Case of Osseous Lymphoma Involving Bilateral Femur with Secondary Cardiac Involvement
Article Information
Prerana Saraswat1*, Sapna Singh2, Rashmi Dixit2, Anjali Prakash2, Nita Khurana3
1Senior Resident, Department of Radiodiagnosis, Maulana Azad Medical College, New Delhi, India
2Director Professor, Department of Radiodiagnosis, Maulana Azad Medical College, New Delhi, India
3Director Professor, Department of Pathology, Maulana Azad Medical College, New Delhi, India
*Corresponding Author: Prerana Saraswat, Senior Resident, Department of Radiodiagnosis, Maulana Azad Medical College, A-36 Pocket A, Sarita Vihar, New Delhi, 110076, India
Received: 03 August 2021; Accepted: 25 August 2021; Published: 16 September 2021
Citation: Prerana Saraswat, Sapna Singh, Rashmi Dixit, Anjali Prakash, Nita Khurana. Case of Osseous Lymphoma Involving Bilateral Femur with Secondary Cardiac Involvement. Journal of Radiology and Clinical Imaging 4 (2021): 102-112.
Share at FacebookAbstract
We present a case of a 38-year-old male with osseous Diffuse large B-cell lymphoma (DLBCL) involving bilateral femur, with secondary cardiac dissemination involving right atrium and pericardium extending into SVC. The article discusses the osseous involvement of lymphoma and emphasizes the presence of cardiac involvement in the extra nodal lymphoma which may cause secondary symptoms like SVC obstruction. Such cases carry poor prognosis and require treatment modification and careful monitoring to avoid cardiac complications after initiation of chemotherapy. Only few such cases have been described in literature so far.
Keywords
DLBCL; Osseous lymphoma; Cardiac lymphoma; SVC obstruction
DLBCL articles; Osseous lymphoma articles; Cardiac lymphoma articles; SVC obstruction articles
Diffuse large B-cell lymphoma articles Diffuse large B-cell lymphoma Research articles Diffuse large B-cell lymphoma review articles Diffuse large B-cell lymphoma PubMed articles Diffuse large B-cell lymphoma PubMed Central articles Diffuse large B-cell lymphoma 2023 articles Diffuse large B-cell lymphoma 2024 articles Diffuse large B-cell lymphoma Scopus articles Diffuse large B-cell lymphoma impact factor journals Diffuse large B-cell lymphoma Scopus journals Diffuse large B-cell lymphoma PubMed journals Diffuse large B-cell lymphoma medical journals Diffuse large B-cell lymphoma free journals Diffuse large B-cell lymphoma best journals Diffuse large B-cell lymphoma top journals Diffuse large B-cell lymphoma free medical journals Diffuse large B-cell lymphoma famous journals Diffuse large B-cell lymphoma Google Scholar indexed journals Osseous lymphoma articles Osseous lymphoma Research articles Osseous lymphoma review articles Osseous lymphoma PubMed articles Osseous lymphoma PubMed Central articles Osseous lymphoma 2023 articles Osseous lymphoma 2024 articles Osseous lymphoma Scopus articles Osseous lymphoma impact factor journals Osseous lymphoma Scopus journals Osseous lymphoma PubMed journals Osseous lymphoma medical journals Osseous lymphoma free journals Osseous lymphoma best journals Osseous lymphoma top journals Osseous lymphoma free medical journals Osseous lymphoma famous journals Osseous lymphoma Google Scholar indexed journals Cardiac lymphoma articles Cardiac lymphoma Research articles Cardiac lymphoma review articles Cardiac lymphoma PubMed articles Cardiac lymphoma PubMed Central articles Cardiac lymphoma 2023 articles Cardiac lymphoma 2024 articles Cardiac lymphoma Scopus articles Cardiac lymphoma impact factor journals Cardiac lymphoma Scopus journals Cardiac lymphoma PubMed journals Cardiac lymphoma medical journals Cardiac lymphoma free journals Cardiac lymphoma best journals Cardiac lymphoma top journals Cardiac lymphoma free medical journals Cardiac lymphoma famous journals Cardiac lymphoma Google Scholar indexed journals SVC obstruction articles SVC obstruction Research articles SVC obstruction review articles SVC obstruction PubMed articles SVC obstruction PubMed Central articles SVC obstruction 2023 articles SVC obstruction 2024 articles SVC obstruction Scopus articles SVC obstruction impact factor journals SVC obstruction Scopus journals SVC obstruction PubMed journals SVC obstruction medical