Assessment of Complete Blood Count in the Breast Cancer Patients of Arsenic Exposed Population of Bihar.
Article Information
Yerravarapu Vamsi Krishna1, Chandrajeet Kumar1 and Arun Kumar2*
1Department of Biochemistry, YBN University, Ranchi, Jharkhand, India
2Mahavir Cancer Sansthan and Research Centre, Patna, Bihar, India
*Corresponding Author: Arun Kumar, Mahavir Cancer Sansthan & Research Centre, Patna, Bihar- 801505 India.
Received: 10 October 2023; Accepted: 18 October 2023; Published: 19 October 2023.
Citation: Yerravarapu Vamsi Krishna, Chandrajeet Kumar and Arun Kumar. Assessment of Complete Blood Count in the Breast Cancer Patients of Arsenic Exposed Population of Bihar. Journal of Cancer Science and Clinical Therapeutics 7 (2023): 186-193.
Share at FacebookAbstract
Arsenic contamination of groundwater has recently been recognized as a major threat to human health. They developed cancer after being exposed to arsenic for a long time. Among women, breast cancer is a rapidly expanding health problem in the modern era. Arsenic exposure leads to hormonal imbalance and breast cancer in the exposed population. Blood samples from n=203 breast cancer study participants and n=100 control female individuals were taken for analysis of complete blood count in this present research. The study reveals that there is significant elevation in the WBC counts and decrease in the RBC counts, platelets counts and haemoglobin percentage in the breast cancer patients. Out of n=203, female breast cancer patients, n=174 subject’s blood had significant changes in the haematological parameters in comparison to the control patient’s blood samples. Women who have been exposed to arsenic for an extended period of time in the state of Bihar have hormonal imbalances in their bodies as a result of the poisoning. In the present study, there was significant decrease (p<0.05) in the RBC counts in 92% of breast cancer patients in comparison to the control patients. Moreover, RBC indices were significantly fluctuated (p<0.05) in PCV%, MCV, MCH and MCHC levels in breast cancer patients in comparison to the control patients. The haemoglobin percentage in 94% in breast cancer patients had significant less levels (p<0.05) in comparison to the control patients. Finally, there was significant increase (p<0.05) in the WBC counts in 85% of the breast cancer patients in comparison to the control patients. This denotes that there haemotological parameters are highly affected. Moreover, these breast cancer patients were from the arsenic hotspot areas, where in the recent times the breast cancer disease burden has increased many folds. Hence, there is need to make strategies to control the disease burden in these arsenic hotspot regions.
Keywords
Breast Cancer, Complete Blood Counts, Gangetic plains.
Breast Cancer articles; Complete Blood Counts articles; Gangetic plains articles.
Breast Cancer articles Breast Cancer Research articles Breast Cancer review articles Breast Cancer PubMed articles Breast Cancer PubMed Central articles Breast Cancer 2023 articles Breast Cancer 2024 articles Breast Cancer Scopus articles Breast Cancer impact factor journals Breast Cancer Scopus journals Breast Cancer PubMed journals Breast Cancer medical journals Breast Cancer free journals Breast Cancer best journals Breast Cancer top journals Breast Cancer free medical journals Breast Cancer famous journals Breast Cancer Google Scholar indexed journals Complete Blood Counts articles Complete Blood Counts Research articles Complete Blood Counts review articles Complete Blood Counts PubMed articles Complete Blood Counts PubMed Central articles Complete Blood Counts 2023 articles Complete Blood Counts 2024 articles Complete Blood Counts Scopus articles Complete Blood Counts impact factor journals Complete Blood Counts Scopus journals Complete Blood Counts PubMed journals Complete Blood Counts medical journals Complete Blood Counts free journals Complete Blood Counts best journals Complete Blood Counts top journals Complete Blood Counts free medical journals Complete Blood Counts famous journals Complete Blood Counts Google Scholar indexed journals Gangetic plains articles Gangetic plains Research articles Gangetic plains review articles Gangetic plains PubMed articles Gangetic plains PubMed Central articles Gangetic plains 2023 articles Gangetic plains 2024 articles Gangetic plains Scopus articles Gangetic plains impact factor journals Gangetic plains Scopus journals Gangetic plains PubMed journals Gangetic plains medical journals Gangetic plains free journals Gangetic plains best journals Gangetic plains top journals Gangetic plains free medical journals Gangetic plains famous journals Gangetic plains Google Scholar indexed journals breast cancer articles breast cancer Research articles breast cancer review articles breast cancer PubMed articles breast cancer PubMed Central articles breast cancer 2023 articles breast cancer 2024 articles breast cancer Scopus articles breast cancer impact factor journals breast cancer Scopus journals breast cancer PubMed journals breast cancer medical journals breast cancer free journals breast cancer best journals breast cancer top journals breast cancer free medical journals breast cancer famous journals breast cancer Google Scholar indexed journals haematological