Acute Transient Dyspnea in Arterial Gadoxetate-Enhanced Liver Magnetic Resonance Imaging: Depends on Arterial Phase Timing and Potential Risk Factors
Article Information
Kromrey ML1, Schorn F1, Liedtke KR2, Ittermann T3, Plodeck V4, Kühn JP1,4
1Department of Diagnostic Radiology and Neuroradiology, University Medicine Greifswald, Greifswald, Germany
2Department of General, Visceral, Thoracic and Vascular Surgery, University Medicine Greifswald, Greifswald, Germany
3Institute for Community Medicine, University Medicine Greifswald, Greifswald, Germany
4Department of Radiology, University Hospital Carl Gustav Carus Dresden, Dresden, Germany
*Corresponding Author: Marie-Luise Kromrey, Department of Radiology and Neuroradiology, University Medicine Greifswald, Ferdinand-Sauerbruch-Straße, Greifswald, D-17475; Germany
Received: 06 September 2019; Accepted: 15 September 2019; Published: 19 September 2019;
Citation: Kromrey ML, Schorn F, Liedtke KR, Ittermann T, Plodeck V, Kühn JP. Acute Transient Dyspnea in Arterial Gadoxetate-Enhanced Liver Magnetic Resonance Imaging: Depends on Arterial Phase Timing and Potential Risk Factors. Journal of Radiology and Clinical Imaging 2 (2019): 045-054.
Share at FacebookAbstract
Purpose: To investigate the frequency, influence of arterial phase timing and risk factors for TSM artifacts in arterial phase of gadoxetate-enhanced MRI of the liver.
Materials and Methods: Between 2013-2016, gadoxetate-enhanced liver MRI of 354 patients (196 men, 158 women, mean age 60.8±14.2 years) were retrospectively enrolled. Sixty-nine patients received follow-up. Arterial phase images were evaluated regarding motion artifacts on a four-point scale (0 = no motion artifacts, 1 = minor artifacts, 2 = distinct artifacts, 3 = severe artifacts/non-diagnostic). Occurrence and artifact grading were correlated with arterial phase timing (early, true and late arterial phase), previous TSM and selected risk factors such as patients’ demographics, behaviors and laboratory data.
Results: TSM artifacts occurred in 48.6% (172/354) of the patients. 25.7% (91/354) had distinct (18.4%) or severe (7.3%) image artifacts. Significantly higher incidence of TSM was detected in the true arterial phase (58.8%) compared to early (51.6%) or late arterial phase (42.1%) (p=0.031). Severe artifacts were mainly seen in the true arterial phase (42.3%). Occurrence of TSM was correlated with BMI (p=0.001). Longitudinal analysis showed significant association between TSM at baseline and follow-up (p=0.041).
Conclusion: Severity of TSM in gadoxetic-enhanced MRI is influenced by arterial phase timing, more common in the true arterial phase compared to early or late arterial phases, and is associated with BMI and prior TSM occurrence.
