Communication in the Time of Coronavirus: Three Tips for Enhancing Communication with Families in the Intensive Care Unit that are here to stay
Article Information
Kashika G Goyal MD1*, Tyler Trahan MD2, Margaret M Hayes MD3,4
1Division of Pulmonary, Critical Care & Sleep Medicine, Ohio State University, Columbus, Ohio, USA
2Department of Medicine, Henry Ford Health System, Detroit, Michigan, USA
3Division of Pulmonary, Critical Care & Sleep Medicine, Beth Israel Deaconess Medical Center, Boston, Massachusetts, USA
4Carl J Shapiro Institute for Education and Research, Beth Israel Deaconess Medical Center, Boston Massachusetts, USA
*Corresponding Author: Kashika G Goyal, Division of Pulmonary, Critical Care & Sleep Medicine, Ohio State University, Columbus, Ohio, USA
Received: 19 November 2021; Accepted: 25 November 2021; Published: 12 January 2022
Citation: Kashika G Goyal, Tyler Trahan, Margaret M Hayes. Communication in the Time of Coronavirus: Three Tips For Enhancing Communication with Families in the Intensive Care Unit that are here to stay. Anesthesia and Critical Care 4 (2022): 8-13.
Share at FacebookAbstract
Coronavirus disease 19 (COVID19) has forced the rapid evolution of ICU care including re-evaluation of ICU triage, resource utilization, staffing models and in the most stark manner end of life care. Family members, usually present on rounds and in waiting rooms, are suddenly absent, making family meetings nearly impossible and critical decisions challenging. It would be not only understandable, but also expected if communication broke down during this time. Across countries and hospital systems, the importance of communication and the need for end of life care when required has become paramount. However, translating that to direct patient care can remain nebulous. We present three tangible strategies, implemented during the COVID-19 pandemic to enhance communication in the ICU, that have now become routine in our ICUs. Those strategies include making family updates a daily occurrence and integrated into the workflow of ICU rounds, documenting these conversations in the medical record, and the expansive use of technology and telehealth to further bridge the physical gap that now exists between family members and ICU teams. These strategies are straight forward and pragmatic but if implemented can change care patterns both in a positive and lasting way.
Keywords
ICU, End of life, Communication, COVID-19
ICU articles; End of life articles; Communication articles; COVID-19 articles
ICU articles ICU Research articles ICU review articles ICU PubMed articles ICU PubMed Central articles ICU 2023 articles ICU 2024 articles ICU Scopus articles ICU impact factor journals ICU Scopus journals ICU PubMed journals ICU medical journals ICU free journals ICU best journals ICU top journals ICU free medical journals ICU famous journals ICU Google Scholar indexed journals End of life articles End of life Research articles End of life review articles End of life PubMed articles End of life PubMed Central articles End of life 2023 articles End of life 2024 articles End of life Scopus articles End of life impact factor journals End of life Scopus journals End of life PubMed journals End of life medical journals End of life free journals End of life best journals End of life top journals End of life free medical journals End of life famous journals End of life Google Scholar indexed journals Communication articles Communication Research articles Communication review articles Communication PubMed articles Communication PubMed Central articles Communication 2023 articles Communication 2024 articles Communication Scopus articles Communication impact factor journals Communication Scopus journals Communication PubMed journals Communication medical journals Communication free journals Communication best journals Communication top journals Communication free medical journals Communication famous journals Communication Google Scholar indexed journals COVID-19 articles COVID-19 Research articles COVID-19 review articles COVID-19 PubMed articles COVID-19 PubMed Central articles COVID-19 2023 articles COVID-19 2024 articles COVID-19 Scopus articles COVID-19 impact factor journals COVID-19 Scopus journals COVID-19 PubMed journals COVID-19 medical journals COVID-19 free journals COVID-19 best journals COVID-19 top journals COVID-19 free medical journals COVID-19 famous journals COVID-19 Google Scholar indexed journals quality of life articles quality of life Research articles quality of life review articles quality of life PubMed articles quality of life PubMed Central articles quality of life 2023 articles quality of life 2024 articles quality of life Scopus articles quality of life impact factor journals quality of life Scopus journals quality of life PubMed journals quality of life medical journals quality of life free journals quality of life best journals quality of life top journals quality of life free medical journals quality of life famous journals quality of life Google Scholar indexed journals