parameters articles haematological parameters Research articles haematological parameters review articles haematological parameters PubMed articles haematological parameters PubMed Central articles haematological parameters 2023 articles haematological parameters 2024 articles haematological parameters Scopus articles haematological parameters impact factor journals haematological parameters Scopus journals haematological parameters PubMed journals haematological parameters medical journals haematological parameters free journals haematological parameters best journals haematological parameters top journals haematological parameters free medical journals haematological parameters famous journals haematological parameters Google Scholar indexed journals arsenic poisoning articles arsenic poisoning Research articles arsenic poisoning review articles arsenic poisoning PubMed articles arsenic poisoning PubMed Central articles arsenic poisoning 2023 articles arsenic poisoning 2024 articles arsenic poisoning Scopus articles arsenic poisoning impact factor journals arsenic poisoning Scopus journals arsenic poisoning PubMed journals arsenic poisoning medical journals arsenic poisoning free journals arsenic poisoning best journals arsenic poisoning top journals arsenic poisoning free medical journals arsenic poisoning famous journals arsenic poisoning Google Scholar indexed journals hormonal imbalances articles hormonal imbalances Research articles hormonal imbalances review articles hormonal imbalances PubMed articles hormonal imbalances PubMed Central articles hormonal imbalances 2023 articles hormonal imbalances 2024 articles hormonal imbalances Scopus articles hormonal imbalances impact factor journals hormonal imbalances Scopus journals hormonal imbalances PubMed journals hormonal imbalances medical journals hormonal imbalances free journals hormonal imbalances best journals hormonal imbalances top journals hormonal imbalances free medical journals hormonal imbalances famous journals hormonal imbalances Google Scholar indexed journals cancer patients articles cancer patients Research articles cancer patients review articles cancer patients PubMed articles cancer patients PubMed Central articles cancer patients 2023 articles cancer patients 2024 articles cancer patients Scopus articles cancer patients impact factor journals cancer patients Scopus journals cancer patients PubMed journals cancer patients medical journals cancer patients free journals cancer patients best journals cancer patients top journals cancer patients free medical journals cancer patients famous journals cancer patients Google Scholar indexed journals hotspot regions articles hotspot regions Research articles hotspot regions review articles hotspot regions PubMed articles hotspot regions PubMed Central articles hotspot regions 2023 articles hotspot regions 2024 articles hotspot regions Scopus articles hotspot regions impact factor journals hotspot regions Scopus journals hotspot regions PubMed journals hotspot regions medical journals hotspot regions free journals hotspot regions best journals hotspot regions top journals hotspot regions free medical journals hotspot regions famous journals hotspot regions Google Scholar indexed journals Oncology articles Oncology Research articles Oncology review articles Oncology PubMed articles Oncology PubMed Central articles Oncology 2023 articles Oncology 2024 articles Oncology Scopus articles Oncology impact factor journals Oncology Scopus journals Oncology PubMed journals Oncology medical journals Oncology free journals Oncology best journals Oncology top journals Oncology free medical journals Oncology famous journals Oncology Google Scholar indexed journals
Article Details
1. Introduction
It is estimated that about 300 million people throughout the globe are at risk of arsenic poisoning. As a result, approximately 70 million people in India are at risk. Around ten million people in the state of Bihar are now at risk of getting arsenic poisoning as a result of drinking water that has been tainted with the element. Arsenic has generated major health concerns for the people of Bihar that live in the Gangetic plains, and these dangers have been induced by arsenic. In addition to this, arsenic is often referred to as the "king of poison" or "the poison of kings." Because of the potentially lethal characteristics of the trivalent form of arsenic, it has been given a particular point of emphasis. The World Health Organization (WHO) has determined that an exposure to 10 ppb of inorganic arsenic in drinking water is the absolute highest level that can be considered safe (WHO) [1]. The United States Environmental Protection Agency (EPA) established a limit for the amount of total inorganic arsenic that may be present in drinking water at 10 ug/L (US EPA) [2]. Due to the widespread use of arsenic-tainted groundwater for agricultural irrigation, not only is drinking water becoming a significant source of arsenic exposure, but so are the crops that are used to produce food. Arsenic comes through geological processes and may be found in the alluvial silt of the Delta [3, 4]. The source of arsenic is geological. People in the tens of millions are being affected by the arsenic pollution of the groundwater in southern Asia. According to [5], in the lowlands of southern Asia, where there is a large human density, there are also hazardous levels of arsenic in the groundwater. According to the most recent estimates from 2014 by the Council for Scientific and Industrial Research (CSIR), more than 7 crore people in India are at risk of being exposed to arsenic in their drinking water. The majority of these people live in the Ganga Basin. The countries with the highest risk include Argentina, Bangladesh, Bolivia, Brazil, Chile, China, Cambodia, Ghana, Greece, Hungary, India, Japan, Korea, Mexico, Mongolia, Nepal, New Zealand, Poland, Taiwan, Vietnam, and the United States of America [6-12]. More than 10 million people in the state of Bihar are now at risk due to arsenic pollution in the groundwater [13, 14]. This contamination has been documented from 22 districts throughout the state. In 2002, the poisoning of the groundwater in Bihar caused by arsenic was first observed in the the village of Semaria Ojha Patti, which is located in the Shahpur block of the Bhojpur district [15, 16]. According to the findings of [17], groundwater arsenic pollution was found in 50 blocks across 11 districts in the state of Bihar. Recently, [18] assessed that there is an extremely significant danger to one's health in the regions of the Maner block of the Patna district that have been poisoned by arsenic. Additionally, the districts of Bhojpur, Patna, Samastipur, and Bhagalpur are the parts of Bihar that have been impacted by arsenic contamination and have levels of arsenic in their drinking water that are higher than 1000 g/L. More than fifty micrograms per liter of arsenic was found in the water in the districts of Vaishali, Saran, Begusarai, Khagaria, Munger, and Katihar [12, 19, 20-30]. In recent years, the incidence of breast cancer among women in our nation has risen to unprecedented heights. Hereditary causes, reproductive variables, hormone imbalances, women who discontinue nursing, and other lifestyle choices are all potential contributors to the development of the condition. In addition, in more recent times, it has come to be believed that environmental factors may potentially be the causal agent underlying the development of breast cancer. It's possible that the contaminants in the environment include things like pesticides, heavy metals, and metalloids like arsenic [31-35]. The Gangetic plains of Bihar have seen an exponential rise in the number of women diagnosed with breast cancer over the last few decades. Unfortuitously, reports of serious arsenic poisoning in the groundwater have also been received in this region. As a result, the purpose of the current research is to compare the patients who have breast cancer to those who do not have the disease in order to look for differences in the haematological parameters.
2. Methods and Materials
2.1 Ethical Approval:
The research project received approval from the Ethics Committee (IEC) of the Mahavir Cancer Sansthan and Research Centre on January 8, 2019, as shown by the authorized IEC No. MCS/Research/2019-2020/11. Both the breast cancer patients who were the focus of the study and the control individuals gave their permission after receiving appropriate information.
2.2 Location:
The research was conducted at our own institution, the Mahavir Cancer Sansthan and Research Centre in Patna, which is located in the state of Bihar in India. The research began in January 2019 and continued until April 2023, when it was finally finished.
2.3 Selection of the Subjects for the study:
For the purpose of the investigation, a total of n=100 control normal people were chosen for participation, and for the purpose of the investigation's cross-sectional design, n=203 patients with breast disease that had been pathologically proven were chosen to participate as the arsenic exposed group.
2.4 Collection of blood samples for the study:
After collecting about 5 milliliters of blood by volume from the peripheral vein in the patient's arm using disposable syringes, the blood was then transferred to a heparinized vacutainer in accordance with the instructions provided by IUPAC [36]. These procedures were carried out in accordance with the IUPAC. In preparation for further analysis, the blood samples were frozen at a temperature of -80 degrees centigrade.
2.5 Haematological study:
The acquired blood samples were analyzed using the standard protocols in order to determine haematological parameters such as the count of red blood cells, RBC indices level (PCV%, MCV, MCH and MCHC), haemoglobin percentage and White Blood Cells (WBC) counts.
2.6 Statistical Analysis:
All the data were analysed using the software GraphPad Prism 5.0 and the values were generated as Mean ± SEM. The data variables were also analysed statistically through one-way analysis of variance (ANOVA) by using the Dunnett’s test [37].
3. Results
Haemotological Study:
Red Blood Cell Counts (RBC): The RBC counts in control n=100 patients in less than normal levels i.e <4.5 millions/Cu.mm were in n=11 patients but the patients having RBC counts observed >4.5 millions/Cu.mm were in n=89. The RBC counts in breast cancer n=203 patients in less than normal levels i.e <4.5 millions/Cu.mm were in n=186 patients, but the patients having RBC counts observed >4.5 millions/Cu.mm were in n=17 (Figure 1).