journals SVC obstruction free journals SVC obstruction best journals SVC obstruction top journals SVC obstruction free medical journals SVC obstruction famous journals SVC obstruction Google Scholar indexed journals Non-Hodgkin’s type articles Non-Hodgkin’s type Research articles Non-Hodgkin’s type review articles Non-Hodgkin’s type PubMed articles Non-Hodgkin’s type PubMed Central articles Non-Hodgkin’s type 2023 articles Non-Hodgkin’s type 2024 articles Non-Hodgkin’s type Scopus articles Non-Hodgkin’s type impact factor journals Non-Hodgkin’s type Scopus journals Non-Hodgkin’s type PubMed journals Non-Hodgkin’s type medical journals Non-Hodgkin’s type free journals Non-Hodgkin’s type best journals Non-Hodgkin’s type top journals Non-Hodgkin’s type free medical journals Non-Hodgkin’s type famous journals Non-Hodgkin’s type Google Scholar indexed journals X--ray articles X--ray Research articles X--ray review articles X--ray PubMed articles X--ray PubMed Central articles X--ray 2023 articles X--ray 2024 articles X--ray Scopus articles X--ray impact factor journals X--ray Scopus journals X--ray PubMed journals X--ray medical journals X--ray free journals X--ray best journals X--ray top journals X--ray free medical journals X--ray famous journals X--ray Google Scholar indexed journals PET CT articles PET CT Research articles PET CT review articles PET CT PubMed articles PET CT PubMed Central articles PET CT 2023 articles PET CT 2024 articles PET CT Scopus articles PET CT impact factor journals PET CT Scopus journals PET CT PubMed journals PET CT medical journals PET CT free journals PET CT best journals PET CT top journals PET CT free medical journals PET CT famous journals PET CT Google Scholar indexed journals Lymphoma articles Lymphoma Research articles Lymphoma review articles Lymphoma PubMed articles Lymphoma PubMed Central articles Lymphoma 2023 articles Lymphoma 2024 articles Lymphoma Scopus articles Lymphoma impact factor journals Lymphoma Scopus journals Lymphoma PubMed journals Lymphoma medical journals Lymphoma free journals Lymphoma best journals Lymphoma top journals Lymphoma free medical journals Lymphoma famous journals Lymphoma Google Scholar indexed journals Transesophageal echocardiography articles Transesophageal echocardiography Research articles Transesophageal echocardiography review articles Transesophageal echocardiography PubMed articles Transesophageal echocardiography PubMed Central articles Transesophageal echocardiography 2023 articles Transesophageal echocardiography 2024 articles Transesophageal echocardiography Scopus articles Transesophageal echocardiography impact factor journals Transesophageal echocardiography Scopus journals Transesophageal echocardiography PubMed journals Transesophageal echocardiography medical journals Transesophageal echocardiography free journals Transesophageal echocardiography best journals Transesophageal echocardiography top journals Transesophageal echocardiography free medical journals Transesophageal echocardiography famous journals Transesophageal echocardiography Google Scholar indexed journals MRI articles MRI Research articles MRI review articles MRI PubMed articles MRI PubMed Central articles MRI 2023 articles MRI 2024 articles MRI Scopus articles MRI impact factor journals MRI Scopus journals MRI PubMed journals MRI medical journals MRI free journals MRI best journals MRI top journals MRI free medical journals MRI famous journals MRI Google Scholar indexed journals
Article Details
1. Introduction
Lymphoma is a common malignancy in elderly occurring in patients with mean age of 60 years. Most lymphomas in elderly are Non-Hodgkin’s type (NHL) with Diffuse Large B-Cell lymphoma (DLBCL) being the most common subtype. Osseous involvement of lymphoma is mainly seen as a part of multifocal nodal/ extra nodal disease and less commonly as a primary osseous lymphoma. Also, secondary cardiac involvement in lymphomas is not common and has been described in literature occurring in 8-20% of cases as per autopsy studies. Primary cardiac lymphoma is even rare accounting for only ~1.3 % of cardiac tumors. Cardiac lymphoma carries poor prognosis due to risk of post chemotherapy life threatening complications.