Keywords
Acute transient dyspnea; Transient severe motion artifact; Magnetic resonance imaging; Gadoxetate
Acute transient dyspnea articles, Transient severe motion artifact articles, Magnetic resonance imaging articles, Gadoxetate articles
Acute transient dyspnea articles Acute transient dyspnea Research articles Acute transient dyspnea review articles Acute transient dyspnea PubMed articles Acute transient dyspnea PubMed Central articles Acute transient dyspnea 2023 articles Acute transient dyspnea 2024 articles Acute transient dyspnea Scopus articles Acute transient dyspnea impact factor journals Acute transient dyspnea Scopus journals Acute transient dyspnea PubMed journals Acute transient dyspnea medical journals Acute transient dyspnea free journals Acute transient dyspnea best journals Acute transient dyspnea top journals Acute transient dyspnea free medical journals Acute transient dyspnea famous journals Acute transient dyspnea Google Scholar indexed journals Transient severe motion artifact articles Transient severe motion artifact Research articles Transient severe motion artifact review articles Transient severe motion artifact PubMed articles Transient severe motion artifact PubMed Central articles Transient severe motion artifact 2023 articles Transient severe motion artifact 2024 articles Transient severe motion artifact Scopus articles Transient severe motion artifact impact factor journals Transient severe motion artifact Scopus journals Transient severe motion artifact PubMed journals Transient severe motion artifact medical journals Transient severe motion artifact free journals Transient severe motion artifact best journals Transient severe motion artifact top journals Transient severe motion artifact free medical journals Transient severe motion artifact famous journals Transient severe motion artifact Google Scholar indexed journals Magnetic resonance imaging articles Magnetic resonance imaging Research articles Magnetic resonance imaging review articles Magnetic resonance imaging PubMed articles Magnetic resonance imaging PubMed Central articles Magnetic resonance imaging 2023 articles Magnetic resonance imaging 2024 articles Magnetic resonance imaging Scopus articles Magnetic resonance imaging impact factor journals Magnetic resonance imaging Scopus journals Magnetic resonance imaging PubMed journals Magnetic resonance imaging medical journals Magnetic resonance imaging free journals Magnetic resonance imaging best journals Magnetic resonance imaging top journals Magnetic resonance imaging free medical journals Magnetic resonance imaging famous journals Magnetic resonance imaging Google Scholar indexed journals Gadoxetate articles Gadoxetate Research articles Gadoxetate review articles Gadoxetate PubMed articles Gadoxetate PubMed Central articles Gadoxetate 2023 articles Gadoxetate 2024 articles Gadoxetate Scopus articles Gadoxetate impact factor journals Gadoxetate Scopus journals Gadoxetate PubMed journals Gadoxetate medical journals Gadoxetate free journals Gadoxetate best journals Gadoxetate top journals Gadoxetate free medical journals Gadoxetate famous journals Gadoxetate Google Scholar indexed journals transient severe motion articles transient severe motion Research articles transient severe motion review articles transient severe motion PubMed articles transient severe motion PubMed Central articles transient severe motion 2023 articles transient severe motion 2024 articles transient severe motion Scopus articles transient severe motion impact factor journals transient severe motion Scopus journals transient severe motion PubMed journals transient severe motion medical journals transient severe motion free journals transient severe motion best journals transient severe motion top journals transient severe motion free medical journals transient severe motion famous journals transient severe motion Google Scholar indexed journals chronic obstructive pulmonary disease articles chronic obstructive pulmonary disease Research articles chronic obstructive pulmonary disease review articles chronic obstructive pulmonary disease PubMed articles chronic obstructive pulmonary disease PubMed Central articles chronic obstructive pulmonary disease 2023 articles chronic obstructive pulmonary disease 2024 articles chronic obstructive pulmonary disease Scopus articles chronic obstructive pulmonary disease impact factor journals chronic obstructive pulmonary disease Scopus journals chronic obstructive pulmonary disease PubMed journals chronic obstructive pulmonary disease medical journals chronic obstructive pulmonary disease free journals chronic obstructive pulmonary disease best journals chronic obstructive pulmonary disease top journals chronic obstructive pulmonary disease free medical journals chronic obstructive pulmonary disease famous journals chronic obstructive pulmonary disease Google Scholar indexed journals region-of-interest articles region-of-interest Research articles region-of-interest review articles region-of-interest PubMed articles region-of-interest PubMed Central articles region-of-interest 2023 articles region-of-interest 2024 articles region-of-interest Scopus articles region-of-interest impact factor journals region-of-interest Scopus journals region-of-interest PubMed journals region-of-interest medical journals region-of-interest free journals region-of-interest best journals region-of-interest top journals region-of-interest free medical journals region-of-interest famous journals region-of-interest Google Scholar indexed journals activated partial thromboplastin time articles activated partial thromboplastin time Research articles activated partial thromboplastin time review articles activated partial thromboplastin