Cannonball Metastasis as a Presenting Imaging Feature of Cancer of Unknown Primary
Article Information
Marwa Najaf*
Queen Elizabeth Hospital Birmingham, UK
*Corresponding Author: Marwa Najaf, Queen Elizabeth Hospital Birmingham, UK.
Received: 31 October 2022; Accepted: 10 November 2022; Published: 18 November 2022
Citation:
Najaf M. Cannonball Metastasis as a Presenting Imaging Feature of Cancer of Unknown Primary. Journal of Radiology and Clinical Imaging 5 (2022): 50-52.
Share at FacebookKeywords
Cannonball Metastasis
Cannonball Metastasis
Cannonball Metastasis articles Cannonball Metastasis Research articles Cannonball Metastasis review articles Cannonball Metastasis PubMed articles Cannonball Metastasis PubMed Central articles Cannonball Metastasis 2023 articles Cannonball Metastasis 2024 articles Cannonball Metastasis Scopus articles Cannonball Metastasis impact factor journals Cannonball Metastasis Scopus journals Cannonball Metastasis PubMed journals Cannonball Metastasis medical journals Cannonball Metastasis free journals Cannonball Metastasis best journals Cannonball Metastasis top journals Cannonball Metastasis free medical journals Cannonball Metastasis famous journals Cannonball Metastasis Google Scholar indexed journals CT thorax articles CT thorax Research articles CT thorax review articles CT thorax PubMed articles CT thorax PubMed Central articles CT thorax 2023 articles CT thorax 2024 articles CT thorax Scopus articles CT thorax impact factor journals CT thorax Scopus journals CT thorax PubMed journals CT thorax medical journals CT thorax free journals CT thorax best journals CT thorax top journals CT thorax free medical journals CT thorax famous journals CT thorax Google Scholar indexed journals pulmonary nodules articles pulmonary nodules Research articles pulmonary nodules review articles pulmonary nodules PubMed articles pulmonary nodules PubMed Central articles pulmonary nodules 2023 articles pulmonary nodules 2024 articles pulmonary nodules Scopus articles pulmonary nodules impact factor journals pulmonary nodules Scopus journals pulmonary nodules PubMed journals pulmonary nodules medical journals pulmonary nodules free journals pulmonary nodules best journals pulmonary nodules top journals pulmonary nodules free medical journals pulmonary nodules famous journals pulmonary nodules Google Scholar indexed journals CT imaging articles CT imaging Research articles CT imaging review articles CT imaging PubMed articles CT imaging PubMed Central articles CT imaging 2023 articles CT imaging 2024 articles CT imaging Scopus articles CT imaging impact factor journals CT imaging Scopus journals CT imaging PubMed journals CT imaging medical journals CT imaging free journals CT imaging best journals CT imaging top journals CT imaging free medical journals CT imaging famous journals CT imaging Google Scholar indexed journals Alpha Fetoprotein articles Alpha Fetoprotein Research articles Alpha Fetoprotein review articles Alpha Fetoprotein PubMed articles Alpha Fetoprotein PubMed Central articles Alpha Fetoprotein 2023 articles Alpha Fetoprotein 2024 articles Alpha Fetoprotein Scopus articles Alpha Fetoprotein impact factor journals Alpha Fetoprotein Scopus journals Alpha Fetoprotein PubMed journals Alpha Fetoprotein medical journals Alpha Fetoprotein free journals Alpha Fetoprotein best journals Alpha Fetoprotein top journals Alpha Fetoprotein free medical journals Alpha Fetoprotein famous journals Alpha Fetoprotein Google Scholar indexed journals Cancer of Unknown Primary articles Cancer of Unknown Primary Research articles Cancer of Unknown Primary review articles Cancer of Unknown Primary PubMed articles Cancer of Unknown Primary PubMed Central articles Cancer of Unknown Primary 2023 articles Cancer of Unknown Primary 2024 articles Cancer of Unknown Primary Scopus articles Cancer of Unknown Primary impact factor journals Cancer of Unknown Primary Scopus journals Cancer of Unknown Primary PubMed journals Cancer of Unknown Primary medical journals Cancer of Unknown Primary free journals Cancer of Unknown Primary best journals Cancer of Unknown Primary top journals Cancer of Unknown Primary free medical journals Cancer of Unknown Primary famous journals Cancer of Unknown Primary Google Scholar indexed journals metastatic adenocarcinomas articles metastatic adenocarcinomas Research articles metastatic adenocarcinomas review articles metastatic