Complex Pneumosinus Dilatans Frontalis and CSOM associated with Cranial Fibrous Dysplasia
Article Information
Sabujan Sainudeen1*, Asmi M2, Methil Pradeep3
1Department of Radiology, Thangam Hospital, Palakkad, Kerala, India
2Department of Radiology, Malabar Scans & Research centre, Tirur, Kerala, India
3Department of Neurology, Thangam Hospital, Palakkad, Kerala, India
*Corresponding Author: Sabujan Sainudeen, Department of Radiology, Thangam Hospital, Palakkad, Kerala, India
Received: 02 June 2021; Accepted: 25 August 2021; Published: 16 September 2021
Citation: Sabujan Sainudeen, Asmi M, Methil Pradeep. Complex Pneumosinus Dilatans Frontalis and CSOM associated with Cranial Fibrous Dysplasia. Journal of Radiology and Clinical Imaging 4 (2021): 113-124.
Share at FacebookAbstract
Pneumosinus dilatans is a rare condition of abnormal dilatation of the paranasal sinuses. It can involve one or all of the sinuses. It may be developmental or associated with other conditions, mainly potentially obstructive lesions of the sinus cavity. Fibrous dysplasia is a benign condition in which the normal bone matrix is replaced by a disorganized fibrous tissue that involves craniofacial bones or peripheral skeleton. The entity may be a part of McCune-Albright syndrome or Mazabraud syndrome. Complications include extra skeletal manifestations like hyper functioning endocrinopathies and malignant transformation. Here we report a case of long-standing fibrous dysplasia leading to a frontal swelling due to complex dilatation of left frontal sinus- pneumosinus dilatans.
Keywords
Pneumosinus dilatans, Fibrous dysplasia, Fibro-osseous dysplasia, CSOM, Temporal bone, Imaging
Pneumosinus dilatans articles, Fibrous dysplasia articles, Fibro-osseous dysplasia articles, CSOM articles, Temporal bone articles, Imaging articles
Pneumosinus dilatans articles Pneumosinus dilatans Research articles Pneumosinus dilatans review articles Pneumosinus dilatans PubMed articles Pneumosinus dilatans PubMed Central articles Pneumosinus dilatans 2023 articles Pneumosinus dilatans 2024 articles Pneumosinus dilatans Scopus articles Pneumosinus dilatans impact factor journals Pneumosinus dilatans Scopus journals Pneumosinus dilatans PubMed journals Pneumosinus dilatans medical journals Pneumosinus dilatans free journals Pneumosinus dilatans best journals Pneumosinus dilatans top journals Pneumosinus dilatans free medical journals Pneumosinus dilatans famous journals Pneumosinus dilatans Google Scholar indexed journals Fibrous dysplasia articles Fibrous dysplasia Research articles Fibrous dysplasia review articles Fibrous dysplasia PubMed articles Fibrous dysplasia PubMed Central articles Fibrous dysplasia 2023 articles Fibrous dysplasia 2024 articles Fibrous dysplasia Scopus articles Fibrous dysplasia impact factor journals Fibrous dysplasia Scopus journals Fibrous dysplasia PubMed journals Fibrous dysplasia medical journals Fibrous dysplasia free journals Fibrous dysplasia best journals Fibrous dysplasia top journals Fibrous dysplasia free medical journals Fibrous dysplasia famous journals Fibrous dysplasia Google Scholar indexed journals chronic suppurative otitis media articles chronic suppurative otitis media Research articles chronic suppurative otitis media review articles chronic suppurative otitis media PubMed articles chronic suppurative otitis media PubMed Central articles chronic suppurative otitis media 2023 articles chronic suppurative otitis media 2024 articles chronic suppurative otitis media Scopus articles chronic suppurative otitis media impact factor journals chronic suppurative otitis media Scopus journals chronic suppurative otitis media PubMed journals chronic suppurative otitis media medical journals chronic suppurative otitis media free journals chronic suppurative otitis media best journals chronic suppurative otitis media top journals chronic suppurative otitis media free medical journals chronic suppurative otitis media famous journals chronic suppurative otitis media Google Scholar indexed journals Temporal bone articles Temporal bone Research articles Temporal bone review articles Temporal bone PubMed articles Temporal bone PubMed Central articles Temporal bone 2023 articles Temporal bone 2024 articles Temporal bone Scopus articles Temporal bone impact factor journals Temporal bone Scopus journals Temporal bone PubMed journals Temporal bone medical journals Temporal bone free journals Temporal bone best journals Temporal bone top journals Temporal bone free medical journals