
The occurrence of errors in medicine weakens the personal and systemic approach to maintain institutional integrity with the patients. The origin of these unsafe acts can pursue repetitive patterns of incidence to trigger adverse events in error management. Thus, this kind of situation may create a serious loss of life, occupational insecurity and institutional quality.
In the following paper, the integration of the theme best suits with the commonly known model, the Swiss cheese model of system accidents, which describes the systemic approach. The model has its defined defensive boundaries to safeguard from hazards. This key of boundaries comprises secured physical barriers, control alarms, and procedures with protected room operators structured with the ideal consideration of technology to keep up the defensive layers in avoidance of errors. These guarded layers are similar to a slice of Swiss cheese with some holes that open and shut their area in layers. This shifting of holes in a layer is not a sign of a bad outcome until the holes in many defensive layers get aligned to cause an accident carrying risk to patients, such as a medication error reported due to the wrong prescription and was administered without keeping five rights of administration in consideration. These multiple holes in the defensive boundaries are more likely to cause potential damage. These holes in defensive layers arise from two variables: Active failures and latent conditions. Active failures involve unsafe acts committed by the people who are in direct contact with the patients, such as wrong medication administration documentation, procedural violation and any attempt leading to active failures when in contact to neonate can increase the error risk. Latent failures involve contributing factors that can produce adverse effects such as understaffing, resource allocation issues, long shifting’s and less expertise which can weaken the defensive barrier of a system. The effective defenses in personal and systemic approach can limit the chances of active and latent failures for successful outcomes in error management [25].
3. Methodology
In order to identify the understanding of nurses working in the setting of NICU, a survey form with likert scale was created on Google forms and provided to nurses in the area to fill it out. This provided us with a maximum understanding about what are the usual practices of nurses, which make them vulnerable to attempt medication errors. The form comprised of 17 general questions, mostly including specific NICU drugs related help seeking behaviors of nurses, while preparing dilution. This will also give us an idea that which drug is more complicated to prepare or which drug has mostly seen to be difficult in preparation leading to errors. From the total number of nurses present, nineteen (n=19) consented to fill the survey form which included both male and female Registered Nurses (RNs).
4. Results and Discussion
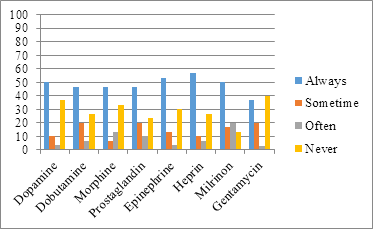
The survey has two main portions as discussed in the methodology. The majority part (from question 1-8) inquires about the responses of RNs in NICU regarding the need of assistance while preparing or making any of these commonly prepared infusions in NICU. These common medicines/infusions include dopamine, dobutamine, morphine, prostaglandin, epinephrine, heparin, milrinon and gentamycin (1-8 respectively). It was evident that more than half of the registered nurses always had issues in preparing Heparin and Epinephrine in the NICU setting and required assistance. Also, most of the RNS had no requirement of help and assistance when they are preparing gentamycin (Figure 1).
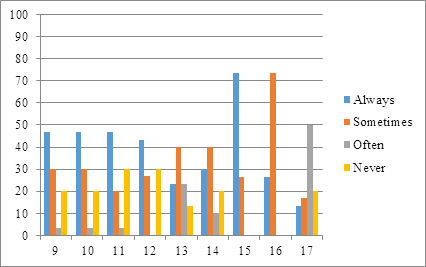
In the remaining part of the survey (from question 9-17) inquires for other details where almost half of the RNs have considered that they help their colleagues while they are preparing infusion’s concentration (Q9), they need any help themselves too from colleague, instructor or head while preparing (Q 10), they have required assistance for conforming volumes while making infusion’s concentration (Q 11) and they have also needed help while taking mcg/mg from ampule for making concentration (Q 12). While some other important details were very less practiced, always, which actually should be practiced every time. These showed that very less RNs always needed someone’s help to know the adverse effects (Q 13) and alarming signs (Q 14) of medicines which are used in NICU. Unfortunately, it is not necessary that nurse remember these details everytime, which are difficult and huge to memorize. Majority of the RNs considered are always fine in managing with EMAR and BCS system and few have still some issues (Q 15). Also, it was very significant from the results that more than half RNs have sometimes utilized the five rights methods or rechecked 5 rights while administering the medication, which is comparatively better, but not a majority of RNs do this practice always (Q 16). Lastly, it was a very different response to notice that very few RNs commonly realize about making an error through their negligence during medication preparation or administration and it was seen that almost half consider that they often realize this thing (Q 17) (Figure 2).