2. Clinical Presentation
The patient presented to the OPD with chief complaint of progressive painless swelling around bilateral knee joints (right >left) since last two months. The patient also had history of fever and weight loss. There were no presenting cardiorespiratory symptoms. On clinical examination patient had firm nontender swelling above and around the right knee joint. Overlying skin was normal. Mild swelling was also seen around the left knee joint. Pulse rate was 90 per minute and BP was 120/70. Physical examination and laboratory tests were unremarkable.
3. Imaging and Histopathological Findings and Diagnosis
X--ray of bilateral knee joints and chest was performed. Chest Xray did not reveal any significant abnormality. The X-ray of right knee joint revealed an ill-defined permeative type of bony lesion in the distal femur with wide zone of transition (Figure 1). There was cortical thinning with associated soft tissue mass seen on both medial and lateral aspect with fullness of suprapatellar recess. No e/o matrix mineralization was seen. Xray left knee revealed subtle permeative lesion in the distal femur. Soft tissue shadows were unremarkable.
Further, contrast enhanced MRI of bilateral knees was performed which showed a soft tissue mass lesion in the right distal femur showing isointense to hypointense signal on T1WI (Figure 2) and heterogenous iso to hyperintense signal on STIR/T2WI (Figure 3) with erosion of medial cortex and a large extraosseous extension of soft tissue circumferentially around the femur with heterogenous post contrast enhancement (Figure 4). The left distal femur also showed a similar intramedullary soft tissue lesion with no extraosseous extension. Restricted diffusion was noted in the involved areas. Findings were consistent with a malignant lesion likely lymphoma however metastatic bone lesions were also a differential. The biopsy specimen was taken from the mass around right knee. Histopathological examination revealed a cellular tumor comprised of large lymphoid cells intermingled with small lymphocytes. The large lymphoid cells had irregular nuclear membrane, prominent nucleoli, and scanty pale eosinophilic cytoplasm (Figure 11 (a & b)). The cells showed frequent mitosis and increased apoptosis. They were immunoreactive for CD20, PAX5, CD79a which are B cell markers. The small lymphocytes were immunoreactive for CD3 (Figure 11 (c & d)). The findings were consistent with Diffuse large B cell lymphoma.
In view of multifocal bone lesions PET CT was performed. Apart from the lesions in both femur showing FDG uptake, it also revealed a FDG avid heterogenous enhancing mass lesion completely filling the right atrium lumen and extending into the SVC and left brachiocephalic vein causing their luminal occlusion and distension (Figure 7 & 8). The wall of the atrium could not be delineated from the mass. Diffuse pericardial thickening was also seen with focal FDG uptake in the pericardium along the left atrium (Figure 10). On the basis of above findings final diagnosis of extra nodal lymphoma involving bilateral femur with secondary involvement was made.
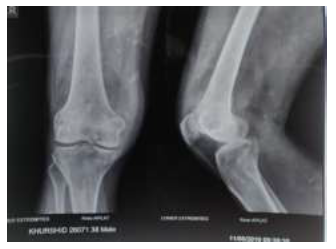
Figure 1: AP and Lateral Xray of the right knee reveal an ill-defined lytic lesion in distal femur with permeative pattern of bone destruction and extraosseous soft tissue with articular margin erosion.