Temporal bone famous journals Temporal bone Google Scholar indexed journals Imaging articles Imaging Research articles Imaging review articles Imaging PubMed articles Imaging PubMed Central articles Imaging 2023 articles Imaging 2024 articles Imaging Scopus articles Imaging impact factor journals Imaging Scopus journals Imaging PubMed journals Imaging medical journals Imaging free journals Imaging best journals Imaging top journals Imaging free medical journals Imaging famous journals Imaging Google Scholar indexed journals CT articles CT Research articles CT review articles CT PubMed articles CT PubMed Central articles CT 2023 articles CT 2024 articles CT Scopus articles CT impact factor journals CT Scopus journals CT PubMed journals CT medical journals CT free journals CT best journals CT top journals CT free medical journals CT famous journals CT Google Scholar indexed journals X-ray articles X-ray Research articles X-ray review articles X-ray PubMed articles X-ray PubMed Central articles X-ray 2023 articles X-ray 2024 articles X-ray Scopus articles X-ray impact factor journals X-ray Scopus journals X-ray PubMed journals X-ray medical journals X-ray free journals X-ray best journals X-ray top journals X-ray free medical journals X-ray famous journals X-ray Google Scholar indexed journals fibrous dysplasia articles fibrous dysplasia Research articles fibrous dysplasia review articles fibrous dysplasia PubMed articles fibrous dysplasia PubMed Central articles fibrous dysplasia 2023 articles fibrous dysplasia 2024 articles fibrous dysplasia Scopus articles fibrous dysplasia impact factor journals fibrous dysplasia Scopus journals fibrous dysplasia PubMed journals fibrous dysplasia medical journals fibrous dysplasia free journals fibrous dysplasia best journals fibrous dysplasia top journals fibrous dysplasia free medical journals fibrous dysplasia famous journals fibrous dysplasia Google Scholar indexed journals HRCT articles HRCT Research articles HRCT review articles HRCT PubMed articles HRCT PubMed Central articles HRCT 2023 articles HRCT 2024 articles HRCT Scopus articles HRCT impact factor journals HRCT Scopus journals HRCT PubMed journals HRCT medical journals HRCT free journals HRCT best journals HRCT top journals HRCT free medical journals HRCT famous journals HRCT Google Scholar indexed journals Pneumosinus Dilatans Frontalis articles Pneumosinus Dilatans Frontalis Research articles Pneumosinus Dilatans Frontalis review articles Pneumosinus Dilatans Frontalis PubMed articles Pneumosinus Dilatans Frontalis PubMed Central articles Pneumosinus Dilatans Frontalis 2023 articles Pneumosinus Dilatans Frontalis 2024 articles Pneumosinus Dilatans Frontalis Scopus articles Pneumosinus Dilatans Frontalis impact factor journals Pneumosinus Dilatans Frontalis Scopus journals Pneumosinus Dilatans Frontalis PubMed journals Pneumosinus Dilatans Frontalis medical journals Pneumosinus Dilatans Frontalis free journals Pneumosinus Dilatans Frontalis best journals Pneumosinus Dilatans Frontalis top journals Pneumosinus Dilatans Frontalis free medical journals Pneumosinus Dilatans Frontalis famous journals Pneumosinus Dilatans Frontalis Google Scholar indexed journals
Article Details
1. Introduction
Pneumosinus dilatans is a rare condition of abnormal dilatation of the paranasal sinuses characterized by the hyperpneumatisation of a single or multiple paranasal sinuses. The condition was originally described by Meyes in 1898 followed by refinement of the entity later by Benjamins and Urken et al [1-3]. This nomenclature is typically reserved for a sinus that is abnormally expanded beyond its normal boundaries with an intact wall and normal wall thickness. This is in contrast to pneumatocoele, which is an expansion of a sinus associated with thinned sinus wall. A typical pneumosinus dilatans is radiologically an abnormal dilation of one or more paranasal sinuses without any features of localized bone destruction, associated hyperostosis, or thickening of the mucous membrane [4]. Rarely along with generalized invol-vement of paranasal sinuses, there is associated dilation of mastoid air cells and is termed as pneumosinus dilatans multiplex [5]. The etiology of the condition is contested and the proposed mechanism include obstruction of the sinus by a mass, the presence of gas-forming microorganisms, spontaneous drainage of a mucocele, the presence of a one-way valve, abnormalities of hormonal regulation leading to a disturbance of osteoblastic and osteoclastic activity [4, 5].