Article Details
Abbreviations:
ICU (intensive care unit)
Communication in the time of Coronavirus: Three tips for enhancing communication with families in the Intensive Care Unit
The Intensive Care Unit (ICU) is a high acuity environment where communication is instrumental to patient care. Because critically ill patients are often unable to make medical decisions for them, communication frequently occurs between clinicians and family members. Communication is most needed around end of life issues and when done well, effective communication about end-of-life care is associated with decreased intensity of care, increased quality of life, and improved quality of dying [1]. Coronavirus disease 19 (COVID19) has forced the rapid evolution of ICU care including re-evaluation of ICU triage, resource utilization, staffing models and in the most stark manner end of life care [2]. Hospitals were forced to initially prohibit, and now restrict visitors to limit exposure to COVID-19 and help prevent the spread. Family members, usually present on rounds and in waiting rooms, are suddenly absent, making family meetings difficult and critical decisions challenging. It would be not only understandable, but also expected if communication broke down during this time. Instead though, the height of the pandemic accelerated a necessary evolution in our communication strategies. Across countries and hospital systems, recommendations have been published that highlight the importance of realistic goals of care, the importance of communication and the need for end of life care when required [3]. However, translating that to direct patient care can remain nebulous. Herein we present three tangible strategies, implemented during the COVID-19 pandemic to enhance communication in the ICU, that have now become routine in our ICUs.
Making family updates a daily “to-do.”
Families often rate the communication between them and ICU physicians as inadequate. It is easy for families and patient to feel excluded from their own care, left in a metaphorical waiting room. Without the convenience of in-person conversations and families present on rounds in the COVID era, we witnessed essential changes in response. Family communication became a critical task for the day. At our institution, resident physicians use an electronic to-do list (a team census) that allows team members to leave unofficial updates and keep track of tasks for day. Once the COVID-19 pandemic occurred, updating families became a daily “to-do” on this list and these updates became engrained in the workflow. Family updates had always been a goal, but the pandemic makes it a necessity. Further, family updates have since become formally embedded into our multidisciplinary rounds, ensuring this is reviewed as a core measure of quality care, similar to ensuring proper venous thromboembolism prophylaxis and documented code status. Throughout the pandemic, we noted that frequent clinical updates facilitated an alliance between families and the care team, which allowed for easier conversations at critical turning points in the patient’s clinical course. Despite the increase in physical distance between physicians and family members, a space has opened for increased dialogue and ironically physician visibility.
Documenting goals of care conversations in the medical record
The frequent updates we witnessed were also accompanied by an increase in the practice of documenting both content and tone of these conversations in the electronic medical record. Handoffs are a vulnerable time when it comes to creating a shared understanding of the patient’s clinical course and individual goals. Providers may be hyperfocused on raw clinical data, forgetting to pass off goals of care conversations. COVID-19 patients decompensate quickly and are often transferred from the floor to the ICU- further transitions of care occur when surge spaces are open and closed. The number of handoffs increases dramatically, as does the inherent variability in care team members, potentiating situations of perpetuated misunderstandings. Inconsistent messages erode patient-physician trust as 1 in 4 family members of patients surviving to discharge from ICU stays felt they received inconsistent information, noting that these mixed messages make decision making difficult [4]. The practice of documenting conversations with family members lays the groundwork for a new layer of continuity, so all team members can be on the same page with family members, recognizing that this page does change frequently. Within our own institution we observed increased frequency of documentation but there continues to be variability in what is included in communication notes. We suggest a template that includes documenting the members of the team who participated in the conversation, family members involved, the medical update provided and any elements of the conversation that pertain to goals of care (figure 1). Additionally we recommend documenting the timeline for the next update.