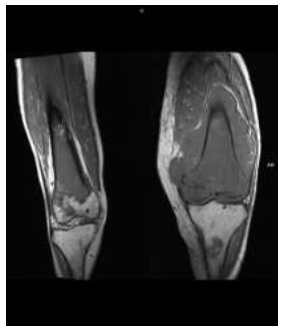
Figure 2: CORONAL T1W MRI image of bilateral knees show a T1 iso-hypointense mass lesion in bilateral distal femur with extraosseous soft tissue.
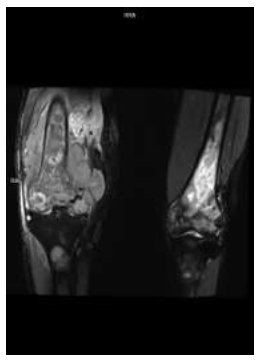
Figure 3: Coronal STIR MRI image of bilateral knees shows heterogenous hyperintense signal within the lesion with erosion of medial cortex of right femur (*).
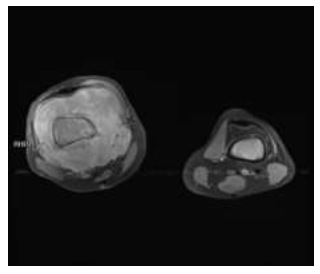
Figure 4: Axial T1 post contrast FATSAT MRI image shows mass in the right distal femur with heterogenous enhancement and circumferential soft tissue around the femur. Similar enhancing mass lesion is also seen in left distal femur with no extraosseous soft tissue.
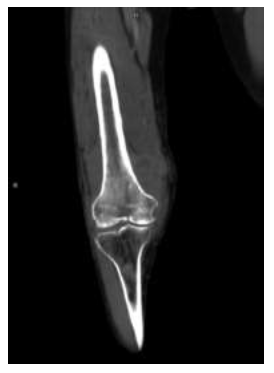
Figure 5: CORONAL CECT image of the right thigh and knee in soft tissue window shows that the lesion is causing permeative type of bone destruction in the distal femur with soft tissue component showing heterogenous enhancement.
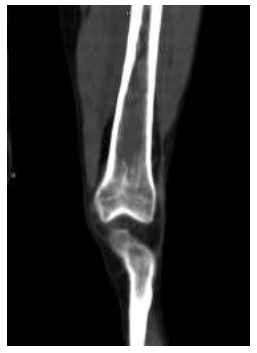
Figure 6: Coronal CECT image of the left thigh also shows similar lesion in left distal femur with intramedullary expansion and wide zone of transition.
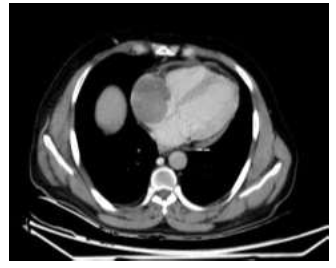
Figure 7: AXIAL CECT images of the chest shows another enhancing mass lesion in the right atrium displacing the interatrial septum mildly. There is diffuse pericardial thickening (--).
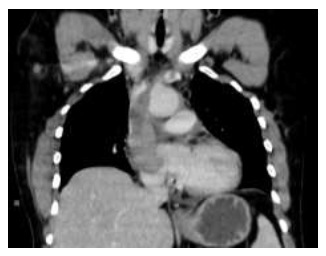
Figure 8: CORONAL CECT image of the chest shows the mass extending into the SVC and left brachiocephalic vein.
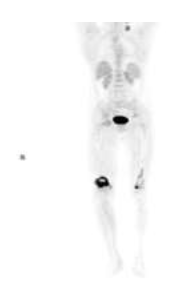
Figure 9: CORONAL PET images show FDG avid lesions in bilateral distal femur.