Fibrous dysplasia is part of a spectrum of anomalies termed fibro-osseous lesions, a diverse group of processes that are characterized by the replacement of normal bone by a fibrous tissue containing a newly formed mineralized product. Apart from the more important fibrous dysplasia (FD), the group includes cemento-osseous dysplasia and ossifying fibroma. Fibrous dysplasia is a non-hereditary, developmental tumor-like condition in which the normal trabecular bone is replaced by cellular fibrous connective tissue proliferation intermixed with irregular trabeculae [6, 7]. In general, three major patterns of fibrous dysplasia are described namely monostotic, polyostotic and craniofacial form. About 3% of patients are associated with McCune–Albright syndrome featuring skin pigmentation and hyper-functioning endocrine disorders [7, 8].
2. Clinical Observations and Imaging Findings
A 32-year-old man was admitted to the emergency following an episode of seizure. An emergency CT head was performed which showed areas of bilateral frontal lobe gliosis and changes of left front parietal craniectomy. He also had a sclerosing disease of the skull involving the left frontal, temporal, zygomatic bones, and a part of the left parietal bone. There were also patchy areas of involvement in the right frontal, temporal and parietal bones. Associated bone disease in the form of fibrous dysplasia was thought of and a detailed clinical assessment was made after his recovery from seizure and postictal confusion.
The patient was suffering from epilepsy since infancy and was on medication. He was found to have a bony disease of the calvarium when he was15 years old, after a CT examination. As the expansile bony lesion was found to cause compression of the left frontal lobe, a wide excision craniectomy was done to remove the bony lesion. The resection biopsy proved fibrous dysplasia.
Current CT shows a craniectomy defect with the margins showing irregular sclerosis and calvarial thickening indicating recurrent disease. There is bilateral frontal lobe gliosis on CT scan and MRI, which may be attributed to sequelae of the previous compression by the expansile bony lesion and with a possible contribution from surgery (Figure 1). The patient’s seizures are now occasional, about once in 6 months to 5 years. He is on a maintenance dose of antiepileptic.
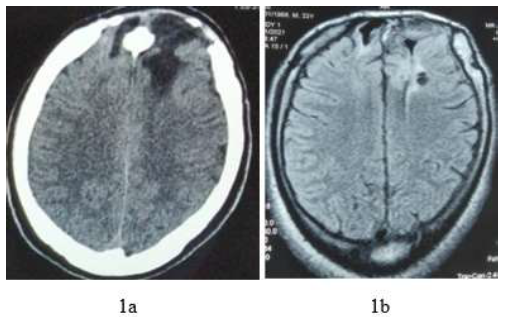
Figure 1: 1a. Axial CT at a high level shows bifrontal hypodense areas, indicating gliosis. Note the central nodular bone density and changes of craniectomy; 1b. Axial FLAIR images showing gliosis and expanded left frontal bone with high signal than the corresponding normal area on the right side indicating residual lesions of fibrous dysplasia.
Another complaint is a progressive bulging hard swelling of the left frontal region with minor disturbance to the visual field. X-ray skull reveals unusually large paranasal sinuses (Figure 2). CT images show that much of the frontal bossing is due to an unusually large left frontal sinus which is protruding to create the frontal bulge (Figure 3). There is an irregular lobulated thickening of the left frontal sinus wall with a sclerotic or ground glass haze indicating involvement by fibrous dysplasia. Maxillary, ethmoid, and sphenoid sinuses are relati-vely larger than normal. The right frontal sinus is normal in size. The left frontal sinus is grossly enlarged with a tortuous cavity extending higher up and posteriorly with many intervening bony septae (Figure 4). It is expanding the ethmoid and left sphenoid bone areas crossing the midline at places reaching as far posteriorly to cause a bulge into the left anterior temporal fossa. This unusual dilation of the left frontal sinus can be described as a complex pneumosinus dilatans frontalis. The ostium of the left frontal sinus appears patent on CT, though narrowed by expanded ethmoid and maxillary sinuses. There is no bony involvement of maxillary or ethmoid sinuses by fibrous dysplasia. There is irregular polypoid-nodular wall thickening of the left frontal bone with outer and inner cortical projections showing sclerosis with central areas of high density or ground glass haze. This is causing compression of the left frontal lobe and mild asymmetry of intracranial structures (Figures 5, 6). No evidence of any extracranial involvement or skin involvement was evident on history and physical examination to diagnose McCune-Albright syndrome. The visual acuity is normal. He has moderate-severe conductive hearing loss of the left ear on audiometry.
