Bilateral Malignant Pleural Effusion as an Initial Manifestation of Acute Lymphoblastic Leukemia: A Rare Case Report
Article Information
Gajjar Jay Daxay1, Vyakhya1, Ajeta Vijaykumar Gupta1, Bhagwan Sahai Sharma2, Susheel Kumar Saini3*, Madhur sarthalia1, Ajay Kumar Saini4
1MBBS, MD Pediatrics trainee, NIMS medical college, Jaipur, India
2MBBS, MD Pediatrics, Senior Professor and Head, Pediatric pulmonology division, NIMS medical college, Jaipur, India
3MBBS, MD Pediatrics, FNB Pediatric Intensive care, Assistant Professor, NIMS medical college, Jaipur, India
4MBBS, DNB Pediatrics, SGMH, Delhi, India
*Corresponding Author: Susheel Kumar Saini, MBBS, MD Pediatrics, FNB Pediatric Intensive care, Assistant Professor, NIMS medical college, Jaipur, India.
Received: 29 March 2023; Accepted: 28 April 2023; Published: 05 May 2023
Citation:
Gajjar Jay Daxay, Vyakhya, Ajeta Vijaykumar Gupta, Bhagwan Sahai Sharma, Susheel Kumar Saini, Madhur sarthalia, Ajay Kumar Saini. Bilateral Malignant Pleural Effusion as an Initial Manifestation of Acute Lymphoblastic Leukemia: A Rare Case Report. Journal of Pediatrics, Perinatology and Child Health. 7 (2023): 83-85.
Share at FacebookAbstract
Exudative pleural effusion in children is mainly caused by bacterial infections. Leukemia rarely presents as pleural effusion as the first manifestation of the disease process. Bilateral malignant pleural effusion as an initial manifestation that leads to the diagnosis of an underlying acute lymphoblastic leukemia is a rare event. Most commonly pleural effusion is seen as complication in solid tumors such as the lung, lymphomas, carcinomas of the breast and gastrointestinal tract.
We report a case of 15 yrs. old girl presented with bilateral massive pleural effusion and respiratory failure. She was initially diagnosed as a case of pulmonary tuberculosis but evaluated further due to poor response to antitubercular treatment. She was finally diagnosed as a case of B cell Acute Lymphoblastic Leukemia. She underwent induction chemotherapy which led to significant clinical improvement due to resolution of the pleural effusion. The patient is on chemotherapy at present. This case report highlights the importance of cytopathological analysis of body cavity fluids in the diagnosis of underlying unsuspected malignancies.
Keywords
Bilateral pleural effusion; Leukemia; Malignant; Rare
Article Details
1. Objective
Pleural effusion is defined as accumulation of fluid in the pleural space. The condition can have various causes and may be a life threatening [1]. Malignancy is a rare cause of pleural effusion in children. Lymphoma is the most common malignancy associated with pleural effusion. About 5% of patients with Hodgkin's or non-Hodgkin's lymphoma will develop a pleural effusion. In addition, T cell lymphoblastic leukemia can also cause a malignant pleural effusion. Common symptoms of pleural effusion are dyspnea, cough, and chest pain that are more severe in effusions with greater volumes. Respiratory distress is an important symptom that needs urgent management [2].
When effusions do occur in the setting of malignancy, they commonly have an infectious etiology [3]. Malignant Pleural Effusion (MPE) may be underdiagnosed because of low diagnostic yield from cyto-pathological analysis. Since MPE may be an indicator of poor prognosis [3], a valid and timely diagnosis is of utmost importance.
Leukemic infiltration of the lungs may occur as a part of a systemic relapse or rarely as an isolated pulmonary leukemic infiltration. This case highlights the rare initial presentation of B Cell ALL (Acute Lymphoblastic Leukemia) as isolated pleural effusion [4].
2. Case Presentation
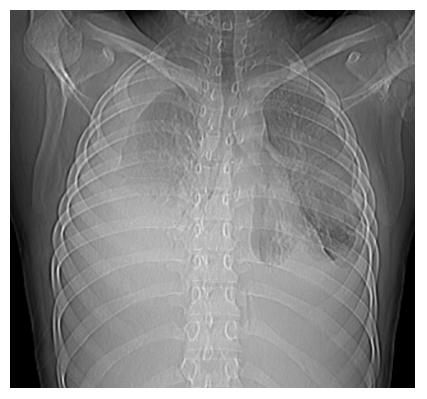
A 15 years-old girl presented to the pediatric emergency department with fever on and off for 2 months and progressively increasing difficulty in breathing for 15 days. She took OPD based treatment but symptoms not relieved. He had no previous history of traveling, blood transfusion, bleeding or previous medical or surgical treatment. She had history of contact with pulmonary tuberculosis as her mother was taking Antitubercular Treatment (ATT) for tuberculosis for last 6 months. Upon presentation, during physical examination, she had fever, tachycardia, tachypnoea and severe difficulty in breathing. On respiratory system examination she had severely decreased breath sounds on bilateral lung fields (Right > Left) along with nasal flaring and chest retractions. The rest of the examination was normal as there was no lymphadenopathy, organomegaly or tenderness. The patient was admitted, and laboratory investigations were carried out. Ultrasound examination revealed bilateral moderate to severe pleural effusion. Her laboratory workup showed hemoglobin 7.6 g/dl, total leukocytes count 3790/mm3 with 52% neutrophils, and platelets 273,000/mm3. Her ESR was 104 mm while liver function test came normal. Her creatinine and electrolytes were normal. Peripheral blood examination was negative for any abnormal cells. Pleural fluid examination showed Protein 2.8 g/dl, total leukocytes count 1884/mm3 with 68% neutrophils, ADA 84 IU/L. Pleural fluid CB NAAT came negative and sputum for AFB was also negative. CT chest was done which was negative for mediastinal lymphadenopathy. As she had history of contact with tuberculosis and pleural fluid