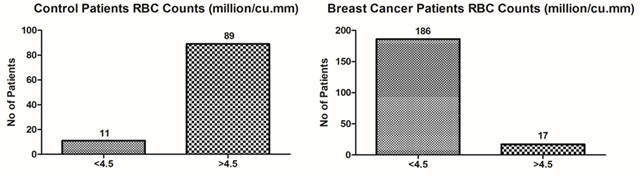
Figure 1: RBC counts of control patients versus breast cancer patients (ANOVA- Dunnett’s Test, P<0.05)
Red Blood Cell Indices: The RBC in control n=100 patients were in normal levels in PCV%, MCV, MCH and MCHC levels. But, in breast cancer n=203 patients were in n=186 patients, had fluctuated levels (Figure 2).
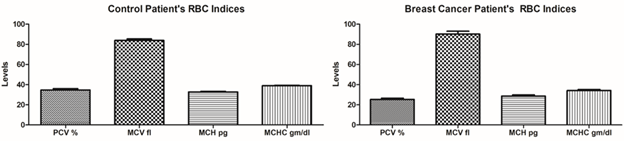
Figure 2: RBC indices levels of control patients versus breast cancer patients (ANOVA- Dunnett’s Test, P<0.05)
Haemoglobin percentage (Hb%): The haemoglobin percentage in control n=100 patients had major patients with haemoglobin in normal range. In breast cancer n=203 patients in more than 94% had their haemoglobin percentage less than normal range of 12-14 g/dL. (Figure 3).
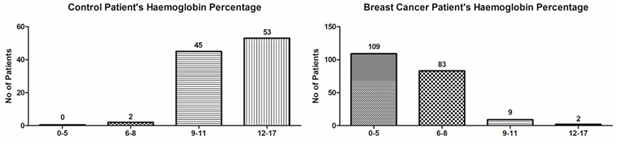
Figure 3: Haemoglobin percentage levels of control patients versus breast cancer patients (ANOVA- Dunnett’s Test, P<0.05).
White Blood Cell Counts (WBC): The WBC counts in control n=100 patients in less than normal levels i.e <11000/Cu.mm were in n=96 patients but the patients having RBC counts observed >11000/Cu.mm were in n=4. The WBC counts in breast cancer n=203 patients in less than normal levels i.e <11000/Cu.mm were in n=29 patients, but the patients having WBC counts observed <11000/Cu.mm were in n=174 (Figure 4).
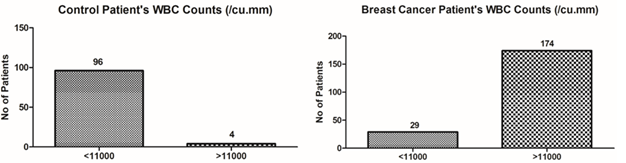
Figure 4: WBC counts of control patients versus breast cancer patients (ANOVA- Dunnett’s Test, P<0.05)
4. Discussion
In recent years, exposure to arsenic has been linked to a number of major health problems among the general population. Because arsenic mimics the estrogen hormone, which, in turn, produces hormonal imbalance in female subjects, arsenic poisoning has severe effects on female subjects. This is especially true for female subjects who are tested. Because of this, the levels of hormones including estrogen, leutenizing hormone, prolactin, and oxytocin increase. According to research published by [38-40], increased levels of prolactin are responsible for the development of breast lumps, which in turn may lead to breast cancer. Furthermore, owing to the instability of the compounds, the AsIII is more poisonous than the AsV [41-45]. In most cases, the liver and kidneys are the metabolic organs responsible for the removal of the arsenic from the body. In the present study, there was significant decrease (p<0.05) in the RBC counts in 92% of breast cancer patients in comparison to the control patients. Moreover, RBC indices were significantly fluctuated (p<0.05) in PCV%, MCV, MCH and MCHC levels in breast cancer patients in comparison to the control patients. The haemoglobin percentage in 94% in breast cancer patients had significant less levels (p<0.05) in comparison to the control patients. Finally, there was significant increase (p<0.05) in the WBC counts in 85% of the breast cancer patients in comparison to the control patients. This denotes that there haemotological parameters are highly affected. Moreover, these breast cancer patients were from the arsenic hotspot areas, where in the recent times the breast cancer disease burden has increased many folds. Various studies have correlated the significant association between the arsenic with cancer risk [46-48]. According to the International Agency for Research on Cancer (IARC), the Environmental Protection Agency (EPA), and the World Health Organization (WHO), arsenic is a category I carcinogen that may cause cancer of the gallbladder, skin, lung, kidney, bladder, and colorectal cancer [48-50]. Poisoning from arsenic brought on by chronic exposure causes signaling pathways to become dysregulated, which in turn leads to the development of breast cancer. Incorrect signaling plays a role in the gene transformations that lead to severe mutations caused by arsenic poisoning. These gene transformations include BCL-2, PTEN, MLH, MMP-2, and Bax. [44, 47, 51-61]. In the state of Bihar, in the arsenic hotspot regions, the exposed population are consuming arsenic contaminated water for very long time. This long-term exposure causes lowering down