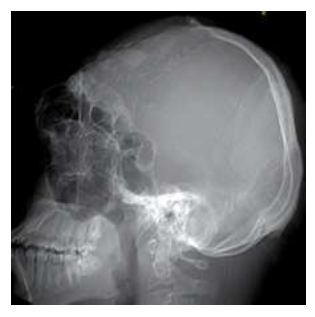
Figure 2: Lateral X-ray of skull showing unusually expanded paranasal sinuses-Pneumosinus dilatans.
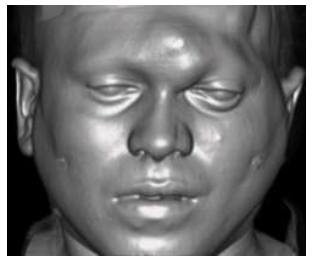
Figure 3: Surface rendered CT images showing a large bulge in the left frontal area which is extending to the left orbital area.
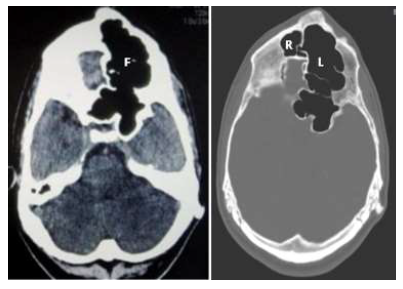
Figure 4: 4a. Axial CT at mastoid level showing grossly dilated left frontal sinus (F) encroaching the left middle cranial fossa; 4b. Axial CT bone window images showing the grossly dilated left frontal sinus (L) with multiple bony septations indicating pneumosinus dilatans. Compare this with a near-normal size of the right frontal sinus (R).
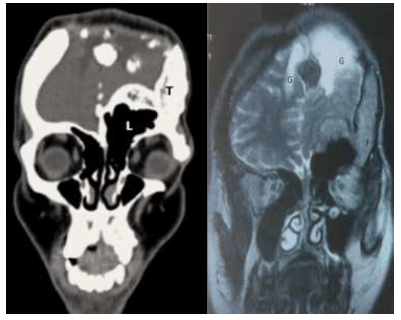
Figure 5: 5a. Coronal CT sections showing dilated left frontal sinus (L) compared to the right side. Left side frontal, temporal and zygomatic bones are expanded with lobulated outline (T); 5b.Coronal T2 MR image showing the sinus changes and the expanded left side bone matrix with a heterogeneous hyperintense signal (F) indicating fibrous dysplasia. Areas of frontal lobe gliosis (G) are also evident.
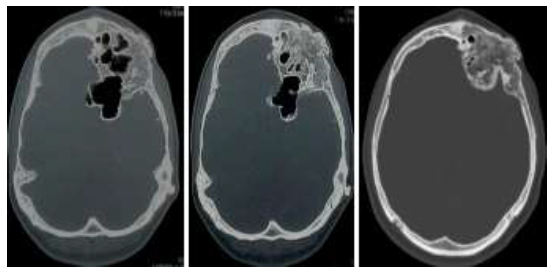
Figure 6: 6a. Axial CT sections showing dilated left frontal sinus surrounded by an expanded left frontal bone; 6b, 6c. Sections higher up showing the expanded diploic space and lobulated cortical margins. The margins are sclerosed with a relatively ground glass density matrix indicating the sclerosing phase of fibrous dysplasia.
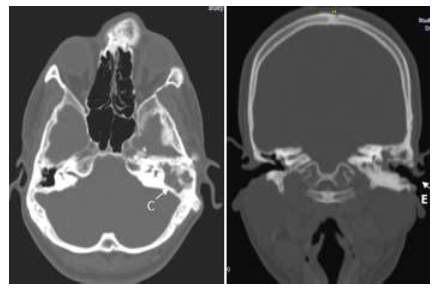
Figure 7: 7a. Axial CT sections showing soft tissue density filling the left mastoid antrum and air cells (C) indicating otitis media; 7b. Coronal CT image shows a sclerosed left temporal bone including the mastoid with a homogenous matrix of fibrous dysplasia. The left external auditory canal (E) is irregular. Soft tissue density noted in the left middle ear cavity and mastoid air cells indicating CSOM.
