Delayed Diagnosis and Treatment of Simultaneous Bilateral Adnexal Torsion
Article Information
Misgav Rottenstreich, Reut Rotem, Fayez Khatib, Shunit Armon, Orna Reichman a, Sorina Grisaru-Granovsky, Hen Y Sela*
Department of Obstetrics and Gynecology, Hebrew University Medical School, Jerusalem, Israel
*Corresponding author: Hen Y Sela, Department of Obstetrics and Gynecology, Shaare Zedek Medical Center, 12 Bayit Street, Jerusalem, 91031, Israel
Received: 28 August 2020; Accepted: 04 September 2020; Published: 09 September 2020
Citation:
Misgav Rottenstreich, Reut Rotem, Fayez Khatib, Shunit Armon, Orna Reichman a, Sorina Grisaru-Granovsky, Hen Y Sela. Delayed Diagnosis and Treatment of Simultaneous Bilateral Adnexal Torsion. Journal of Women’s Health and Development 3 (2020): 376-378.
Share at FacebookAbstract
Adnexal torsion (AT) is a gynecologic emergency that requires prompt diagnosis and treatment to relieve patient symptoms and to achieve viable adnexa. We present a case that resulted in delayed diagnosis and treatment of simultaneous bilateral adnexal torsion most following the use of ART. Our delayed diagnosing resulted likely from the identical appearance of the ovaries on ultrasound and alternative diagnosis of ovarian hyperstimulation syndrome, an awareness to this rare phenomenon of simultaneous bilateral adnexal torsion might have helped to perform the surgery earlier.
Keywords
Adnexal torsion, Ovarian hyperstimulation syndrome, Ultrasound, Advanced reproductive technology
Adnexal torsion articles Adnexal torsion Research articles Adnexal torsion review articles Adnexal torsion PubMed articles Adnexal torsion PubMed Central articles Adnexal torsion 2023 articles Adnexal torsion 2024 articles Adnexal torsion Scopus articles Adnexal torsion impact factor journals Adnexal torsion Scopus journals Adnexal torsion PubMed journals Adnexal torsion medical journals Adnexal torsion free journals Adnexal torsion best journals Adnexal torsion top journals Adnexal torsion free medical journals Adnexal torsion famous journals Adnexal torsion Google Scholar indexed journals Ovarian hyperstimulation syndrome articles Ovarian hyperstimulation syndrome Research articles Ovarian hyperstimulation syndrome review articles Ovarian hyperstimulation syndrome PubMed articles Ovarian hyperstimulation syndrome PubMed Central articles Ovarian hyperstimulation syndrome 2023 articles Ovarian hyperstimulation syndrome 2024 articles Ovarian hyperstimulation syndrome Scopus articles Ovarian hyperstimulation syndrome impact factor journals Ovarian hyperstimulation syndrome Scopus journals Ovarian hyperstimulation syndrome PubMed journals Ovarian hyperstimulation syndrome medical journals Ovarian hyperstimulation syndrome free journals Ovarian hyperstimulation syndrome best journals Ovarian hyperstimulation syndrome top journals Ovarian hyperstimulation syndrome free medical journals Ovarian hyperstimulation syndrome famous journals Ovarian hyperstimulation syndrome Google Scholar indexed journals Ultrasound articles Ultrasound Research articles Ultrasound review articles Ultrasound PubMed articles Ultrasound PubMed Central articles Ultrasound 2023 articles Ultrasound 2024 articles Ultrasound Scopus articles Ultrasound impact factor journals Ultrasound Scopus journals Ultrasound PubMed journals Ultrasound medical journals Ultrasound free journals Ultrasound best journals Ultrasound top journals Ultrasound free medical journals Ultrasound famous journals Ultrasound Google Scholar indexed journals "Advanced reproductive technology articles Advanced reproductive technology Research articles Advanced reproductive technology review articles Advanced reproductive technology PubMed articles Advanced reproductive technology PubMed Central articles Advanced reproductive technology 2023 articles Advanced reproductive technology 2024 articles Advanced reproductive technology Scopus articles Advanced reproductive technology impact factor journals Advanced reproductive technology Scopus journals Advanced reproductive technology PubMed journals Advanced reproductive technology medical journals Advanced reproductive technology free journals Advanced reproductive technology