of their immunity as arsenic directly hits the bone marrow cells which in turn causes lowering down of the immunity due to the decrease in the WBC levels. Moreover, these levels are much lower in the breast cancer patients who are from these arsenic hotspot regions. Similarly, the other haemotological parameters such as RBC counts, haemoglobin percentage and RBC indices such as PCV%, MCV, MCH and MCHC levels are hampered in the breast cancer patients in comparison to the control patients. Hence, the first line of defense is breached in these patients due to arsenic exposure which in long-term causes serious implications in them. Similar studies, have been reported by various researchers [62-75]
Conclusions
The present study, demonstrates the significant fluctuation in the haemotological parameters in breast cancer patients from the arsenic hotspot regions in comparison to the control. The basic cause for the changes is due to the accidental arsenic exposure to the patients for very long term, which lowers down their immunity causing invitation to various diseases. Breast cancer disease has been found to be in very high number from these arsenic hotspot regions where unfortunately their immunity has significantly lowered down in comparison to the control group. Hence, there is need to make strategies to control the disease burden in these arsenic hotspot regions.
Acknowledgement:
The authors are thankful to YBN University and Mahavir Cancer Sansthan and Research Centre (MCSRC) for providing all necessary infrastructures required for this study. The financial assistance for the study was provided by the University itself.
Author contributions:
Yerravarapu Vamsi Krishna, Chandrajeet Kumar and Arun Kumar conceptualized the entire work. Yerravarapu Vamsi Krishna is the principal author and had the major contributions in writing the manuscript but support was also provided by Arun Kumar and Chandrajeet Kumar, literature search was done by Yerravarapu Vamsi Krishna, experimental work and data analysis was done by Yerravarapu Vamsi Krishna and Arun Kumar, final data interpretation was done by Yerravarapu Vamsi Krishna, Chandrajeet Kumar and Arun Kumar. All authors read and approved the final manuscript.
Funding:
Funding information is not applicable as there was no funding for this project.
Data availability:
The data that support the findings of this study is available from the corresponding author upon reasonable request.
References
- Exposure to arsenic: A major public health concern, In: Preventing disease through healthy environments (2010): 1-5.
- US EPA. Guidance for evaluating the oral bioavailability of metals in soils for use in human health risk assessment. OSWER 9285 (2007): 7-80.
- Mukherjee A, Sengupta MK, Hossain MA, et al. Arsenic Contamination in Groundwater: A Global Perspective with Emphasis on the Asian Scenario. J Health Popul Nutr 24 (2006): 142-163
- Chakraborti D, Singh SK, Rahman MM, et al. Groundwater Arsenic Contamination in the Ganga River Basin: A Future Health Danger. Int J Environ Res Public Health 15 (2018): 180.
- Benner S. Arsenic occurs naturally in the groundwater of southern Asia. Analyses of an agricultural site in Bangladesh suggest that human activities, including widespread farming practices, can dictate where elevated arsenic is found. Nature Geoscience 3 (2010): 5-6.
- Smedley PL and Kinniburgh DG. A review of the source, behavior and distribution of arsenic in natural waters. Applied Geochemistry 17 (2002): 517-568.
- Bibi MH, Ahmed F and Ishiga H. Geochemical study of arsenic concentrations in groundwater of the Meghna River Delta, Bangladesh. Journal of Geochemical Exploration 97 (2008): 43-58.
- Ravenscroft P, Brammer H and Richards KS. Arsenic pollution: A global synthesis. UK (2009).
- Bundschuh J, Litter M and Bhattacharya P. Targeting arsenic-safe aquifers for drinking water supplies. Environmental Geochem Health 32 (2010): 307-315.
- Casentini B, Hug SJ and Nikolaidis NP. Arsenic accumulation in irrigated agricultural soils in Northern Greece. The Science of the Total Environment 409 (2011): 4802-4810.
