Chronic, Massive Pneumoperitoneum in a Patient without Signs of Peritonitis
Article Information
Matt Kubina1, Mohamad Mouchli2*
1Northeast Ohio Medical University, Rootstown, OH, USA
2Cleveland Clinic, Digestive Diseases and Surgery Institute, Cleveland, OH, USA
*Corresponding Author: Mohamad Mouchli, Cleveland Clinic, Digestive Diseases and Surgery Institute, Cleveland, OH, USA.
Received: 18 January 2023; Accepted: 27 January 2023; Published: 10 February 2023
Citation: Matt Kubina, Mohamad Mouchli. Chronic, Massive Pneumoperitoneum in a Patient without Signs of Peritonitis. Fortune Journal of Health Sciences 6 (2023): 38-40.
Share at FacebookAbstract
Pneumoperitoneum is the presence of air in the abdomen. This can be due to a wide variety of etiologies, many of which are surgical emergencies, yet it can also present as a chronic symptom of underlying pathology. Pneumoperitoneum can be due to primary (idiopathic) or secondary causes, of which the causes are numerous. This can even be due to other pathology unrelated to the GI tract, such as pathology of the thoracic cavity. We present a case of chronic pneumatosis intestinalis that was due to peritoneal blebs likely secondary to an alveolar-peritoneal fistula through the right hemidiaphragm.
Keywords
Pneumoperitoneum; Pneumatosis Intestinalis; CT Imaging
Article Details
1. Introduction
Pneumoperitoneum is the presence of free air in the abdominal cavity seen on plain abdominal radiography or with CT imaging. This can be due to a wide variety of etiologies. In 66% of these cases, this will present as a surgical emergency with peritonitis. This can be seen in the setting of many conditions, including infection, trauma, perforation, iatrogenic causes, and others. However, pneumatosis intestinalis, which is the presence of free air in the extraluminal space, can be due to other pathology unrelated to the GI tract. It can be seen in pulmonary disease, such as COPD and asthma, autoimmune conditions, and drug-induced causes. It can sometimes be a benign symptom as well. We present a case of chronic pneumatosis intestinalis that was present in the patient for over two years and presented with relatively minor, nonspecific symptoms.
2. Case
This patient was a 62-year-old male who presented with initial concerns of abdominal bloating and cramping, which was ongoing for the last two years. History was only significant for a traumatic fall 20 years prior in which he fractured his pelvis, along with appendectomy. He had endorsed having issues with significant unintentional weight loss of approximately 35 pounds in the last two years. He also reported issues of feeling full after eating and being excessively bloated with associated pain for approximately an hour after eating. He also reported intermittent diarrhea but has otherwise been having regular bowel movements. He had not had any fevers or chills.
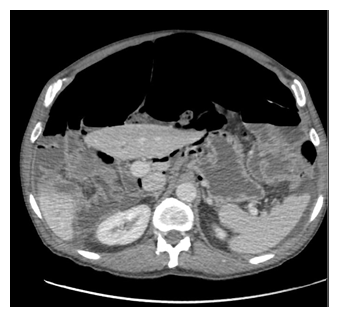
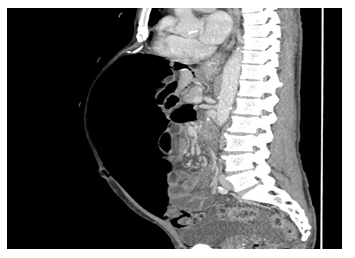
The patient had previous workups which had not revealed a clear cause for his ongoing symptoms. He was tested negative for celiac disease. He had a positive breath test which was reported to be significant for SIBO. Upper endoscopy and colonoscopy had been performed, which showed normal mucosa and colonic diverticulosis. The endoscopist did note that the pylorus was difficult to evaluate as the stomach shape was abnormal. He had undergone CT of the abdomen, which was significant for massive pneumoperitoneum, as well as fluid-filled prominent loops of small bowel concerning for ileus or obstruction (Figure 1,2). Patient declined surgery at that time and opted to pursue a second opinion and was started on bacterial-suppressive antibiotics. His symptoms failed to resolve, and he returned for further evaluation. Repeat CT imaging showed persistent pneumoperitoneum and interval free fluid in the pelvis. There was no site of bowel perforation that could be visualized. Colonoscopy was again performed and was also significant only for diverticulosis. Repeat EGD done at that time revealed a few gastric polyps, which were resected. At that time, the primary diagnosis was chronic pneumatosis intestinalis of unknown etiology.
After further workup at an additional institution, diagnostic laparotomy was recommended to further evaluate his small bowel. There was a significant amount of pneumoperitoneum noted during the operation, along with a moderate amount of serous fluid in the abdomen. There was no evidence of a leak from the stomach. Moderate-to-large small bowel diverticula were noted, but no other pathology was visualized that could explain the free air. At the lower anterior diaphragm near the xiphoid, the peritoneal surface had subperitoneal emphysema suggesting a potential thoracic source for the pneumoperitoneum. Thoracic surgeries were consulted for exploratory right-sided thoracoscopy since he was noted to have peritoneal blebs along the diaphragm most notably, with one also being identified on the liver. Surgical pathology of the biopsies taken from the diaphragm showed mesothelial lined inflamed fibro-connective tissue with multinucleated giant cell reaction and organizing serositis, which were negative for neoplasm. It was concluded that the etiology was most likely due to an alveolar-peritoneal fistula through the right hemidiaphragm.