He was suffering from recurrent left ear pain and ear discharge indicating chronic suppurative otitis media (CSOM). He underwent resection of fibrous dysplasia of the left external auditory canal about 5 years back. Current CT and MRI show diffuse involvement of left temporal bone with thickening, widening of diploic space, and lobulated appearance of outer cortex mimicking exostosis at places. His left external ear canal is roomy with nodular granulation tissue on physical examination. CT shows soft tissue density filling the left middle ear cavity and mastoid indicating cholesteatoma or granulation tissue.
There is diffuse sclerotic involvement of left petrous temporal bone involving the mastoid, walls of the external ear canal, and the mandibular cavity of the temporal bone on CT scan (Figure 7). The left Eustachian tube is narrowed. The left internal ear structures, middle ear ossicles, and the internal auditory canal are intact.
3. Discussion
3.1 Pneumosinus dilatans
Pneumosinus dilatans is a rare condition with just more than 100 cases reported to date. A meta-analysis in early 2021 counted a total of 145 patients from 103 articles [9] and an earlier article in 2013 reviewed 123 cases [10]. It is slightly more common among males (57%) with an average age of 32 years at presentation. It commonly involves the frontal sinus (62%), followed by sphenoid sinus (24%), maxillary sinus (20%), and rarely (19%) the ethmoid sinus [9, 10]. Commonly it affects a single sinus (81.5%) than multiple sinuses. Rarely all the sinuses and both mastoid air cells are involved and such cases are labeled as pneumosinus dilatans multiplex, with only three reported cases noted in our review [11, 12, 13]. About 50% of cases are associated with another condition, which is commonly an ethmoid sinus disease (81.5%) than frontal sinus (29.7%) involvement [9]. About 25% of symptomatic frontal pneumosinus dilatans is associated with an intracranial pathology like meningioma, arachnoid cyst, or orbital tumor [10].
3.2 Aetiopathology of frontal pneumosinus dilatans
Several theories on the etiology of pneumosinus dilatans are proposed, but not substantiated with reliable scientific evidence. The aetiology of the condition remains obscure even after 100 years of describing this entity [14]. Only a small number (about 19) of articles offer some form of evidence of aetiology. A "ball-valve" mechanism of sinus outflow obstruction causing air trapping is the most substantiated of the proposed aetiologies. Another is a primary fibro-osseous pathologic process with potential to disrupt the cellular milieu. A proposal like hormonal dysregulation or a spontaneously draining mucocele is even less substantiated. Causation by gas-forming bacteria was proposed but without adequate evidence. Epidemiological evidence of a bimodal distribution of disease occurrence in a younger population (16-25 years) and an older population (36-40 years) may indicate possible multiple etiologies [12, 14]. Commonly reported symptoms of pneumosinus dilatans are facial deformities (39%), headache (24%), or visual loss (15%). Uncommon visual disturbances include diplopia, reduced visual acuity which is frequent with sphenoid sinus involvement. The presence of pneumosinus dilatans may be a sign of underlying disease or help in unmasking significant clinical findings like meningomyelocoele in some cases [9, 15]. Large pneumosinus dilatans can cause pressure effects like neurological deficits, cranial nerve palsies, and exophthalmos [16]. There is a wide difference in the size of the frontal sinus in the general population [17] and many cases of pneumosinus dilatans are associated with a many-fold expansion of the sinus. At birth, frontal sinuses are absent or rudimentary. Pneumatisation starts at 4 years and becomes well-formed by 7-8 years to reach the full size by puberty. Pneumatisation may continue even after forty years. The average estimated size of a frontal sinus in an adult is 3.3cm height, 2.6cm width, and 1.8cm length [18, 19]. Sinus expansion is often an ongoing process and is possibly due to a progressive increase in the sinus pressure as a result of a one-way ball valve mechanism allowing entering but not exiting of air at the level of the frontal sinus ostium. Drastic pressure changes occurring during the Valsalva maneuver or forced sneezing are possibly another mechanism for sinus expansion. Sinus overgrowth also occurs in acromegaly, influenced by general growth factor or due to compensatory expansion as in cases of cerebral agenesis. Other pathological entities like fibro-osseous diseases are probable causes. Normal development of frontal sinus may be modified by fractures, severe infections, or neoplasm. Frontal sinus expansion presents with changes of facial contour, headache, facial pain, or visual disturbances [19-22].