- Thakur JK, Thakur RK, Ramanathan AL.et al. Arsenic contamination of groundwater in Nepal-An overview. Water 3 (2011): 1-20.
- Sahoo, P. K. and Kim, K. 2013 A review of the arsenic concentration in paddy rice from the perspective of geoscience. Geosciences Journal. 17(1): 107-122.
- Saha D. Arsenic groundwater contamination in parts of middle Ganga plain, Bihar. Current Science 97 (2009): 753-755.
- School of Environmental Studies, Groundwater arsenic contamination in middle Ganga plain, Bihar, India: A Future Danger? School of Environmental Science, Jadavpur University, Kolkata, India (2012).
- Chakraborti D, Mukherjee SC, Pati S, et al. Arsenic groundwater contamination in Middle Ganga Plain, Bihar, India: a future danger?. Environmental health perspectives 111 (2003): 1194-1201.
- Chakraborti D, Sengupta MK, Rahman MM, et al. Groundwater arsenic contamination and its health effects in the Ganga-Meghna-Brahmaputra plain. Journal of environmental monitoring : JEM 6 (2004): 74-83.
- Nickson R, Sengupta C, Mitra P, et al. 2007 Current Knowledge on the Distribution of Arsenic in Groundwater in Five States of India. Journal of Environmental Science and Health. Part A 42(2007): 1707-1718.
- Singh SK and Ghosh AK. Health Risk Assessment due to Groundwater Arsenic Contamination: Children are at High Risk, Human and Ecological Risk Assessment. An International Journal 18 (2012): 751-766.
- Singh SK, Ghosh AK, Kumar A, et al. Groundwater Arsenic Contamination and Associated Health Risks in Bihar, India. International Journal of Environmental Research 8 (2014): 49-60.
- Kumar A, Ali M, Rahman SM, et al. Ground water arsenic poisoning in “Tilak Rai Ka Hatta” village of Buxar district, Bihar, India causing severe health hazards and hormonal imbalance. J Environ Anal Toxicol 5 (2015): 1-7.
- Kumar A, Rahman MS, Iqubal A, et al. Ground Water Arsenic Contamination: A Local Survey in India. International journal of preventive medicine, 7 (2016): 100.
- Kumar A, Ali M, Kumar R, et al. Arsenic exposure in Indo Gangetic plains of Bihar causing increased cancer risk. Scientific reports 11 (2021a): 2376.
- Kumar A, Kumar R, Rahman MS, et al. Assessment of arsenic exposure in the population of Sabalpur village of Saran District of Bihar with mitigation approach. Environmental science and pollution research international, 28 (2021b): 43923-43934.
- Kumar A, Rahman MS, Ali M, et al. Assessment of arsenic exposure and its mitigation intervention in severely exposed population of Buxar district of Bihar, India. Toxicol. Environ. Health Sci (2021c).
- Kumar A, Ghosh AK. Assessment of arsenic contamination in groundwater and affected population of Bihar. N. Kumar (ed.), Arsenic Toxicity: Challenges and Solutions (2021d).
- Kumar A, Rahman MS, Ali M, et al. Assessment of disease burden in the arsenic exposed population of Chapar village of Samastipur district, Bihar, India, and related mitigation initiative. Environmental science and pollution research international 29 (2022a): 27443-27459.
- Kumar A, Ravi C, Dhingra S, et al. Arsenic Causing Gallbladder Cancer Disease near the Himalayan bound Rivers in Bihar: A Case study of Gallbladder Cancer. Journal of Cancer Science and Clinical Therapeutics 6 (2022b): 388-391.
- Goyal A, Sahu RK, Kumar M, et al. p16 promoter methylation, expression, and its association with estrogen receptor, progesterone receptor, and human epidermal growth factor receptor 2 subtype of breast carcinoma. J Can Res Ther 15 (2019): 1147-54.
- Kumar A and Ghosh AK. Arsenic and Cancer. In Environmental Exposures and Human Health Challenges (2019a): 106-132.
- Kumar A, Rahman MS, Kumar R, et al. Arsenic contamination in groundwater causing impaired memory and intelligence in school children of Simri village of Buxar district of Bihar. J Mental Health Hum Behav 24 (2019b): 132-138.
- Calaf GM. Role of organophosphorous pesticides and acetylcholine in breast carcinogenesis. Seminars in cancer biology 76 (2021): 206-217.
- Rocha PRS, Oliveira VD, Vasques CI, et al. Exposure to endocrine disruptors and risk of breast cancer: A systematic review. Critical reviews in oncology/hematology 161 (2021): 103330.