The results provided different types of results from the survey as we want nurses to practice these things every time through any source like enhancing their knowledge, referring to a document or pamphlets, considering colleagues or administration as help, etc. On the basis of this, educational sessions was organized and implemented to strengthen the learning and fill the educational gap of RNs at NICU regarding medication error. Other resources for referral purpose were also created.
5. Implementation Highlights
Since neonate are very sensitive to drug dosage, so all these medications are prescribed on the basis of 24 hours and physician prescribe those medicines as ml/hr and share with nurses. In NICU setup where we work, the protocol is more vigilant as the dosages are decided according to the body weight of the neonate. It can be very harmful if the infusions are incorrectly calculated or not rechecked during preparation or administration. Also, providing medication to an incorrect patient would be similarly harmful. On the basis of survey and needs, assessment is done including the regular clinical observation verified by clinical administration and faculty mentors, the educational sessions along with creating educational resources was the main project implementation highlight.
The main goals of the educational program were using EMAR and BCS properly along with remembering few basic NICU related medications and their adverse effect, mechanism of administration, compatibility and usage while administration. This need was also fulfilled their preparation of educational resources like booklet, posters and online presentation for referring. The booklet contained very detail snap shot of the processes, including EMAR and BCS usage and currently the video resources and online module is in progress which will support these nurses to revisit their concepts and enhance their learning regarding commonly used medications in NICU. Some of the cue cards were also prepared which contains the medication dilution and dosage related quick information. Since the observations were essential in terms of evaluation as they were important during the need assessment. The outcome measuring indicator was itself our observation and supervision of clinical administration. After providing these facilitation sessions and educational materials, we tend to observe the RNs to practice these learning and revisit their concepts. We encouraged them to seek help when required instead of provoking a potential medication error. The project is very significant and impact generating in its kind. As it will not only improve knowledge of nurses, but practices that will ultimately impact neonatal health and improve the family stratification, quality care and poor health indicators of Pakistan. The management will have an additional responsibility to observe the practices keenly, as they always do.
6. Recommendations and Conclusion
In the lieu of following, study and program, our team would like to recommend that neonatal risk management trainings should be arranged and the role and practices of neonatal nurse practitioners should be strengthen. Medication prescribed by the doctor must be double checked by the entire team before administration and nurses must be well aware of their patient’s medications actions and reactions. Using EMAR should be a compulsory learning skills for nurses at the electronic system provide a good time margin for recheck king and detects errors that we potentially miss. Reporting system of error in an electronic manner along with copying the report in patient file should be another practice to introduce in order to keep a record of how often clients especially neonates, suffer from these situations and minimizing that should be the priority goal of healthcare team.
A quality practice is when medication is received, prepared, administered and discarded by the RN who is assigned on the particular neonate. Take nurse instructors or head nurses for support in case you need. Eradicate the practice of providing non licensed people the responsibility to administrate medication of neonates. Make sure RNs do not trust anyone in terms of medication preparation or administration even you know them much better. They should get an opportunity to get involved in clinical decision making to make decisions based on patient condition rather to only rely on prescribed orders. This strategy will allow healthcare professionals to work as a team in promoting the patient’s recovery and minimize any error. The team leader must utilize own interpersonal skills to develop the strategies to meet the important quality parameters. The transformational leadership style is significant in building vision among nurses and doctors in the adaptation of positive behaviors to work together in a collaborative environment. Further researches need to be done to develop and implement effective equipment utilization strategies to avoid any medication error through equipment and specialized training for healthcare providers to maintain the sustainability of quality care.
Medication error can be lethal for patients if not get detected at the right moment, especially neonates. Each neonate tolerance and response to medication varies and it's critically important to recognize the trend of neonatal response to a specific drug and dose. The inappropriate preparation and administration of a drug more commonly lead to medication error that is picked by the nurses when the wrong drug is received to the wrong patient or get exchanged among the patients. This is high time where we can encourage nurses’ education, practice and help seeking from colleagues and management to minimize chance of error and improve the quality of care that our clients (neonates) deserve.
7. Acknowledgment
The following study was part of an academic project which was done during BSN course with the support of clinical administration and academic leaders in nursing who were mentoring our team to develop this educational program for NICU nurses based on the need assessment survey. We would like to acknowledge all of them who contributed in any way for the success of this project.