Having found a relatively uninvolved patent frontal sinus ostium and uninvolved osteomeatal complex and robust involvement of the left frontal bone, the possible aetiology in the index case appears to be due to a disruption of the cellular milieu leading to sinus expansion secondary to bony involvement with fibrous dysplasia. There are reports on the association of meningioma with pneumosinus dilatans, with the tumor tending to affect the trophic milieu of the adjacent bone [23, 24]. Fibrous dysplasia is a rare association of pneumosinus dilatans with occasional case reports [24, 25].
3.3 Fibrous dysplasia
Fibrous dysplasia was first described by Lichtenstein and Jaffe in 1942 and is sometimes called as Lichtenstein-Jaffe disease. It is a developmental non-inherited anomaly of bone where the normal bone marrow is replaced by a fibro-osseous tissue. Commonly, it is a disease of a single bone (monostotic fibrous dysplasia) in 75-80% of cases, but in 20-25% of cases, it is polyostotic, involving more than one bone [6, 26]. The exact incidence of fibrous dysplasia is uncertain as the disease is often asymptomatic and many cases are detected incidentally. Roughly, it accounts for about 5% of benign bone lesions [27]. It is a slow-growing lesion that clinically presents during the age of bone growth and is thus commonly noticed in early teenage and adolescent years. Polyostotic fibrous dysplasia usually presents earlier, an average of 8 years. Polyostotic fibrous dysplasia rarely occurs as part of syndromes like McCune-Albright syndrome or Mazabraud syndrome.
Monostotic fibrous dysplasia commonly involves ribs, proximal femur, or craniofacial bones which typically involves the posterior maxilla. The lesion may involve a small area of bone or occupy the entire bone. Polyostotic fibrous dysplasia involvement varies from just two bones to more than 75% of the entire skeleton. The most common locations of this form of the disease are femur, tibia, pelvis, and foot bones. Less commonly affected sites include ribs, skull bones, upper extremity, lumbar spine, cervical spine, and clavicle [28, 29]. Limb deformities, pain, pathological fracture, facial asymmetry due to cranial involvement are common presentations. Symptomatic involvement is more common (75%) in polyostotic disease [30, 31].
Many cases of fibrous dysplasia are stabilised at bone maturity, but the deformity caused by it may progress. About 0.9-4% of fibrous dysplasia can undergo an aggressive form which often occurs more than 20 years of onset. It is more common in the polyostotic form [6, 32]. Malignant transformation of fibrous dysplasia occurs in about 0.4 to 4% as per different literature. It is more common in polyostotic form and is frequently (39%) associated with previous irradiation, cautioning against undue radiation exposure. The craniofacial region is the most common site of malignant transformation followed by femur, tibia, and pelvis [6, 33].
There is no tendency for the monostotic form to convert to the polyostotic form. A high rate of recurrence of fibrous dysplasia is seen after curettage and bone grafting. The majority of the lesions stabilize by skeletal maturity. But the deformity caused by the disease may persist or worsen [34] as in the index case. The bone lesions appear sclerotic and quiescent in the current imaging of our index case compared to the cystic nature before. However, the pneumosinus dilatans appear progressive with increasing bossing of the left frontal region. Apart from the cosmetic problems and mass effect, pneumosinus dilatans can cause erosion of the sinus resulting in pneumocephalus, and can rarely become severe enough to cause tension pneumocephalus [35]. The index patient underwent excision of the left external auditory canal wall. But sclerosis and thickening of the left temporal bone are causing narrowing of the Eustachian tube with a soft tissue density of the middle ear cavity and mastoid air cells, which might be caused by cholesteatoma or chronic granulation tissue. The patient continued to have left ear pain and discharge which occasionally get worse. Surprisingly the persistent gliosis of both frontal lobes is not causing any notable neurological deficit, although the patient rarely experiences seizure which is under control compared to early childhood. Because of the complexity of the disease, the patient chose to be on conservative management and is able to perform his routine occupational activities. As of now, there is no effective medication for fibrous dysplasia with a capacity to change the course of the disease. Bisphosphonates may be helpful for related bone pain. Surgical interventions are reserved for addressing specific issues than as a main treatment option [6].
3.4 Temporal bone involvement in fibrous dysplasia
Temporal bone involvement in fibrous dysplasia is frequent in craniofacial disease. Most cases occur around the external auditory canal causing stenosis. Frequent clinical complaints include headache, otalgia, otorrhea, temporal region mass, or trismus. Most affected patients (about 80% in some series) have a varying degree of stenosis of the external auditory canal leading to conductive hearing loss. Cholesteatoma is frequent in such patients causing destruction of the middle and inner ear. Facial nerve involvement can lead to facial nerve palsy [36]. Polyostotic lesions affecting temporal bones are rarely reported and bilateral temporal bone involvement is unusual [37]. In a large review, hearing loss from fibrous dysplasia was found commonly due to crowding of the ossicular chain and elongation of the internal auditory canal [38]. External ear canal stenosis and otic capsule invasion were less often encountered causes. CT imaging with multiplanar reconstruction and HRCT is the optimal imaging modality to study craniofacial involvement [39, 40] and the easy way to assess disease burden.