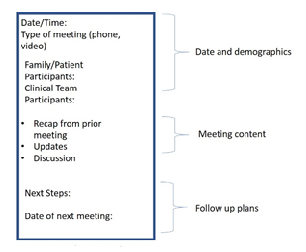
Figure 1: Sample communication note template.
Visiting virtually
For critically ill patients communication between patients and families is paramount as physicians seek ways to alleviate the distress and fear of being alone. The tumult of a pandemic removes control as families are physically separated from their loved ones. To close this gap we saw the rise of telehealth communication. Early studies have suggested that physicians and families find remote communication satisfactory in some contexts, though the need to develop remote communication skills to improve experience remains [5]. Our hospital instituted the use of tablet devices collected through a donation program to facilitate virtual visits and updates.In addition to virtual visits enabling companionship and support, we also utilize video conferencing with these tablets to hold family meetings. During the beginning of the pandemic, these were typically done over the phone, but as donations of tablets increased, we are now able to dedicate devices specifically for family meetings. We implemented the use of HIPAA compliant programs such as the Starleaf™ application to facilitate this communication. In our experience, meetings held via video conference are superior to those conducted over the phone, as they enable participants to see faces, read expressions, and understand emotion. Prior studies have attempted to implement protocols for the frequency of family meetings- despite this protocol family meetings occurred on average twice over the course of 17 days [6]. Virtual family meetings transcend barriers of schedules and physical limitations of gathering in small conference rooms, and at our institution have led to more frequent family meetings. As a tertiary care center our patients are frequently transferred from hours away, by incorporating virtual visits we have increased the convenience of family meetings, an adaptation that will persist beyond the pandemic. This change in communication does come with caution as the use of telehealth and technology has the risk of perpetuating technology-driven health care disparities, although flexibility in platforms used (ie integration of Face Time and Skype) may help balance this [7].
Lasting Changes
Visitors have slowly trickled back into the ICU at our institution, but the pandemic is far from over. We believe that these communication changes have changed our communication for the better. We continue to seek out families daily. These conversations are now ever-present in the medical record- another point of continuity when the complexity of someone’s clinical course means multiple teams and transfers of care. For our ICU and care teams, these changes, born from isolation and uncertainty, remain a bridge between the ICU and the family members at its core. The coronavirus pandemic, which we hope is a finite moment in medical history, has provided the impetus for lasting change in the structure of communication within the ICU.
Declarations
Ethics approval
Not applicable
Consent for publication
Not applicable
Availability of data and materials
Not applicable
Competing interests
The authors declare that they have no competing interests
Funding
Not applicable
Author’s contributions
K.G. and M. H conceived of the main conceptual ideas of this manuscript. All authors contributed to the exploration of these ideas and to the writing of the manuscript.
Acknowledgements
Not applicable
References
- Wright AA, Zhang B, Ray A, et al. Associations between end-of-life discussions, patient mental health, medical care near death, and caregiver bereavement adjustment. JAMA 300 (2008): 1665-1673.
- Arabi YM, Azoulay E, Al-Dorzi HM, et al. How the COVID-19 pandemic will change the future of critical care. Intensive Care Med 47 (2021): 282-291.
- National Institute of Clinical Health and Excellence (NICE) COVID 19: Rapid Guidance for Critical Care (2020).
- Hwang DY, Yagoda D, Perrey HM, et al. Consistency of communication among intensive care unit staff as perceived by family members of patients surviving to discharge. J Crit Care 29 (2014): 134-138.
- Perspectives on telephone and video communication in the ICU during COVID-19. Annals of the American Thoracic Society 11 (2020): 12-18.
- Douglas SL, Daly BJ, Lipson AR. Neglect of quality-of-life considerations in intensive care unit family meetings for long-stay intensive care unit patients. Crit Care Med 40 (2021): 461-467.
- Ye, Siqin, Kronish, et al. Telemedicine Expansion During the COVID-19 Pandemic and the Potential for Technology-Driven Disparities. Journal of General Internal Medicine 36 (2021): 256-258.