time PubMed articles activated partial thromboplastin time PubMed Central articles activated partial thromboplastin time 2023 articles activated partial thromboplastin time 2024 articles activated partial thromboplastin time Scopus articles activated partial thromboplastin time impact factor journals activated partial thromboplastin time Scopus journals activated partial thromboplastin time PubMed journals activated partial thromboplastin time medical journals activated partial thromboplastin time free journals activated partial thromboplastin time best journals activated partial thromboplastin time top journals activated partial thromboplastin time free medical journals activated partial thromboplastin time famous journals activated partial thromboplastin time Google Scholar indexed journals glomerulary filtration rate articles glomerulary filtration rate Research articles glomerulary filtration rate review articles glomerulary filtration rate PubMed articles glomerulary filtration rate PubMed Central articles glomerulary filtration rate 2023 articles glomerulary filtration rate 2024 articles glomerulary filtration rate Scopus articles glomerulary filtration rate impact factor journals glomerulary filtration rate Scopus journals glomerulary filtration rate PubMed journals glomerulary filtration rate medical journals glomerulary filtration rate free journals glomerulary filtration rate best journals glomerulary filtration rate top journals glomerulary filtration rate free medical journals glomerulary filtration rate famous journals glomerulary filtration rate Google Scholar indexed journals alanine aminotransferase articles alanine aminotransferase Research articles alanine aminotransferase review articles alanine aminotransferase PubMed articles alanine aminotransferase PubMed Central articles alanine aminotransferase 2023 articles alanine aminotransferase 2024 articles alanine aminotransferase Scopus articles alanine aminotransferase impact factor journals alanine aminotransferase Scopus journals alanine aminotransferase PubMed journals alanine aminotransferase medical journals alanine aminotransferase free journals alanine aminotransferase best journals alanine aminotransferase top journals alanine aminotransferase free medical journals alanine aminotransferase famous journals alanine aminotransferase Google Scholar indexed journals
Article Details
1. Introduction
Contrast-enhanced magnetic resonance imaging (MRI) is a clinically established imaging modality for visualizing and characterizing focal lesions in the liver [1-4]. Especially gadoxetate disodium (Primovist®, Eovist®, Bayer-Schering Healthcare), a gadolinium-based hepatobiliary contrast agent, has proven to be of very high diagnostic value to assess hepatobiliary diseases since its approval [4-8].
However, according to recent studies intravenous bolus injection of gadoxetate disodium is also associated with the occurrence of acute transient dyspnea accompanied by transient severe motion (TSM) artifacts in the arterial phase [9,10]. This phenomenon is experienced by patients as temporary and self-limited (or “transient”) and does not occur after the hepatic arterial phase. As, however, the arterial phase is essential for the characterization of focal lesions [11], TSM leads to image degradation and reduced diagnostic accuracy and therefore proves to be of high clinical importance. Compared to the application of the alternative contrast agent gadobenate dimeglumine, the incidence of TSM in patients receiving gadoxetate disodium was found to be significantly higher with 11-22% vs 0.5-2% [9,10,12]. The underlying mechanism, however, is not yet solved.
Until now, the incidence of TSM has been linked to chronic obstructive pulmonary disease (COPD), volume of gadoxetate administration, body mass index, male sex and prior episode of arterial phase motion in MR examination [7,9,10,12-14]. However, at this time the causation of TSM after administration of gadoxetate disodium is not yet definitely clarified. In our opinion, acute transient dyspnea in gadoxetate-enhanced liver MRI as a reason for motion artifacts is of high clinical importance, since image degradation could impair diagnostic quality. Therefore, the purpose of our study was to investigate the influence of image acquisition parameters, such as arterial phase timing and patient characteristics on the frequency and severity of TSM.
2. Materials and Methods
The retrospective study was approved by the local ethics committee of the XXX (BB 113/16). The requirement to obtain informed consent of the participants was waived. Data were assessed anonymously.
2.1 Study Population
The electronic database of the XXX was searched for abdominal MR examinations under administration of gadoxetate disodium between January 1st, 2013 and June 30th, 2016. In the case that the electronic database revealed previous examinations outside the set time interval (dating back to February 2008), these were also included into primary image acquisition. This revealed 738 consecutively performed examinations in 422 patients. MR examinations were undertaken at three different MR scanners of our hospital. For comparability reasons, only those 386 patients who received imaging at Magnetom Aera (Siemens HealthCare, Erlangen, Germany) were included in the study (669 examinations). Furthermore, 163 examinations in 32 patients had to be excluded because of non-interpretability. This included imaging artifacts other than TSM (e.g. magnetic artifacts caused by foreign material, ringing artifacts, moving artifacts caused by incompliance). From the 3rd follow-up examination on, additional MR examinations in one patient were suspended from the study – this encompassed 83 examinations.