4. Conclusion
Advanced craniofacial fibrous dysplasia may have multiple complications such as hearing loss, chronic otitis media, pneumosinus dilatans, and neurological complications. A comprehensive multimodality approach may be needed in managing such cases. CT scan is highly valuable in assessing the cranial involvement of fibrous dysplasia.
Authors’ Contributions
Sabujan Sainudeen: I am the author of the article and was involved in imaging at the time of this patient’s admission. I followed up with the patient and was present at the CT and MRI examination, taking the clinical history and examining the patient.
Asmi M: She contributed to the diagnosis, research, and manuscript preparation.
Methil Pradeep: Is a consultant neurologist who was treating and following the patient for the last ten years. He supervised the work.
Declaration of Competing Interest
The authors declare that we have no conflict of interest.
Ethical Statement
Written informed consent was obtained from the patient.
All identifying information has been removed and CT images were entirely anonymized.
References
- Alatar AA, Al Suliman YA, Alrajhi MS, et al. Maxillary pneumosinus dilatans presenting with proptosis: A case report and review of the literature, Clinical Medicine Insights: Ear, Nose and Throat. January (2019).
- Meyes J. Pneumosinus dilatans. Nederlands Tijdschr Geneeskd 11 (1898): 143-148.
- Urken ML, Som PM, Lawson W, Edelstein D, Weber AL, Biller HF, Abnormally large frontal sinus. II. Nomenclature, pathology, and symptoms. Laryngoscope. 97 (1987) 606–611.
- Teh BM, Hall C, Chan SW. Pneumosinus dilatans, pneumocoele or air cyst? A case report and literature review. The Journal of laryngology and otology 126 (2012): 88-93.
- Ushas P, Ravi V, Painatt JM, et al. Pneumosinus dilatans multiplex associated with hormonal imbalance. Case Reports (2013): bcr2013010345.
- Kushchayeva YS, Kushchayev SV, Glushko TY, et al. Fibrous dysplasia for radiologists: beyond ground glass bone matrix. Insights Imaging 9 (2018): 1035-1056.
- Javaid MK, Boyce A, Appelman-Dijkstra N, et al. Best practice management guidelines for fibrous dysplasia/McCune-Albright syndrome: a consensus statement from the FD/MAS international consortium. Orphanet J Rare Dis 14 (2019): 139.
- McCarthy EF. Fibro-osseous lesions of the maxillofacial bones. Head Neck Pathol 7 (2013): 5-10.
- Ricci, Joseph A, Pneumosinus Dilatans, Journal of Craniofacial Surgery: January 07 (2021).
- Desai Naman S, Saboo Sachin S, Khandelwal Ashish, et al. Pneumosinus dilatans: Is it more than an aesthetic concern?, Journal of Craniofacial Surgery 25 (2014): 418-421.
- Kiroglu Y, Karabulut N, Sabir NA, et al. Pneumosinus dilatans and multiplex: report of three rare cases and review of the literature. Dento Maxillo Facial Radiology 36 (2007): 298-303.
- Ushas P, Ravi V, Painatt JM, et al. Pneumosinus dilatans multiplex associated with hormonal imbalance. Case Reports (2013): bcr2013010345.
- Hwang Kun, Lee Dae Kwang, Lee Choong Jae, et al. Pneumosinus dilatans multiplex, mental retardation, and facial deformity. Journal Of Craniofacial Surgery 11 (2000): 487-490.
- Ricci JA. Pneumosinus Dilatans: Over 100 years without an etiology. J Oral Maxillofac Surg 75 (2017): 1519-1526.
- Kiroglu Y, Karabulut N, Sabir NA, et al. Pneumosinus dilatans and multiplex: report of three rare cases and review of the literature. Dento Maxillo Facial Radiology 36 (2007): 298-303.
- Rebeca Rosés Sáiz, Elsa Font Julià, Félix García Ortega, et al. Progressive proptosis secondary to pneumosinus dilatans of the ethmoidal sinus in a pediatric patient,Orbit (2020).