adenocarcinomas PubMed articles metastatic adenocarcinomas PubMed Central articles metastatic adenocarcinomas 2023 articles metastatic adenocarcinomas 2024 articles metastatic adenocarcinomas Scopus articles metastatic adenocarcinomas impact factor journals metastatic adenocarcinomas Scopus journals metastatic adenocarcinomas PubMed journals metastatic adenocarcinomas medical journals metastatic adenocarcinomas free journals metastatic adenocarcinomas best journals metastatic adenocarcinomas top journals metastatic adenocarcinomas free medical journals metastatic adenocarcinomas famous journals metastatic adenocarcinomas Google Scholar indexed journals choriocarcinoma articles choriocarcinoma Research articles choriocarcinoma review articles choriocarcinoma PubMed articles choriocarcinoma PubMed Central articles choriocarcinoma 2023 articles choriocarcinoma 2024 articles choriocarcinoma Scopus articles choriocarcinoma impact factor journals choriocarcinoma Scopus journals choriocarcinoma PubMed journals choriocarcinoma medical journals choriocarcinoma free journals choriocarcinoma best journals choriocarcinoma top journals choriocarcinoma free medical journals choriocarcinoma famous journals choriocarcinoma Google Scholar indexed journals osteosarcoma articles osteosarcoma Research articles osteosarcoma review articles osteosarcoma PubMed articles osteosarcoma PubMed Central articles osteosarcoma 2023 articles osteosarcoma 2024 articles osteosarcoma Scopus articles osteosarcoma impact factor journals osteosarcoma Scopus journals osteosarcoma PubMed journals osteosarcoma medical journals osteosarcoma free journals osteosarcoma best journals osteosarcoma top journals osteosarcoma free medical journals osteosarcoma famous journals osteosarcoma Google Scholar indexed journals metastatic lung cancer articles metastatic lung cancer Research articles metastatic lung cancer review articles metastatic lung cancer PubMed articles metastatic lung cancer PubMed Central articles metastatic lung cancer 2023 articles metastatic lung cancer 2024 articles metastatic lung cancer Scopus articles metastatic lung cancer impact factor journals metastatic lung cancer Scopus journals metastatic lung cancer PubMed journals metastatic lung cancer medical journals metastatic lung cancer free journals metastatic lung cancer best journals metastatic lung cancer top journals metastatic lung cancer free medical journals metastatic lung cancer famous journals metastatic lung cancer Google Scholar indexed journals
Article Details
1. Case
A 56 year old male presented with three weeks of shortness of breath associated with cough productive of green sputum and haemoptysis. He also reported significant weight loss, myalgia and chest pain upon coughing. He has no past medical or surgical history and is an ex-smoker. On examination, observations were normal aside from tachycardia. Coarse crackles were audible throughout the chest. Abdominal palpation revealed tenderness in the right upper quadrant with a four finger breadth hepatomegaly. No other clinical findings were identified. Bloods revealed a C-reactive protein 183, corrected calcium 2.43, alanine transaminase 60 u/L, alkaline phosphatase 672 u/L, hemoglobin 122g/L and white cell count 13.5 × 10*9/L.
Initial imaging modality used was a plain chest x-ray which revealed multiple bilateral well-circumscribed pulmonary lesions (Figure 1). A CT thorax, abdomen and pelvis was arranged which again revealed multiple bilateral lung nodules and masses up to 7cm in the left lung base (Figure 2). Some of the small lung nodules contained cavitation. Mediastinal and bilateral hilar lymphadenopathy was observed and was causing external compression on the pulmonary arteries and completely occluding the right upper lobe pulmonary artery. Bilateral apical lung scarring was also noted. In addition, multiple liver, adrenal and renal lesions were identified. Mild pancreatic duct dilatation was observed in the body and a possible low attenuation lesion in the centre of the pancreatic head. Peri-pancreatic and lower para-oesophageal lymphadenopathy was also present.

Figure 1: A plain chest c-ray showing extensive bilateral lung nodules.
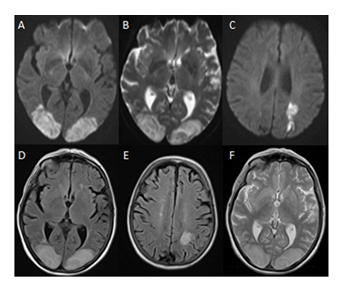
Figure 2: CT thorax, abdomen, pelvis with contrast showing multiple bilateral lung nodules, multiple bilobar liver metastases and multiple low attenuation bilateral renal lesions.