References
- Al-Jeraisy MI, Alanazi MQ, Abolfotouh MA. Medication prescribing errors in a pediatric inpatient tertiary care setting in Saudi Arabia. BMC research notes 4 (2011): 294.
- Al Anazi M, Al-Jeraisy M, Abolfotouh MA. Medication prescribing errors in a pediatric inpatient tertiary care setting in Saudi Arabia. Journal of Infection and Public Health 8 (2015): 395.
- Kaushal R, Bates DW, Landrigan C, et al. Medication errors and adverse drug events in pediatric inpatients. Jama 285 (2001): 2114-2120.
- Stavroudis TA, Shore AD, Morlock L, et al. NICU medication errors: identifying a risk profile for medication errors in the neonatal intensive care unit. Journal of Perinatology 30 (2010): 459.
- Sweis RJ, Ahmad KM, Al-Dweik GA, et al. The relationship between total quality management practices and organisational performance at Jordanian hospitals. International Journal of Business Innovation and Research 10 (2016): 519-542.
- Simpson JH, Lynch R, Grant J, et al. Reducing medication errors in the neonatal intensive care unit. Archives of Disease in Childhood-Fetal and Neonatal Edition 89 (2004): 480-482.
- Gray JE, Goldmann DA. Medication errors in the neonatal intensive care unit: special patients, unique issues. Archives of Disease in Childhood-Fetal and Neonatal Edition 89 (2004): 472-473.
- Stavroudis TA, Miller MR, Lehmann CU. Medication errors in neonates. Clinics in perinatology 35 (2008): 141-161.
- ELMeneza S, Habib A, Mohamed R. Analysis and identifying risk profile for medication errors in the neonatal intensive care units. EC Paediatr 7 (2018): 84.
- Pawluk S, Jaam M, Hazi F, et al. A description of medication errors reported by pharmacists in a neonatal intensive care unit. International journal of clinical pharmacy 39 (2017): 88-94.
- Greenberg RG, Smith PB, Bose C, et al. National survey of neonatal intensive care unit medication safety practices. American journal of perinatology 35 (2018): 1419-1422.
- Palmero D, Di Paolo ER, Stadelmann C, et al. Incident reports versus direct observation to identify medication errors and risk factors in hospitalised newborns. European journal of pediatrics 178 (2019): 259-266.
- Krzy?aniak N, Paw?owska I, Bajorek B. Review of drug utilization patterns in NICU s worldwide. Journal of clinical pharmacy and therapeutics 41 (2016): 612-620.
- Grissinger M, Gaunt MJ, Rich DS. Avoiding Medication Errors: Reducing Harm in Residents Using Oral Anticoagulants. The Consultant Pharmacist® 31 (2016): 294-303.
- Kelly LL. Medication error reporting: a qualitative study exploring student nurses’ anticipated peer reactions to error reporting (Doctoral dissertation, University of Alabama Libraries) (2018).
- Martyn JA, Paliadelis P, Perry C. The safe administration of medication: Nursing behaviours beyond the five-rights. Nurse education in practice 37 (2019): 109-114.
- Krzyzaniak N, Bajorek B. Medication safety in neonatal care: a review of medication errors among neonates. Therapeutic advances in drug safety 7 (2016): 102-119.
- Salami I, Subih M, Darwish R, et al. Medication Administration Errors: Perceptions of Jordanian Nurses. Journal of nursing care quality 34 (2019): 7-12.
- Edwards SL, Williams J, Lee M. Reducing drug errors by engaging student nurses in medication management simulation. Journal of Prescribing Practice 1 (2019): 344-355.
- Schoenly L. Safety for the nurse and the patient. Essentials of correctional nursing. New York: Springer 14 (2012): 55-79.
- Chapuis C, Roustit M, Bal G, et al. Automated drug dispensing system reduces medication errors in an intensive care setting. Critical care medicine 38 (2010): 2275-2281.
- Gates PJ, Meyerson SA, Baysari MT, et al. The prevalence of dose errors among paediatric patients in hospital wards with and without health information technology: A systematic review and meta-analysis. Drug safety 42 (2019): 13-25.
- Ni Y, Lingren T, Hall ES, et al. Designing and evaluating an automated system for real-time medication administration error detection in a neonatal intensive care unit. Journal of the American Medical Informatics Association 25 (2018): 555-563.
- Treiber LA, Jones JH. After the Medication Error: Recent Nursing Graduates' Reflections on Adequacy of Education. Journal of Nursing Education 57 (2018): 275-280.
- Armitage G. Human error theory: relevance to nurse management. Journal of nursing management 17 (2009): 193-202.