best journals Advanced reproductive technology top journals Advanced reproductive technology free medical journals Advanced reproductive technology famous journals Advanced reproductive technology Google Scholar indexed journals " gynecologic articles gynecologic Research articles gynecologic review articles gynecologic PubMed articles gynecologic PubMed Central articles gynecologic 2023 articles gynecologic 2024 articles gynecologic Scopus articles gynecologic impact factor journals gynecologic Scopus journals gynecologic PubMed journals gynecologic medical journals gynecologic free journals gynecologic best journals gynecologic top journals gynecologic free medical journals gynecologic famous journals gynecologic Google Scholar indexed journals follicular articles follicular Research articles follicular review articles follicular PubMed articles follicular PubMed Central articles follicular 2023 articles follicular 2024 articles follicular Scopus articles follicular impact factor journals follicular Scopus journals follicular PubMed journals follicular medical journals follicular free journals follicular best journals follicular top journals follicular free medical journals follicular famous journals follicular Google Scholar indexed journals hyperstimulation articles hyperstimulation Research articles hyperstimulation review articles hyperstimulation PubMed articles hyperstimulation PubMed Central articles hyperstimulation 2023 articles hyperstimulation 2024 articles hyperstimulation Scopus articles hyperstimulation impact factor journals hyperstimulation Scopus journals hyperstimulation PubMed journals hyperstimulation medical journals hyperstimulation free journals hyperstimulation best journals hyperstimulation top journals hyperstimulation free medical journals hyperstimulation famous journals hyperstimulation Google Scholar indexed journals blastocyst articles blastocyst Research articles blastocyst review articles blastocyst PubMed articles blastocyst PubMed Central articles blastocyst 2023 articles blastocyst 2024 articles blastocyst Scopus articles blastocyst impact factor journals blastocyst Scopus journals blastocyst PubMed journals blastocyst medical journals blastocyst free journals blastocyst best journals blastocyst top journals blastocyst free medical journals blastocyst famous journals blastocyst Google Scholar indexed journals abdominal pain articles abdominal pain Research articles abdominal pain review articles abdominal pain PubMed articles abdominal pain PubMed Central articles abdominal pain 2023 articles abdominal pain 2024 articles abdominal pain Scopus articles abdominal pain impact factor journals abdominal pain Scopus journals abdominal pain PubMed journals abdominal pain medical journals abdominal pain free journals abdominal pain best journals abdominal pain top journals abdominal pain free medical journals abdominal pain famous journals abdominal pain Google Scholar indexed journals laparoscopy articles laparoscopy Research articles laparoscopy review articles laparoscopy PubMed articles laparoscopy PubMed Central articles laparoscopy 2023 articles laparoscopy 2024 articles laparoscopy Scopus articles laparoscopy impact factor journals laparoscopy Scopus journals laparoscopy PubMed journals laparoscopy medical journals laparoscopy free journals laparoscopy best journals laparoscopy top journals laparoscopy free medical journals laparoscopy famous journals laparoscopy Google Scholar indexed journals
Article Details
1. Introduction
Adnexal torsion (AT) is a gynecologic emergency accounting for 2.7 percent of emergency surgeries [1]. In 86-95% of women with AT ovarian mass exist, making it the primary risk factor for AT [2]. Ovulation induction and In Vitro Fertilization (IVF) occasionally results in the formation of large ovarian follicular cysts and, in some patients, massive ovarian enlargement due to hyperstimulation. Adnexal torsion may occur in women with ovarian hyperstimulation syndrome (OHSS) in up to 8% [3]. Prompt diagnosis and treatment of AT is of importance, in order to relieve patient symptoms and to have better chances of achieving viable adnexa for future fertility and quality of life.