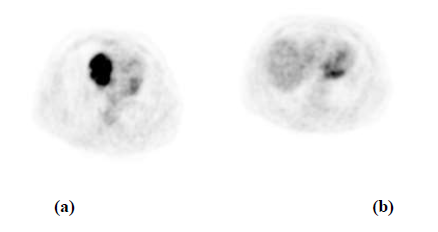
Figure 10: (a) AXIAL PET images reveal increased FDG uptake within the lesion in the right atrium and; (b) Pericardial region.
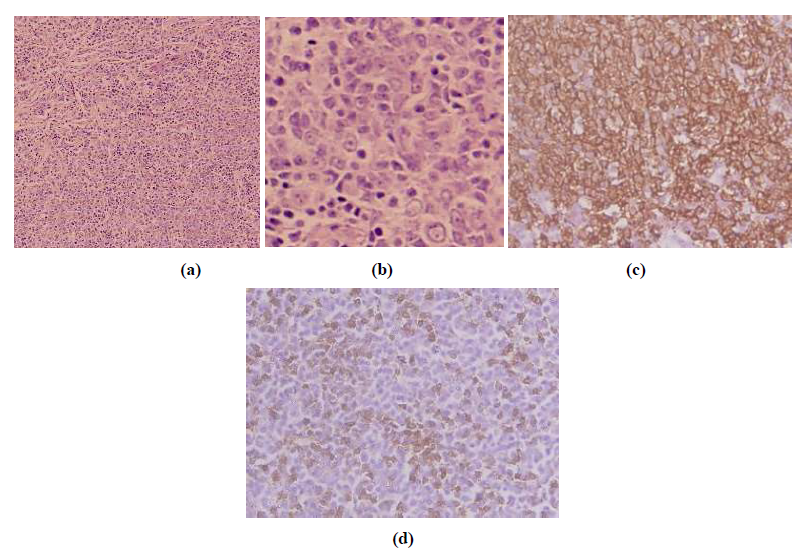
Figure 11: (a) Diffuse infiltrate of large lymphoid cells with scattered small lymphocytes (Hematoxylin & eosin x 200x); (b) Large lymphoid cells show prominent nucleoli and scanty to moderate pale eosinophilic cytoplasm; (c) Diffuse CD 20 immunoreactivity in the large lymphoid cells (CD20 Streptavidin peroxidase with DAB as chromogen x 600); (d) Scattered small lymphocytes show intense CD3 reactivity (CD3, streptavidin peroxidase with DAB as chromogen).
4. Discussion
Lymphoma is a relatively common malignancy of all ages mostly occurring in adults and elderly and presents as large nodal or extra nodal masses. DLBCL is the most common histopathological subtypes of extra nodal lymphomas. Lymphoma of the bone constitutes ~7% of bone malignancies. Osseous lymphomas have been divided into four types [1]. A solitary Primary Bone Lymphoma (PBL) [2], multifocal PBL without soft tissue or nodal involvement [3], simultaneous osseous and nodal/soft tissue involvement, and [4] osseous involvement presenting more than 6 months after confirmed diagnosis of lymphoma [2]. PBL has been described as solitary or multifocal osseous involvement in absence of distant nodal/ extra nodal disease within 6 months of diagnosis. PBL tends to involve the appendicular skeleton whereas secondary lymphomas more commonly involve vertebrae, skull, and pelvis. Solitary or multifocal PBL have a predilection for bones around knee joints including femur and tibia. The site of involvement in long bones includes meta diaphyseal region in most cases, however localized involvement of epiphysis and diaphysis alone may also be seen. On radiographic imaging, bone lymphomas usually appear as ill-defined lesions with permeative or moth-eaten type of bone destruction. The pattern maybe lytic, mixed lytic and sclerotic or purely sclerotic. They show wide zone of transition and are usually associated with soft tissue masses. They can cause cortical erosion and pathological fractures. They also have the tendency to cross the joints and involve adjoining bones and soft tissues. Sometimes the lesions can be subtle on radiographs and the involved bone may appear as near normal. MRI helps in assessment of marrow involvement and also soft tissue extension. It also serves as imaging for further assessment of lesions which are subtle or indefinite on radiographs and also helps to identify multifocal lesions which can be missed on plain radiographs.