- Rubira-Bullen IRF, Rubira CMF, Sarmento VA, et al. Frontal sinus size on facial plain radiographs. J Morphol Sci 27 (2010): 77-81.
- Gray’s Anatomy. Fortieth Edition (2008): 556-557.
- Kalpana Purohit, Ankita Purohit, Ramesh Palanisamy. Pneumosinus Dilatans: A cadaveric case report. Int J Med Res Prof 2 (2016): 89-91.
- Adams WM, Jones RI, Chavda SI, et al. Pneumosinus dilatans: a discussion of four cases and the possible aetiology. Rhinology 36 (1998): 40-42.
- Schrijver HM, Berendse HW. Pneumoncephalus by Valsalva’s maneuver. Neurology 60 (2003): 345-346.
- Weiglein A, Anderhuber W, Wolf G. Radiologic anatomy of the paranasal sinuses in the child. Surg Radiol Anat 14 (1992): 335-339.
- Miller NR, Golnik KC, Zeidman SM, et al. Pneumosinus dilatans: a sign of intracranial meningioma. Surg Neurol 46 (1996): 471-474.
- Sweatman J, Beltechi R. Pneumosinus Dilatans: An exploration into the association between arachnoid cyst, meningioma and the pathogenesis of pneumosinus dilatans. Clin Neurol Neurosurg 185 (2019): 105462.
- Lucas L Walgrave, Benjamin Peersman, Rik Verhille, et al. Pneumosinus dilatans associated with fibrous dysplasia (2019).
- Riminucci M, Saggio I, Robey PG, et al. Fibrous dysplasia as a stem cell disease. J Bone Miner Res. Suppl 2 (2006): 125-131.
- Rahman AM, Madge SN, Billing K, et al. Craniofacial fibrous dysplasia: clinical characteristics and long-term outcomes. Eye (Lond) 23 (2009): 2175-2181.
- Parekh SG, Donthineni-Rao R, Ricchetti E, et al. Fibrous dysplasia. J Am Acad Orthop Surg 12 (2004): 305-313.
- Lietman SA, Schwindinger WF, Levine MA. Genetic and molecular aspects of McCune-Albright syndrome. Pediatr Endocrinol Rev. Suppl 4 (2007): 380-385.
- Tabareau-Delalande F, Collin C, Gomez-Brouchet A, et al. Diagnostic value of investigating GNAS mutations in fibro-osseous lesions: a retrospective study of 91 cases of fibrous dysplasia and 40 other fibro-osseous lesions. Mod Pathol 26 (2013): 911-921.
- Shah ZK, Peh WC, Koh WL, et al. Magnetic resonance imaging appearances of fibrous dysplasia. Br J Radiol 78 (2005): 1104-1115.
- Kaushik S, Smoker WR, Frable WJ. Malignant transformation of fibrous dysplasia into chondroblastic osteosarcoma. Skeletal Radiol 31 (2002): 103-106.
- Ruggieri P, Sim FH, Bond JR. Malignancies in fibrous dysplasia. Cancer 73 (1994): 411-1424.
- Kahn MA, Lucca M, Papageorge MB. A clinico-pathologic correlation: fibrous dysplasia. J Mass Dent Soc 54 (2006): 48-50.
- Scholsem, Martin Collignon, Frederic, et al. Spontaneous pneumocephalus caused by the association of pneumosinus dilatans and meningioma-Case illustration. Journal of neurosurgery 105 (2006): 934.
- Liu YH, Chang KP. Fibrous dysplasia of the temporal bone with external auditory canal stenosis and secondary cholesteatoma. J Int Adv Otol 12 (2016): 125-128.
- Megerian CA, Sofferman RA, McKenna MJ, et al. Fibrous dysplasia of the temporal bone: Ten new cases demonstrating the spectrum of otologic sequelae. Am J Otol 164 (1995): 408-419.
- Papadakis CE, Skoulakis CE, Prokopalis EP, et al. Fibrous dysplasia of the temporal bone: report of a case and a review of its characteristics. Ear Nose Throat J 79 (2000) 52.
- Boyce AM, Brewer C, De Klotz TR, et al. Association of Hearing Loss and Otologic Outcomes With Fibrous Dysplasia. JAMA Otolaryngol Head Neck Surg 144 (2018): 102-107.
- Mazziotti S, Blandino A, Gaeta M, et al. Post processing in Maxillofacial Multidetector Computed Tomography. Cana Asso of Radio Journal 66 (2015): 212-222.