The final study population consisted of 354 patients (196 men, 158 women, mean age 60.8 ± 14.2 years at first imaging within the time interval) with 423 examinations, from which 69 patients (44 men, 25 women, mean age 60.6 ± 12.5 years) received two consecutive MR examinations. An overview of the study design is presented in a flow chart (Figure 1).
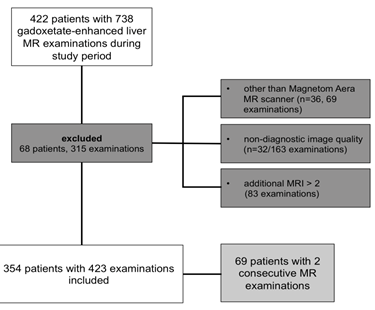
Figure 1: Study flow chart.
2.2 Magnetic resonance imaging acquisition
MR examinations of included patients were performed using a 1.5 Tesla Magnetom Aera (Siemens HealthCare, Erlangen, Germany) with a 280 mT/m gradient using body coils with 16 channels. Pre-contrast and dynamic phases were acquired each during breath-hold. Breath-holding instructions were given by verbal command from the technologist at the end of exspiration without hyperventilation. Gadoxetate disodium (Primovist®, Bayer-Schering Healthcare, Berlin, Germany) was administered intravenously as per clinical routine with an undiluted dose of 10 ml, followed by 20 ml saline both injected per hand, followed by image acquisition at fixed delays (arterial phase approximately after 20 sec, portal venous phase after 60 sec and venous phase after 120 sec).
Dynamic MRI was performed using T1-weighted gradient-echo sequences (Volume Interpolated Breath-hold Examination, VIBE). The VIBE sequences comprised the following imaging parameters: TR = 3.84 ms, TE = 1.57 ms, flip angle: 10°, bandwidth: 450 Hz/pixel, field of view: 320 mm, slice thickness = 3 mm. The complete sequence was acquired in 19 seconds.
2.3 Image analysis
2.3.1 Definition of TSM: Image analyses of pre-contrast and dynamic post-contrast (arterial, venous and hepatobiliary phase) T1-weighted sequences were performed using PACS (Picture Archiving Communication System). Acute transient dyspnea was defined as motion artifacts exclusively detected in the arterial phase. Two observers with one year of experience in abdominal MR imaging independently reviewed all examinations and were blinded to non-imaging based patient risk factors.
Image evaluation concerning TSM and diagnostic validity was undertaken by applying a 4-point scoring system: 0 = no motion artifacts, 1 = minor motion artifacts, no effect on diagnostic quality, 2 = distinct artifacts, impeded diagnostic quality, 3 = severe artifacts, non-diagnostic. Figure 2 shows examples of the different motion scores in the arterial phase of MR imaging. In the case of diverging motion scores, the two readers together reevaluated the corresponding data sets and obtained agreement. These values were used for further calculations.
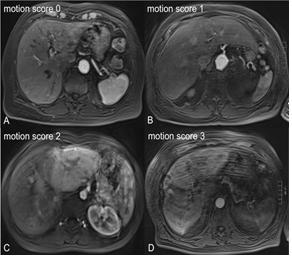
Figure 2: Categorization of motion artifacts caused by acute transient dyspnea in MR imaging. Axial T1-weighted transverse gradient-echo MR images directly following intravenous gadoxetate application exclusively seen in arterial phases show motion score 0 (A), 1 (B), 2 (C) and 3 (D), respectively. Diagnostic image quality is reduced especially in figures C and D.
2.3.2 Influence of arterial phase timing: In addition, both observers quantitatively determined signal intensity of the aorta and portal vein in pre-contrast and post-contrast arterial and portal venous phase for each patient by placing a region-of-interest (ROI). Data were averaged across the two readers to produce a mean signal intensity value (SI) and normalization with native phase was undertaken to obtain mean enhancement (ME = (SIarterial phase resp. portal venous phase - SInative)/SInative).