2. Discussion
20-54% of malignant tumours metastasise to the lungs which makes the lung the second most common site for metastasis [1]. Solitary lung nodules can either be a primary lung tumour or a metastasis from a primary elsewhere. However, multiple lung nodules >5mm are highly suspicious of metastatic lung cancer [1]. Despite this, pulmonary nodules should not be assumed to be metastatic without performing a biopsy [1].
Cancers that commonly metastasise to the lung include breast, lung, colorectal, renal cell carcinoma and pancreatic. These typically present in middle aged or older adults and have a prevalence of 1-100,000 [2]. Other primaries that metastasise to the lungs include testicular, choriocarcinoma, osteosarcoma, thyroid, malignant melanoma, ewing sarcoma and adrenal [3-5]. Occasionally a primary cannot be identified and is termed Cancer of unknown primary (CUP) [3].
A cannonball appearance of metastasis is the term often given to larger nodules and masses observed in the lung field [4]. Alternatively, lung metastasis can be numerous and small giving a “milliary pattern” as seen in malignant melanoma, skeletal sarcoma, testicular carcinoma and adenocarcinomas [5].
CT imaging is excellent not only at visualising the nodules but also to look for the primary tumour site. If a likely primary is identified, tumour type specific treatment should be commenced. In the absence of radiographically detected or clinically suspected primary site, the least risk associated site for core needle biopsy should be identified by the reporting radiologist. Ultrasound guided or surgical biopsy should be sent for histopathological, molecular and genetic testing [6]. Tumour markers may also aid in the identification of the primary cancer [6]. For example, beta Human Chorionic Gonadotrophin (HCG) is significantly elevated in pure choriocarcinoma (>1000 IU/L, normal range is <2 mIU/mL) and these do not produce Alpha Fetoprotein (AFP).
A CT thorax, abdomen and pelvis did not identify a primary. AFP and beta HCG was done which was 2 and 20144.9 respectively. A right axillary biopsy was carried out showing metastatic adenocarcinoma with immunophenotype. An urothelial origin was suggested and a pulmonary origin could also not be excluded.
In an ideal scenario the above workup will suffice to identify the primary site of disease. Cancer of Unknown Primary (CUP) is a histologically diagnosed metastatic cancer where the primary tumour site cannot be located with standard evaluation and imaging studies [6]. In patients with presumed CUP a primary site is identified in less than 30% during the above workup and less than 20% can be further classed into favourable or treatable based on clinical presentation, histological and radiological findings. Patient can present with a variety of signs and symptoms relating to the site of malignancy owing to the diversity of CUP [6]. It makes up approximately 2-5% of all diagnosed cancers worldwide [6]. Approximately 50% of CUP are metastatic adenocarcinomas, 15% are squamous cell carcinoma and about 30% are undifferentiated or poorly differentiated carcinomas [6].
It is of paramount important to work closely in a multidisciplinary team with oncologist and radiologist in order to prevent unnecessary investigation, to perform the appropriate scan/protocol in order to answer the physicians clinical question [7]. A multidisciplinary team meeting took place which concluded that most likely this is CUP.
Consent for Publication
Written consent was gained from the patient for the publication of this case.
Competing Interests
There are no conflicts of interest to declare in writing this case report.
References
- Caparica R, Mak MP, Rocha CH, et al. Pulmonary Nodules in Patients With Nonpulmonary Cancer: Not Always Metastases. J Glob Oncol 2 (2016): 138-144.
- Chen H, Stoltzfus K, Lehrer E, et al. The Epidemiology of Lung Metastases. Front Med 8 (2021): 723396.
- Jamil A, Kasi A. Lung Metastasis. [Updated 2022 Feb 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing (2022).
- Seo J, Im J, Goo J, et al. Atypical Pulmonary Metastases: Spectrum of Radiologic Findings. Radiographics. 21 (2001): 403-417.
- Collins J, Eric J. Stern. Chest Radiology (2008).
- Lee MS, Sanoff HK. Cancer of unknown primary. BMJ 7 (2020): 371.
- Kim KW, Krajewski KM, Jagannathan JP, et al. Cancer of unknown primary sites: what radiologists need to know and what oncologists want to know. AJR Am J Roentgenol 200 (2013): 484-492.