examination was examination was in favor of tubercular pleural effusion; she was started on ATT along with antibiotics and other supportive treatment. She required mechanical ventilation for 4 days in view of respiratory failure on admission. Bilateral ICD were placed on admission for bilateral pleural effusion which were removed later. The patient was discharged on request on ATT from DOTS at day 8 after significant improvement in condition. She was readmitted after 2 months with complaint of intermittent fever, difficulty in breathing and puffiness over face. On USG chest she had moderate bilateral pleural effusion which was managed with repeated tapping. Hemogram showed hemoglobin 6.8 g/dl, total leukocytes count 2480/mm3 with 87% neutrophils and platelets 227,000/mm3. Pleural fluid examination showed total protein of 4.4 g/dl, sugar 21 mg/dl, total cell count of 7600/mm3 with neutrophilic predominance, ADA 198 U/L, negative for CB NAAT. Pleural fluid culture came positive for Pseudomonas aeruginosa. Antibiotics upgraded as per culture sensitivity; after which fever subsided but pleural effusion was resistant to repeated tapping. CECT chest was done which showed multiple small lymph nodes of various sized along with features of pneumonitis. As the pleural effusion of patient was not responding, pleural fluid examination for malignant cells was done which showed lymphocytic infiltration mixed with few atypical large lymphoid cells. Immunophenotyping done from pleural fluid which show 73% B lineage lymphoblasts, positive for CD13, CD10, CD19, CD22, CD38, CD34, CD123, CD45, HLA DR and negative for CD33, CD117, CD64, CD20, CD3, CD7. Peripheral blood smear came negative for atypical cells and blasts. Bone marrow aspiration and biopsy done which also showed B cell ALL. This confirmed the cause of effusion as the B cell ALL. The patient was referred to the department of Clinical hematology for further treatment (Figure 1).
3. Discussion
A hematological malignancy rarely manifests with bilateral massive leukemic pleural effusion as an initial presentation. Malignant pleural effusions can occur in patients with solid tumor and lymphoid malignancies, such as Hodgkin lymphoma, adult T-cell lymphoma, and precursor T- lymphoblastic lymphoma.4 Acute and chronic leukaemia are rarely accompanied by pleural effusions [5].
Possible mechanisms of leukaemic pleural effusion in patients with ALL include extramedullary proliferation of a quiescent leukaemic clone with subsequent metastasis to the bone marrow. The other possible mechanism of the fluid formation include shedding of malignant cells into the pleural space, lymphatic obstruction due to lymphomatous infiltration of the pulmonary and mediastinal lymph nodes or obstruction of the thoracic duct.
There are variable views about the prognostic significance of pleural involvement in leukemias. According to some it does not affect the rate of remission and survival, while others report a worse prognosis. Currently available studies suggest that most of the patients with pleural effusion associated leukemia have active disease at the time of presentation [6]. Patients with hematologic malignancies are prone to infection because of their inherent immunosuppression, but other causes are also common. As in our case in addition to malignant pleural effusion; patient also had positive growth of Pseudomonas aeruginosa in pleural fluid. Pleural effusions associated with hematological malignancy usually disappear after induction chemotherapy for primary malignancy and result in clinical improvement. However, in some patients no remission occurs and respiratory failure ensues due to massive pleural effusion [7]. Intrapleural chemotherapy and chemical sclerosis is indicated in such cases [6].
4. Conclusion
On the basis of our case, we conclude that a normal complete blood cell count does not exclude a diagnosis of ALL. This case emphasizes the need to be vigilant in determining the causes of pleural effusion in patients whose other causes have been ruled out. Most patients with a malignant effusion have a known history of primary, but sometimes a positive effusion may be the first sign of an unsuspected malignancy. Hence, cytological examination of a serous effusion may offer the possibility of an early and accurate diagnosis by using minimal intervention permitting appropriate therapy.
References
- Fischer GB, Mocelin HT, Andrade CF, et al. When should parapneumonic pleural effusions be drained in children? Paediatric respiratory reviews 26 (2018): 27-30.
- Beaudoin S, Gonzalez AV. Evaluation of the patient with pleural effusion. CMAJ 190 (2018): E291-E295.
- FaizSA, SahayS, JimenezCA. Pleural effusions inacute and chronic leukemia and myelodysplastic syndrome. Curr Opin Pulm Med 20 (2014): 340- 346.
- Alexandrakis MG, Passam FH, Kyriakou DS, et al. Pleural effusions in hematologic malignancies. Chest 125 (2005): 1546-1555.
- Raina S, Kaul R, Mahesh DM, et al. Pleural effusions in acute myeloid leukaemia. J Assoc Physicians India 56 (2008): 914-915.
- Fatih T, Selim Y, Mesut A, et al. An unusual cause of unilateral pleural effusion in the setting of aortic stenosis: acute myeloid leukemia. Intern Med 46 (2007): 325-327.
- Bronner GM, Baas P, Beijnen JH. Pleurodesis in malignant pleural effusion [Article in Dutch]. Ned Tijdschr Geneeskd 141 (1997): 1810-1814.