Furthermore, on the basis of contrast agent flow measurements within the aorta and portal vein, the arterial phase was classified into three states, for which the median was used as cut off (aorta median = MEAorta 4.647, portal vein median = MEPV 1.308). Early arterial phase was defined as low contrast enhancement in the aorta and no contrast material in the portal vein or parenchyma (MEAorta < aorta median, MEPV < portal vein median), true arterial phase as high contrast enhancement in the aorta and low enhancement in portal vein or early parenchymal enhancement without strong parenchymal or hepatic venous enhancement (MEAorta > aorta median, MEPV < portal vein median) and late arterial phase as enhancement of hepatic veins (MEPV > portal vein median). Arterial phases were then compared with TSM graduation.
2.3.3 Clinical Correlates: For correlation analysis, demographics of the patients and potential risk factors for acute transient dyspnea were derived from a query of the institutional medical record and are depicted in Table 1. These patient characteristics include age, gender, positive history of allergies (general and specific against contrast agent or iodine), smoking status, concomitant diseases (chronic obstructive pulmonary disease (COPD), asthma, liver cirrhosis, hepatic encephalopathy, cholestasis, ascites, pleural effusion, anaemia), Body-Mass-Index (BMI), and laboratory parameters for blood clotting (Quick’s value, international normalized ratio (INR), activated partial thromboplastin time (aPTT)), liver function (albumin, bilirubin, alanine aminotransferase (ALAT), aspartate aminotransferase (ASAT), gamma GT) and renal function (creatinine, glomerulary filtration rate (GFR)). Ascites as variable was assessed by reviewing the MR images.
|
Risk factor |
p-value |
|
age |
0.832 |
|
gender |
0.183 |
|
history of allergies general |
0.215 |
|
history of allergies specific (contrast agent/iodine) |
0.217 |
|
smoking status |
0.821 |
|
COPD |
0.426 |
|
asthma |
0.423 |
|
liver cirrhosis |
0.050 |
|
hepatic encephalopathy |
0.169 |
|
cholestasis |
0.447 |
|
ascites |
0.138 |
|
pleural effusion |
0.082 |
|
anaemia |
0.417 |
|
BMI (kg/m2) |
0.001 |
|
Quick’s value (>130%) |
0.497 |
|
INR |
0.448 |
|
aPTT (<20 sec) |
0.783 |
|
albumin (g/l) |
0.360 |
|
bilirubin (mmol/l) |
0.431 |
|
ALAT (mkatal/l) |
0.910 |
|
ASAT (mkatal/l) |
0.962 |
|
gGT (mkatal/l) |
0.095 |
|
creatinine (mmol/l) |
0.120 |
|
GFR |
0.618 |
Table 1: Risk factors of the study population and p-values.
2.4 Statistics
All descriptive data were described as absolute numbers and percentages (categorical variables) or as means and standard deviation (continuous variables). Associations of occurrence and severity of transient motion artifacts with arterial phase timing were analyzed by multinomial logistic regression adjusted for body mass index and ascites occurrence. Correlations between patient characteristics and the occurrence of transient severe motion artifacts were performed by Chi-Square tests for categorical risk factors and by Wilcoxon tests for continuous variables. A p-value < 0.05 was considered statistically significant. All analyses were performed using Stata 14.1 (Stata Corporation, College Station, TX, USA).
To evaluate the quality of our data, interobserver reliability was calculated by using kappa statistics. Hereby, a value below 0.20 defines disagreement, 0.20-0.40 poor agreement, 0.41-0.60 moderate agreement, 0.61-0.80 good agreement and over 0.80 excellent agreement.
3. Results
3.1 Interobserver reliability
The interobserver agreement with regard to the presence of TSM artifacts was good with Kappa=0.696 (standard error 0.0482).
3.2 Occurrence and graduation of transient severe motion artifacts (TSM)
Transient severe motion artifacts were detected in 48.6% of the examinations (n=172). Most patients had minor artifacts with a motion score of 1 (22.9%, n=81). 18.4% (n=65) of the patients showed distinct artifacts (motion score 2) and 7.3% (n=26) severe artifacts (motion score 3).