- Ledda C, Bracci M, Lovreglio P, et al. Pesticide exposure and gender discrepancy in breast cancer. European review for medical and pharmacological sciences 25 (2021): 2898-2915.
- Paydar P, Asadikaram G, Fallah H, et al. Serum levels of Organochlorine Pesticides and Breast Cancer Risk in Iranian Women. Archives of environmental contamination and toxicology 77 (2019): 480-489.
- Girard L, Reix N & Mathelin C. Impact des pesticides perturbateurs endocriniens sur le cancer du sein [Impact of endocrine disrupting pesticides on breast cancer]. Gynecologie, obstetrique, fertilite & senologie 48 (2020): 187-195.
- Cornelis R, Heinzow B, Herber RF, et al. Sample collection guidelines for trace elements in blood and urine (technical report). Pure Appl Chem 67 (1995): 1575-1608.
- Sanz E, Muñoz-Olivas R, Cámara C, et al. Arsenic speciation in rice, straw, soil, hair and nails samples from the arsenic-affected areas of Middle and Lower Ganga plain. J Environ Sci Health A Toxicol Hazard Subst Environ Eng 42 (2007): 1695-1705.
- Kortenkamp A. Are cadmium and other heavy metal compounds acting as endocrine disrupters?. Met Ions Life Sci 8 (2011): 305-317.
- Davey JC, Bodwell JE, Gosse JA, et al. Arsenic as an endocrine disruptor: effects of arsenic on estrogen receptor-mediated gene expression in vivo and in cell culture. Toxicol Sci 98 (2007): 75-86.
- Davey JC, Nomikos AP, Wungjiranirun M, et al. Arsenic as an endocrine disruptor: arsenic disrupts retinoic acid receptor-and thyroid hormone receptor-mediated gene regulation and thyroid hormone-mediated amphibian tail metamorphosis. Environmental health perspectives 116 (2008): 165-172.
- Michel-Ramirez G, Recio-Vega R, Lantz RC, et al. Assessment of YAP gene polymorphisms and arsenic interaction in Mexican women with breast cancer. J Appl Toxicol 40 (2020): 342-351.
- Soh MA, Garrett SH, Somji S, et al. Arsenic, cadmium and neuron specific enolase (ENO2, γ-enolase) expression in breast cancer. Cancer Cell Int 11 (2011): 41.
- Lopez-Carrillo L, Hernandez-Ramirez RU, Gandolfi AJ, et al. Arsenic methylation capacity is associated with breast cancer in northern Mexico. Toxicol Appl Pharmacol 280 (2014): 53-59.
- Gamboa-Loira B, Cebrian ME, Salinas-Rodriguez A, et al. Genetic susceptibility to breast cancer risk associated with inorganic arsenic exposure. Environ Toxicol Pharmacol 5 (2017): 106-113.
- Kuo CC, Moon KA, Wang SL, et al. The Association of Arsenic Metabolism with Cancer, Cardiovascular Disease, and Diabetes: A Systematic Review of the Epidemiological Evidence. Environ Health Perspect 125 (2017): 087001.
- Krishna YV, Kumar C and Kumar A. Blood Arsenic Contamination Causing Breast Cancer Risk in Exposed Population of Bihar. Health Science Journal 17 (2023): 1-6.
- Marciniak W, Derkacz R, Muszy?ska M, et al. Blood arsenic levels and the risk of familial breast cancer in Poland. Int J Cancer 146 (2020): 2721-2727.
- Kumar A, Ali M, Raj V, et al. Arsenic causing gallbladder cancer disease in Bihar. Scientific reports 13 (2023a): 4259.
- Palma-Lara P I, Martínez-Castillo M, Quintana-Pérez JC, et al. Arsenic exposure: A public health problem leading to several cancers. Regul Toxicol Pharmacol 110 (2020): 104539.
- Cuzick J. Preventive therapy for cancer. Lancet Oncol 18 (2017): 472-482.
- Joo NS, Kim SM, Jung YS, et al. Hair iron and other minerals’ level in breast cancer patients. Biol Trace Elem Res 129 (2009): 28-35.
- Wadhwa SK, Kazi TG, Afridi HI, et al. Interaction between carcinogenic and anti-carcinogenic trace elements in the scalp hair samples of different types of Pakistani female cancer patients. Clin Chim Acta 439 (2015): 178-84.
- Nielsen FC, van Overeem Hansen T, et al. Hereditary breast and ovarian cancer: new genes in confined pathways. Nat Rev Cancer 16 (2016): 599-612.