CT has a limited role and mainly aids in identifying bony erosions, pathological fractures, matrix mineralization and characterize periosteal reaction. The imaging patterns of osseous lymphoma are however not specific and has multiple mimics including metastasis, chronic osteomyelitis, osteosarcoma, and Ewing’s sarcoma. When present in axial skeleton the differential diagnosis of multiple myeloma and metastasis needs to be considered especially in elderly patients with multifocal involvement. Lymphomas of bones carry good prognosis and 5-year survival rate as high as ~80% has been described [4]. The treatment mainstay is chemo and radiotherapy.
Cardiac lymphoma is also most commonly seen as secondary involvement in disseminated lymphoma and is seen in approximately 30% cases of disseminated lymphoma [3]. Clinical presentation of patient with cardiac involvement may be varied like dyspnea, chest pain, cardiac failure, arrhythmias, thromboembolism and hemodynamic disturbances due to mass effect/valve involvement. Most commonly patient with cardiac masses present with cardiac failure, followed by tumor thromboembolism. Few studies have also reported patients presenting with cardiac ischemia and raised troponin levels due to myocardial infiltration by lymphoma [5]. Due to advancement of imaging techniques and early detections sometimes the findings are incidental without any initial symptoms as seen in this case [4]. Imaging modalities used for evaluation of cardiac masses include echocardiography, CT, and Contrast-Enhanced MRI. Echocardiography is non-invasive first imaging of choice for evaluation of suspected cardiac lesions. It allows localization of mass and assessment of related cardiac functional abnormalities at the same time. Transesophageal echocardiography (TEE) provides better visualization window as compared to transthoracic echocardiography. TEE has sensitivity of almost 100 % in detection of cardiac masses.
CT has excellent spatial resolution and allows characterization of the mass and its anatomical relations. it however has low soft tissue contrast and therefore has limited evaluation of myocardium and epicardium. Cardiac MRI is the preferred modality for cardiac mass assessment since it provides better soft tissue contrast without contrast administration and allows functional as well viability evaluation.
Most cardiac lymphomas, ~80% are DLBCL types. They mainly present as single or multiple infiltrating masses involving myocardium and epicardium. Pericardial thickening and effusion are also common findings. Hemopericardium can also occur in some cases. Right sided cardiac involvement is more as compared to left, right atrium being the commonest site [6, 7]. SVC involvement is also seen in many cases causing SVC obstruction. There may be encasement of coronary vessels in the epicardium. Involvement of the atrioventricular septal walls is also seen Few cases reports have also documented diffuse cardiac involvement of lymphoma seen as multiple diffuse epicardial and myocardial lymphomatous deposits, diffuse pericardial thickening and pericardial effusion causing cardiac failure [8].
On CT cardiac lymphomas appear as iso-hypoattenuating infiltrating masses with involvement of the epicardium. The enhancement is mostly heterogenous. On MRI lymphomas are hypointense on T1WI and hyperintense on T2WI. CE imaging shows heterogenous enhancement within the mass. Delayed CE images also depict the extent of mass and myocardial viability. CE MRI also helps to distinguish between tumor and bland thrombus. The differential diagnosis considerations of cardiac lymphoma include metastasis, myxomas, thrombus and sarcomas. Most common cardiac malignancy is metastasis commonly occurring from lung carcinoma, breast carcinoma or malignant melanoma [9]. It may be direct extension of tumor mass or hematogenous deposits from the primary malignancy. Most common primary sarcoma of heart is angiosarcoma. As compared to lymphoma the sarcomas are more aggressive and appear as necrotic masses with heterogenous enhancement pattern on contrast enhanced CT and MRI. Invasion into the surrounding structures including cardiac valves and vessels is more commonly seen in sarcomas.