MRI analysis revealed a higher frequency of TSM artifacts in the true arterial phase (58.8% patients with TSM) compared to early arterial phase (51.6%) and late arterial phase (42.1%). The frequencies of TSM artifacts within the different arterial phases are displayed in Figure 3. When looking at TSM graduation, image analysis revealed the highest occurrence of motion scores 1 and 2 in the late arterial phase with 50.6% and 43.1%, respectively. Motion score 1 was seen in 21.0% of the patients in the early arterial phase and in 28.4% in true arterial phase. 32.3% of the patients showed motion score 2 in the early arterial phase and 24.6% in true arterial phase. Severe artifacts (score 3) were mainly seen in the true arterial phase with 42.3%, and occurred in 38.5% in early arterial phase and 19.2% in late arterial phase. Both occurrence (p = 0.031) and TSM graduation (p = 0.012) were significantly associated with arterial phase timing.
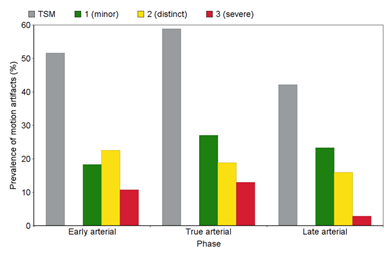
Figure 3: TSM frequency according to arterial phase timing. MR images after intravenous application of gadoxetate disodium revealed highest prevalence of TSM artifacts in the true arterial phase compared to early and late arterial phases. The percentage of the separate motion scores are displayed in color. Occurrence and TSM graduation are significantly associated with arterial phase timing (p = 0.031; p = 0.012).
3.3 Risk factor analysis
The occurrence and severity of TSM were analyzed with regard to underlying potential risk factors (Table 1). The data collected showed a significant correlation of TSM occurrence and BMI (p=0.001).
Occurrence of MR image degradation was not associated with age (p=0.832), gender (p=0.183), ascites (p=0.138), Quick’s value (p=0.497), international normalized ratio (INR) (p=0.448), activated partial thromboplastin time (aPTT) (p=0.783), creatinine (p=0.120), albumin (p=0.360), bilirubin (p=0.431), ALAT (p=0.910), ASAT (p=0.962) or gamma GT (p=0.095). Furthermore, no correlation could be seen between TSM and smoking status (p=0.821), anemia (p=0.417), allergy predisposition in general (p=0.215) or specifically against contrast agent or iodine (p=0.217), asthma (p=0.423), pleural effusion (p=0.082), COPD (p=0.426), hepatic encephalopathy (p=0.169), cholestasis (p=0.447) or GFR (p=0.618). Borderline significance was detected concerning graduation of liver cirrhosis and TSM occurrence (p=0.050).
3.4 Influence of prior TSM
From the 69 patients undergoing follow-up MR examination, motion artifacts were observed in 38 subjects (55.1%) in the first examination and 27 (39.1%) in the second examination. Nineteen patients (27.5%) displayed TSM in both examinations. A prior episode of TSM was a significant predictor for the occurrence of TSM (p=0.041).
4. Discussion
Our study investigates the occurrence of transient severe motion artifacts in MR imaging associated with acute transient dyspnea with respect to its causation and potential risk factors. Intravenous gadoxetate disodium administration leads to TSM artifacts in 48.6% of all cases with 25.7% showing distinct or severe image artifacts. This phenomenon, which could impede diagnostic accuracy of abdominal MR examinations, occurs especially in true arterial phase and is significantly associated with BMI and TSM occurrence in previous MR examinations.