- Easton DF, Pharoah PD, Antoniou AC, et al. Gene-panel sequencing and the prediction of breast-cancer risk. N Engl J Med 372 (2015): 2243-2257.
- Selmin OI, Donovan MG, Skovan B, et al. Arsenic induced BRCA1 CpG promoter methylation is associated with the downregulation of ERα and resistance to tamoxifen in MCF7 breast cancer cells and mouse mammary tumor xenografts. Int J Oncol 54 (2019): 869-878.
- Foster H, Kennedy G, Maisonneuve P, et al. A case-control study of toenail selenium, mercury, arsenic and cadmium and cancer of the breast, colon and prostate in Montreal. Trends Cancer Res 4 (2008): 15-18.
- Pineda-Belmontes CP, Hernández-Ramírez RU, Hernández-Alcaraz C, et al. Genetic polymorphisms of PPAR gamma, arsenic methylation capacity and breast cancer risk in Mexican women. Salud Publica Mex 58 (2016): 220-227.
- Blaurock-Busch E, Busch YM, Friedle A, et al. Comparing the metal concentration in the hair of cancer patients and healthy people living in the Malwa region of Punjab, India. Clin Med Insights Oncol 8 (2014): 1-13.
- Benderli Cihan Y, Sozen S, Ozturk Yildirim S. Trace elements and heavy metals in hair of stage III breast cancer patients. Biol Trace Elem Res 144 (2011): 360-379.
- Garland M, Morris JS, Colditz GA, et al. Toenail trace element levels and breast cancer: a prospective study. Am J Epidemiol 144 (1996): 653-660.
- Alatise OI, Schrauzer GN. Lead exposure: a contributing cause of the current breast cancer epidemic in Nigerian women. Biol Trace Elem Res 136 (2010): 127-139.
- Divsalar B, Heydari P, Habibollah G, et al. Hematological Parameters Changes in Patients with Breast Cancer. Clinical laboratory 67 (2021).
- Kumar A, Kumar K, Ali M, et al. Severe Disease Burden and the Mitigation Strategy in the Arsenic-Exposed Population of Kaliprasad Village in Bhagalpur District of Bihar, India. Biological trace element research (2023b).
- Reichard JF, Puga A. Effects of arsenic exposure on DNA methylation and epigenetic gene regulation. Epigenomics 2 (2010): 87-104.
- Martinez VD, Vucic EA, Becker-Santos DD, et al. Arsenic exposure and the induction of human cancers. J Toxicol (2011): 431287.
- Ren X, McHale CM, Skibola CF, et al. An emerging role for epigenetic dysregulation in arsenic toxicity and carcinogenesis. Environ Health Perspect 119 (2011): 11-19.
- Zhao CQ, Young MR, Diwan BA, et al. Association of arsenic-induced malignant transformation with DNA hypomethylation and aberrant gene expression. Proceedings of the National Academy of Sciences of the United States of America 94 (1997): 10907-10912.
- Mass MJ, Wang L. Arsenic alters cytosine methylation patterns of the promoter of the tumor suppressor gene p53 in human lung cells: a model for a mechanism of carcinogenesis. Mutat Res 386 (1997): 263-277.
- Cui X, Wakai T, Shirai Y, et al. Chronic oral exposure to inorganic arsenate interferes with methylation status of p16INK4a and RASSF1A and induces lung cancer in A/J mice. Toxicol Sci 91 (2006): 372-381.
- Marsit CJ, Karagas MR, Schned A, et al. Carcinogen exposure and epigenetic silencing in bladder cancer. Ann N Y Acad Sci 1076 (2006): 810-821.
- Chanda S, Dasgupta UB, Guhamazumder D, et al. DNA hypermethylation of promoter of gene p53 and p16 in arsenic-exposed people with and without malignancy. Toxicol Sci 89 (2006): 431-437.
- Zimta AA, Schitcu V, Gurzau E, et al. Biological and molecular modifications induced by cadmium and arsenic during breast and prostate cancer development. Environ Res 178 (2019): 108700.
- Dantzig PI. Breast cancer, dermatofibromas and arsenic. Indian J Dermatol 54 (2009): 23-25.
- Danes JM, de Abreu ALP, Kerketta R, et al. Inorganic arsenic promotes luminal to basal transition and metastasis of breast cancer. FASEB J 34 (2020): 16034-48.
- Pullella J, Kotsopoulos K J. Arsenic Exposure and Breast Cancer Risk: A Re-Evaluation of the Literature. Nutrients 12 (2020): 3305.