2. Case Report
We present a case of a 41-years old G1P1 that was referred to our medical center eight days following an oocyte retrieval (9 oocytes) and one week after single blastocyst transfer due to lower abdominal pain, nausea and vomiting. Upon exam, her vital signs were normal; the abdomen was tender with rebound tenderness mostly on the left side. A trans-abdominal ultrasound revealed enlarged ovaries (right ovary measuring 8.7 × 6.2 cm; left ovary 6.5 × 4.9 cm) both had multiple peripheral follicles. In the Cul de sac there was mild amount of free fluid. Blood flow (arterial and venous) to both ovaries appeared normal and both ovaries appeared roughly the same (Image 1). Initial laboratory tests showed leukocytosis of 20.8×10ˆ3/uL, hematocrit of 35.4% and normal electrolytes. Initial impression was that it was a case of OHSS so she was treated with intravenous fluids and upon clinical improvement was discharged with a diagnosis of OHSS. She returned to the hospital within 12 hours with the same complains, her exam, vital signs, laboratory results and ultrasound exam were the same however due to an increasing abdominal pain we decided to proceed with a diagnostic laparoscopy. At the laparoscopy both ovaries were twisted, the right ovary was twisted twice and enlarged to 8 cm, the left ovary was twisted once and enlarged to 6 cm; it showed hemorrhagic and congestive changes, but no necrosis. The ovaries were untwisted and the large follicles were aspirated.
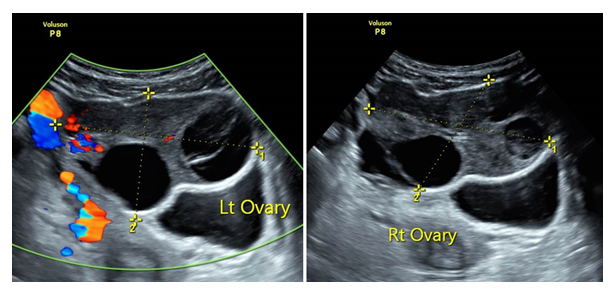
Figure 1: Transabdominal ultrasound revealed enlarged bilateral ovaries with multiple peripheral follicles. Doppler ultrasonography demonstrated normal ovarian blood flow.
3. Discussion
Pre-operative diagnosis of AT is often difficult to reach because of its non-specific symptoms and signs and the absence of precise laboratory and imaging findings. The Radiological Society of North America (RSNA) recommends to compare the gray-scale US appearance and flow of the contralateral ovary to aid significantly in diagnosis of ovarian torsion and that this should be performed at every examination [4]. Indeed Asynchronous bilateral AT may occur, however simultaneous bilateral AT is very rare [5]. We believe that the delayed diagnosis and treatment (12 hours) in our case stems from the lack of the classic ultrasound signs of AT : the presence of enlarged edematic ovary as oppose to contralateral normal ovary given the simultaneous bilateral torsion and the absence of normal contralateral adnexa to compare an AT, we misdiagnosed her as suffering from OHSS. Awareness to this possible but rare presentation of bilateral AT and lack of classical US signs should be kept in mind especially in the case of women undergoing artificial reproductive technologies.
Acknowledgements
Patient consent form has been completed and signed by the patient.
Disclosure Statement
All authors have no conflict of interest or benefit that has arisen from the direct applications this research to disclose.
Funding
None of the authors have any direct or indirect financial incentive associated with publishing the article.
References
- Hibbard LT. Adnexal torsion. Am J Obstet Gynecol 152 (1985): 456-461.
- White M, Stella Ovarian torsion: 10-year perspective. Emerg Med Australas 17 (2005): 231-237.
- Gorkemli H, Camus M, Clasen K. Adnexal torsion after gonadotrophin ovulation induction for IVF or ICSI and its conservative treatment. Arch Gynecol Obstet 267 (2002): 4-6.
- Chang HC, Bhatt S, Dogra VS. Pearls and pitfalls in diagnosis of ovarian torsion. Radiographics 28 (2008): 1355-1368.
- Wafa Al Omari, Saad Ghazal-Aswad, Islam H Sidky, Maha Khalid Al Bassam. Ovarian salvage in bilaterally complicated severe ovarian hyperstimulation syndrome. Fertil Steril 96 (2011): e77-e79.