In 2013, Davenport et al. described in a prospective study that intravenously administered gadoxetate disodium leads to significantly more subjective occurrence of acute transient dyspnea in patients compared to gadobenate dimeglumine (17% vs 2%) [9], which also belongs to the group of hepatobiliary contrast agents. Later on, they confirmed their results in a matched within-patient cohort study [15]. Pietryga et al. retrospectively found a TSM incidence of 10.7% after gadoxetate disodium application compared to 0.5% following gadobenate dimeglumine administration [10]. Kim et al. described an incidence of transient severe motion artifacts during arterial phase MRI of 12.9% after gadoxetate disodium administration, defining TSM as present if the motion score was 4 or above on a 5-point scale [16]. In our study we found a very high frequency of gadoxetate-related motion artifacts in 48.6% of all patients. With regard to the definition undertaken by other studies [12,16], however, which equals score 2 and 3 in our examination, diagnostically relevant TSM occurred in 25.7%, bringing our findings in the vicinity of previous studies by Motusugi et al. [12] and Davenport et al. [9].
Furthermore, Davenport et al. described this phenomenon to be associated with a severe degradation of arterial phase image data sets. Arterial phase enhancement, however, is crucial for the detection and characterization of hepatic focal lesions [11]. This finding has become a frequently discussed issue recently as the causation is still uncertain but of high clinical relevance, since image degradation impedes diagnostic accuracy. Our data fully support a significantly higher occurrence and severity of TSM artifacts, especially in the true arterial phase.
In their retrospective study Kim et al. [16] found that TSM occurrence was increased by history of TSM in prior MRI and allergy to iodinated contrast agent. However, in their conclusion TSM can only be poorly predicted on the basis of risk factors. Regarding other studies, TSM seems to be associated with obstructive pulmonary disease (COPD), volume of gadoxetate administration and prior episode of arterial phase motion in MR examination [9,10,13,14]. These findings are partly confirmed by our results. In our study we found an association of TSM with BMI, but not with the other analyzed risk factors, such as age, gender, history of allergies, smoking status, COPD, liver cirrhosis, hepatic encephalopathy, cholestasis, ascites, pleural effusion, anemia, Quick’s value, INR, aPTT, albumin, bilirubin, ALAT, ASAT, gamma GT, creatinine, GFR.
In order to improve diagnostic accuracy, some strategies are conceivable. Pietryga et al. showed in a retrospective study, that the use of single-breath-hold arterial phase acquisition provides adequate well-timed late hepatic arterial phase images in most patients with TSM [10]. This rapid imaging technique, therefore, may constitute an effective method to reduce the effect of TSM. Polanec et al. investigated the influence of different gadoxetic acid injection protocols and found that a power-injected administration of the contrast agent in 50% dilution with saline best minimized artifacts and provided a good arterial phase timing [17]. Another approach might be a better information or preparation of the patients themselves concerning the problem of acute transient dyspnea. In any case, further studies are necessary in order to reduce image degradation caused by TSM artifacts and improve patient well-being.
Our study has several limitations. First, the study design was retrospective. This, however, enabled the inclusion of a high number of patients. The Consensus report from the 7th International Forum of Liver Magnetic Resonance Imaging [18] suggested adaptation of volume of contrast agent to the patients’ weight and bolus-triggered scanning technique. Our study, however, included patient data before publication of this report and patient examination was undertaken in a clinical setting, so that volume of contrast agent was not adapted to the patients’ weight, but at a fixed dose and a fixed arterial phase time was used in order to enable higher practicability. This circumstance might be a reason for the relatively high frequency of TSM artifacts found in our study. However, the applied scanning protocol, in our opinion, better reflects the conditions in clinical routine settings. In addition, subjective patient complaints concerning dyspnea were not assessed. Furthermore, since patients were informed about the possibility of dyspnea occurrence in the preset of MR examination, they may have been more prone to experience this phenomenon. Likewise, the observers might have been sensitized to TSM occurrence while examining MR images. Both points might deliver an explanation of the relatively high TSM frequency detected in our study compared to other publications.
5. Conclusion
In conclusion, TSM artifacts in arterial phase contrast-enhanced MRI could influence diagnostic image quality in a high number of examinations. The occurrence and severity are depending on arterial phase timing and often seen in the true arterial phase. TSM artifacts are associated with BMI and prior episode of TSM in MR examination. First aim has, therefore, to be the reduction of such artifact-related image degradation to guarantee adequate image evaluation.