Cardiac involvement in lymphoma carries poor prognosis and median survival of patient is approximately 3 months [11]. Chemotherapy is the mainstay of treatment while the other modalities include radiotherapy and palliative surgical resection. The advent of chemotherapy has led to prolongation of survival time [11]. The current treatment guidelines for DLBCL include chemotherapy with CHOP regime (Cyclophosphamide, doxorubicin, vincristine, and prednisone) along with rituximab [1, 10].
Chemotherapy carries risk of potential complications including arrythmias, cardiac thrombo-embolism, cardiac failure, and myocardial rupture due to tumor lysis. Few case reports have documented favorable outcomes with tailored chemotherapy regime which includes initial low dose chemotherapy followed by standard dose chemotherapy [12]. Imaging is an essential tool in pre and post treatment patient monitoring. Echocardiography and CE MRI are helpful in evaluation of cardiac function and post treatment fibrosis of the myocardium.
5. Conclusion
Disseminated lymphomas with cardiac involvement have been less frequently described in previous literature. It carries poor prognosis and requires dose modification and careful treatment monitoring to achieve better prognosis.
Declaration of Conflict of Interest
I hereby declare that there is no issue of conflict of interest associated with this publication.
References
- Shah, Hina J, Keraliya, et al. Diffuse Large B-Cell Lymphoma in the Era of Precision Oncology: How Imaging Is Helpful. Korean Journal of Radiology 18 (2017): 54-70.
- Montoya, Simone, Moorthy, et al. Primary Lymphoma of Bone. Contemporary Diagnostic Radiology 40 (2017): 1-5.
- Lim CY, Ong KO. Imaging of musculoskeletal lymphoma. Cancer Imaging 13 (2013): 448-457.
- Krishnan A, Shirkhoda A, Tehranzadeh J, et al.. Primary Bone Lymphoma: Radiographic–MR Imaging Correlation. RadioGraphics 23 (2003): 1371-1383.
- Jeudy, Jean, Kirsch, et al. From the radiologic pathology archives: Cardiac lymphoma: Radiologic-pathologic correlation. Radiographics 32 (2012): 1369-1380.
- Sheppard MN, Mohiaddin R. Tumors of the heart. Future Cardiol 6 (2010): 181-193.
- O'Mahony D, Peikarz RL, Bandettini WP, et al.
Cardiac involvement with lymphoma: a review of the literature. Clin Lymphoma Myeloma 8 (2008): 249-252.
- Jeudy J, Burke AP, Frazier AA. Cardiac Lymphoma. Radiol Clin North Am 54 (2016): 689-710.
- Bligh MP, Borgaonkar JN, Burrell SC, et al. Spectrum of CT Findings in Thoracic Extranodal Non-Hodgkin Lymphoma. Radiographics 37 (2017): 439-461.
- Ishiwata T, Harada N, Ko R, et al. Malignant lymphoma with diffuse cardiac involvement detected by multiple imaging examinations: a case report. J Med Case Rep 6 (2012): 193.
- Gadage V, Kembhavi S, Kumar P, et al. Primary cardiac diffuse large B-cell lymphoma with activated B-cell-like phenotype. Indian J Pathol Microbiol 54 (2011): 591-593.
- Al-Mehisen R, Al-Mohaissen M, Yousef H. Cardiac involvement in disseminated diffuse large B-cell lymphoma, successful management with chemotherapy dose reduction guided by cardiac imaging: A case report and review of literature. World J Clin Cases 7 (2019): 191-202.
- Gordon MJ, Danilova O, Spurgeon S, et al. Cardiac non-Hodgkin's lymphoma: clinical characteristics and trends in survival. Eur J Haematol 97 (2016): 445-452.
- Shah K, Shemisa K. A "low and slow" approach to successful medical treatment of primary cardiac lymphoma. Cardiovasc Diagn Ther 4 (2014): 270-273.