3. Discussion
Pneumatosis Intestinalis is an alarming symptom that can be secondary to a wide variety of pathologic etiologies, many of which require emergent surgery, making prompt diagnosis critical yet challenging in most patients [1,2]. This can also be a benign presenting symptom, of which the exact incidence is unclear. However, it has been reported to be present in approximately 0.03% of the population and is more typically seen in older adults [3]. Pneumoperitoneum can be due to primary or secondary causes [4]. Primary is often due to idiopathic causes and is responsible for approximately 15% of the total instances of pneumoperitoneum. Secondary causes are numerous. These can be seen in the setting of COPD, immunodeficiency, or acute GI pathology. Free air can also frequently be seen in patients who have had recent surgery, and this typically resolves after approximately one week [5]. Increased pressure in the abdomen, or the lungs and mediastinum, can result in gas diffusing across tissues and into the bowel wall [3]. Treatment and management varies and is dependent both on the clinical status of the patient as well as the underlying cause of the free air. Imaging studies are the best initial tool for investigation and can help differentiate between life-threatening and benign cases, with CT being the most sensitive, with sensitivities ranging from 96-100%.5 Plain abdominal radiographs range in sensitivity from 30-59%, however this approaches 100% in cases of massive pneumoperitoneum, such as the patient presented in this case. More serious abdominal pathology requires surgical management, and delayed diagnosis can result in significant patient morbidity and mortality.
Benign causes in the setting of chronic lung pathology can be asymptomatic or present with mild symptoms that require only conservative medical management [6]. Conservative management includes antibiotic treatment to prevent infection, imaging studies, and observation. Cases of pneumoperitoneum arising from thoracic pathology can also present with signs of acute abdomen and can fully resolve following treatment of the underlying pathology [7]. These patients present with prominent abdominal distension and pain, yet any surgical intervention for abdominal pathology will not aid with the underlying problem and will subject the patient to increased morbidity and mortality risk.
For the thoracic causes of pneumoperitoneum that present non-emergently, the prevalence has not been able to be estimated [8]. Some of the cited etiologies originating from the thorax include mechanical ventilation-induced barotrauma, pneumothorax, and cardiopulmonary resuscitation. Air passage from the mediastinum to the abdomen has been investigated, and possible causes include pleural/diaphragmatic defects, as well as through the diaphragmatic portals and along perivascular connective tissue into the retroperitoneum [9,10]. These are rare occurrences in which the passage of air into the mediastinum occurs and can fail to be visualized with typical imaging studies and even during diagnostic laparotomy.
4. Conclusion
The visualization of free air in the abdomen in a patient complaining of pain and other abdominal symptoms is often a sign of a surgical emergency. However, this can rarely be a presentation of thoracic pathology, which can be benign and managed conservatively. Thoracic and pathology arising from the lungs should remain as a possibility on the differential in cases where air is visualized, yet the presentation and symptoms appear inconsistent with emergent etiologies.
Conflict of Interest:
The authors have no conflicts of interest relevant to this article to disclose.
Funding:
No source of funding was used for this study.
Author Contributions:
Both authors contributed to analyzing the patient case as well as the authoring and editing of the manuscript.
References
- Tahiri M, Levy J, Alzaid S, et al. An approach to pneumatosis intestinalis: Factors affecting your management. Int J Surg Case Rep 6C (2015): 133-137.
- Pinto A, Miele V, Schillirò ML, et al. Spectrum of Signs of Pneumoperitoneum. Semin Ultrasound CT MR 37 (2016): 3-9.
- Im J, Anjum F. Pneumatosis Intestinalis. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing (2022).
- Berritto D, Crincoli R, Iacobellis F, et al. Primary pneumatosis intestinalis of small bowel: a case of a rare disease. Case Rep Surg 2014 (2014): 350312.
- Kumar A, Muir MT. MD; Cohn, Stephen MC, et al. The etiology of pneumoperitoneum in the 21st Journal of Trauma and Acute Care Surgery 73 (2012): 542-548.
- Olson DE, Kim YW, Ying J, et al. CT predictors for differentiating benign and clinically worrisome pneumatosis intestinalis in children beyond the neonatal period. Radiology 253 (2009): 513-519
- Liu D, Torreggiani W, Rowan, et al. Benign pneumatosis intestinalis: A cause of massive pneumoperitoneum in the adult. Canadian Journal of Emergency Medicine 5 (2003): 416-420.
- Mularski RA, Sippel JM, Osborne ML. Pneumoperitoneum: A review of nonsurgical causes. Critical Care Medicine 28 (2000): 2638-2644.
- Gutkin Z, Iellin A, Meged S, et al. Spontaneous pneumoperitoneum without peritonitis. Int Surg 77 (1992): 219-223.
- Paira SO, Roverano S. Bilateral pneumothorax and mediastinal emphysema in systemic lupus erythematosus. Clin Rheumatol 11 (1992): 571-573.