References
- Elsayes KM, Narra VR, Yin Y, et al. Focal hepatic lesions: diagnostic value of enhancement pattern approach with contrast-enhanced 3D gradient-echo MR imaging. Radiographics 25 (2005): 1299-1320.
- Chung YE, Kim MJ, Kim YE, et al. Characterization of incidental liver lesions: comparison of multidetector CT versus Gd-EOB-DTPA-enhanced MR imaging. PLoS One 8 (2013): e66141.
- Grazioli L, Bondioni MP, Haradome H, et al. Hepatocellular adenoma and focal nodular hyperplasia: value of gadoxetic acid-enhanced MR imaging in differential diagnosis. Radiology 262 (2012): 520-529.
- Mohajer K, Frydrychowicz A, Robbins JB, et al. Characterization of hepatic adenoma and focal nodular hyperplasia with gadoxetic acid. J Magn Reson Imaging 36 (2012): 686-696.
- Chen L, Zhang J, Zhang L, et al. Meta-analysis of gadoxetic acid disodium (Gd-EOB-DTPA)-enhanced magnetic resonance imaging for the detection of liver metastases. PLoS One 7 (2012): e48681.
- Zech CJ, Herrmann KA, Reiser MF, et al. MR imaging in patients with suspected liver metastases: value of liver-specific contrast agent Gd-EOB-DTPA. Magn Reson Med Sci 6 (2007): 43-52.
- Bashir MR, Gupta RT, Davenport MS, et al. Hepatocellular carcinoma in a North American population: does hepatobiliary MR imaging with Gd-EOB-DTPA improve sensitivity and confidence for diagnosis? J Magn Reson Imaging 37 (2013): 398-406.
- Fowler KJ, Brown JJ, Narra VR. Magnetic resonance imaging of focal liver lesions: approach to imaging diagnosis. Hepatology 54 (2011): 2227-2237.
- Davenport MS, Viglianti BL, Al-Hawary MM, et al. Comparison of acute transient dyspnea after intravenous administration of gadoxetate disodium and gadobenate dimeglumine: effect on arterial phase image quality. Radiology 266 (2013): 452-461.
- Pietryga JA, Burke LM, Marin D, et al. Respiratory motion artifact affecting hepatic arterial phase imaging with gadoxetate disodium: examination recovery with a multiple arterial phase acquisition. Radiology 271 (2014): 426-434.
- Bruix J, Sherman M. American Association for the Study of Liver D. Management of hepatocellular carcinoma: an update. Hepatology 53 (2011): 1020-1022.
- Motosugi U, Bannas P, Bookwalter CA, et al. An Investigation of Transient Severe Motion Related to Gadoxetic Acid-enhanced MR Imaging. Radiology 279 (2016): 93-102.
- Davenport MS, Bashir MR, Pietryga JA, et al. Dose-toxicity relationship of gadoxetate disodium and transient severe respiratory motion artifact. AJR Am J Roentgenol 203 (2014): 796-802.
- Bashir MR, Castelli P, Davenport MS, et al. Respiratory motion artifact affecting hepatic arterial phase MR imaging with gadoxetate disodium is more common in patients with a prior episode of arterial phase motion associated with gadoxetate disodium. Radiology 274 (2015): 141-148.
- Davenport MS, Caoili EM, Kaza RK, et al. Matched within-patient cohort study of transient arterial phase respiratory motion-related artifact in MR imaging of the liver: gadoxetate disodium versus gadobenate dimeglumine. Radiology 272 (2014): 123-131.
- Kim SY, Park SH, Wu EH, et al. Transient respiratory motion artifact during arterial phase MRI with gadoxetate disodium: risk factor analyses. AJR Am J Roentgenol 204 (2015): 1220-1227.
- Polanec SH, Bickel H, Baltzer PAT, et al. Respiratory motion artifacts during arterial phase imaging with gadoxetic acid: Can the injection protocol minimize this drawback? J Magn Reson Imaging 46 (2017): 1107-1114.
- Merkle EM, Zech CJ, Bartolozzi C, et al. Consensus report from the 7th International Forum for Liver Magnetic Resonance Imaging. Eur Radiol 26 (2016): 674-682.
